THE LIVING WORLD
Unit Six. Animal Life
25. The Path of Food Through the Animal Body
25.8. Accessory Digestive Organs
The Pancreas
The pancreas, a large gland situated near the junction of the stomach and the small intestine (see figure 25.5), is one of the accessory organs that contribute secretions to the digestive tract. Fluid from the pancreas is secreted into the duodenum through the pancreatic duct shown in figure 25.16. Note that the pancreatic duct joins with another duct, the common bile duct (discussed later), before entering the small intestine. This fluid contains a host of enzymes, including trypsin and chymotrypsin, which digest proteins. Inactive forms of these enzymes are released into the duodenum and are then activated by the enzymes of the intestine. Pancreatic fluid also contains pancreatic amylase, which digests starch; and lipase, which digests fats. Pancreatic enzymes digest proteins into smaller polypeptides, polysaccharides into shorter chains of sugars, and fat into free fatty acids and other products. The digestion of these molecules is then completed by the intestinal enzymes.
Pancreatic fluid also contains bicarbonate, which neutralizes the HCl from the stomach and gives the chyme in the duodenum a slightly alkaline pH. The digestive enzymes and bicarbonate are produced by clusters of secretory cells known as acini.
In addition to its exocrine role in digestion, the pancreas also functions as an endocrine gland, secreting several hormones into the blood that control the blood levels of glucose and other nutrients. These hormones are produced in the islets of Langerhans, clusters of endocrine cells scattered throughout the pancreas and shown in the enlarged view in figure 25.16. The two most important pancreatic hormones, insulin and glucagon, are discussed in chapters 26 and 30.
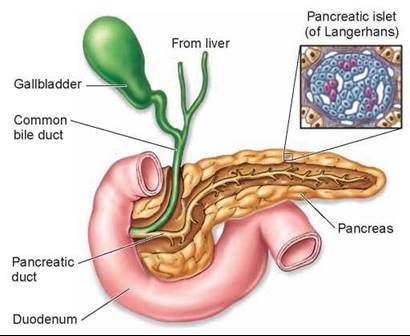
Figure 25.16. The pancreatic and bile ducts empty into the duodenum.
The Liver and Gallbladder
The liver is the largest internal organ of the body. In an adult human, the liver weighs about 1.5 kilograms and is the size of a football. The main exocrine secretion of the liver is bile, a fluid mixture consisting of bile pigments and bile salts that is delivered into the duodenum during the digestion of a meal.
The bile salts play a very important role in the digestion of fats. As explained earlier, fats are insoluble in water, and so they enter the intestine as drops within the watery chyme. The bile salts work like detergents, dispersing the large drops of fat into a fine suspension of smaller droplets. This breaking up, or emulsification, of the fat into droplets produces a greater surface area of fat upon which the lipase enzymes can act, and thus allows the digestion of fat to proceed more rapidly.
After it is produced in the liver, bile is stored and concentrated in the gallbladder (the green organ in figure 25.16). The arrival of fatty food in the duodenum triggers a neural and endocrine reflex that stimulates the gallbladder to contract, causing bile to be transported through the common bile duct and injected into the duodenum. If the bile duct is blocked by a gallstone (formed from a hardened precipitate of cholesterol), contraction of the gallbladder causes pain that is generally felt under the right scapula (shoulder blade).
The digestive system is highly specialized and involves the interactions of many different organs. Figure 25.17 overviews the different functional areas in the digestive system and the different organs involved. The colored circles indicate the primary areas of digestion and enzyme production: red for protein digestion, orange for carbohydrate digestion, green for fat digestion, and blue for nucleic acid digestion (not really discussed in this chapter as nucleic acids are not a major source of calories in the diet).
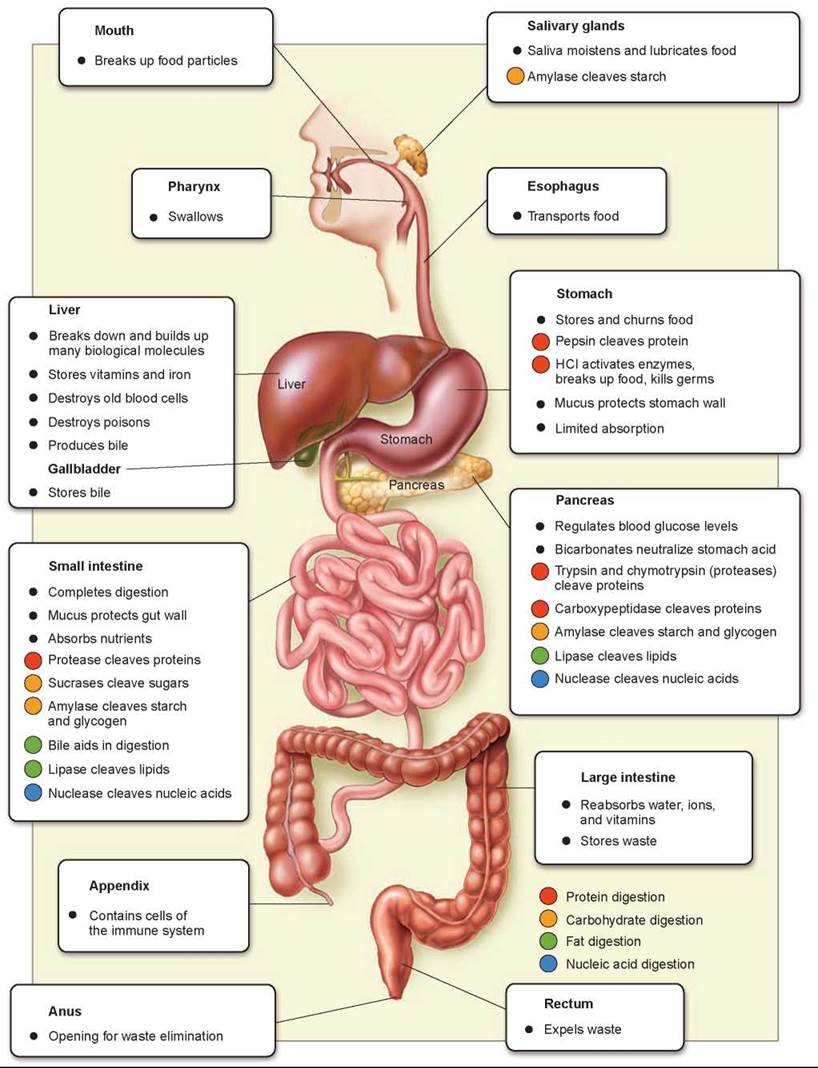
Figure 25.17. The organs of the digestive system and their functions.
The digestive system contains some dozen different organs that act on the food that is consumed, starting with the mouth and ending with the anus. All of these organs must work properly for the body to effectively obtain nutrients.
Regulatory Functions of the Liver
Because a large vein carries blood from the stomach and intestine directly to the liver, the liver is in a position to chemically modify the substances absorbed in the gastrointestinal tract before they reach the rest of the body. For example, ingested alcohol and other drugs are taken into liver cells and metabolized; this is why the liver is often damaged as a result of alcohol and drug abuse. The liver also removes toxins, pesticides, carcinogens, and other poisons, converting them into less-toxic forms. Also, excess amino acids that may be present in the blood are converted to glucose by liver enzymes. The first step in this conversion is the removal of the amino group (—NH2) from the amino acid, a process called deamination. Unlike plants, animals cannot reuse the nitrogen from these amino groups and must excrete it as nitrogenous waste. The product of amino acid deamination, ammonia (NH3), combines with carbon dioxide to form urea. The urea is released by the liver into the bloodstream, where—as you will learn in chapter 26—the kidneys subsequently remove it.
Key Learning Outcome 25.8. The pancreas secretes digestive enzymes and bicarbonate into the pancreatic duct. The liver produces bile, which is stored and concentrated in the gallbladder. The liver and the pancreatic hormones regulate blood glucose concentration.
Inquiry & Analtsis
Why Do Diabetics Excrete Glucose in Their Urine?
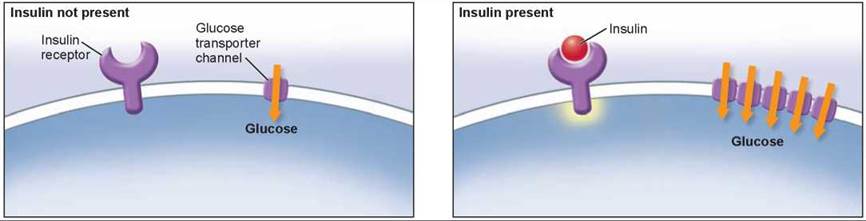
Late-onset diabetes is a serious and increasingly common disorder in which the body's cells lose their ability to respond to insulin, a hormone that is needed to trigger their uptake of glucose. As illustrated below, the binding of insulin to a receptor in the plasma membrane causes the rapid insertion of glucose transporter channels into the plasma membrane, allowing the cell to take up glucose.
In diabetics, however, glucose molecules accumulate in the blood while the body's cells starve for the lack of them. In mild cases, blood glucose levels rise to several times the normal value of 4 mM; in severe, untreated cases, blood glucose levels may become enormously elevated, up to 25 times the normal value. A characteristic symptom of even mild diabetes is the excretion of large amounts of glucose in the urine. The name of the disorder, diabetes mellitus, means "excessive secretion of sweet urine.” In normal individuals, by contrast, only trace amounts of glucose are excreted. The kidney very efficiently reabsorbs glucose molecules from the fluid passing through it. Why doesn't it do so in diabetic individuals?
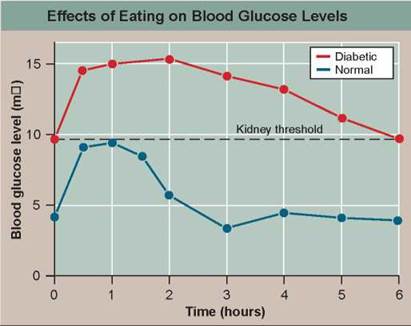
The graph on the upper right displays so-called glucose tolerance curves for a normal person (blue line) and a diabetic (red line). After a night without food, each individual drank a test dose of 100 grams of glucose dissolved in water. Blood glucose levels were then monitored at 30-minute and one-hour intervals. The dotted line indicates the kidney threshold, the maximum concentration of blood glucose molecules (about 10 mM) that the kidney is able to retrieve from the fluid passing through it when all of its glucose-transporting channels are being utilized full-bore.
1. Applying Concepts
a. Variable. In the graph, what is the dependent variable?
b. Reading a Curve. What is the immediate impact on the normal individual's blood glucose levels of consuming the test dose of glucose? How long does it take for the normal person's blood glucose level to return to the level before the test dose?
c. Comparing Curves. Is the impact any different for the diabetic person? How long does it take for the diabetic person's blood glucose levels to return to the level before the test dose?
2. Interpreting Data
a. Is there any point at which the normal individual's blood glucose levels exceed the kidney threshold?
b. Is there any point at which the diabetic individual's blood glucose levels do not exceed the kidney threshold?
3. Making Inferences
a. Why do you suppose the diabetic individual took so much longer to recover from the test dose?
b. Would you expect the normal individual to excrete glucose? Explain. The diabetic individual? Explain.
4. Drawing Conclusions. Why do diabetic individuals secrete sweet urine?
5. Further Analysis
a. If glucose molecules are being excreted in the urine, then they are not being converted to fatty acids for storage as fat. This would imply that severe diabetics would lose weight, even if on a high-calorie diet. How would you go about testing this prediction?
b. Denied glucose, the cells of a diabetic might be expected to turn in desperation to the cell's proteins as a food source. How might you test this hypothesis?
1. One-way passage of food through the digestive system of many animal groups allows
a. intracellular digestion.
b. specialization of different regions of the digestive system.
c. release of digestive enzymes into the gut.
d. extracellular digestion.
2. Organisms with longer digestive systems, which help break down difficult to digest food, are usually
a. herbivores.
b. carnivores.
c. omnivores.
d. detritivores.
3. The purpose of a gizzard, like teeth, is to
a. hold on to prey.
b. begin the chemical digestion of food.
c. release enzymes.
d. begin the physical digestion of food.
4. When a mammal swallows food, it is prevented from going up into the nasal cavity by the
a. esophagus.
b. tongue.
c. soft palate.
d. epiglottis.
5. The first site of protein digestion in the digestive system occurs in the
a. mouth.
b. esophagus.
c. stomach.
d. small intestine.
6. Which of the following statements is false?
a. Carnivores have a reduced or absent cecum.
b. Only ruminants are able to digest cellulose.
c. The human digestive system contains bacteria but is not able to gain nutritional value from the digestion of cellulose.
d. Ruminants are able to regurgitate food.
7. Most of the absorption of food molecules takes place in the
a. stomach.
b. liver.
c. small intestine.
d. large intestine.
8. The purpose of the villi and microvilli in the small intestine is to
a. neutralize stomach acid.
b. produce bile.
c. produce digestive enzymes.
d. increase the surface area of the small intestine for absorption of nutrients.
9. The primary function of the large intestine is
a. the breakdown and absorption of fats.
b. the absorption of water.
c. the concentration of solid wastes.
d. the absorption of vitamin C.
10. The _____ ecretes digestive enzymes and bicarbonate solution into the small intestine to aid digestion.
a. pancreas
b. liver
c. gallbladder
d. All of the above.