5 Steps to a 5: AP Biology 2017 (2016)
STEP 4
Review the Knowledge You Need to Score High
CHAPTER 16
Human Reproduction
IN THIS CHAPTER
Summary: This chapter discusses differences between the sexes, reproductive anatomy in humans, and how a sperm meets up with an egg to produce an embryo. The chapter concludes with a discussion of reproductive hormones.

Key Ideas
![]() Primary sex characteristics are the internal structures that assist in the process of procreation.
Primary sex characteristics are the internal structures that assist in the process of procreation.
![]() Secondary sex characteristics are the noticeable physical characteristics that differ between males and females.
Secondary sex characteristics are the noticeable physical characteristics that differ between males and females.
![]() Understand the concepts and the basics of embryology, but learn the specific details only if you have time.
Understand the concepts and the basics of embryology, but learn the specific details only if you have time.
![]() Take the time to learn which germ layer produces which structures (endoderm, mesoderm, and ectoderm).
Take the time to learn which germ layer produces which structures (endoderm, mesoderm, and ectoderm).
![]() Four extraembryonic structures necessary to the healthy development of an embryo: yolk sac, chorion, allantois, and amnion.
Four extraembryonic structures necessary to the healthy development of an embryo: yolk sac, chorion, allantois, and amnion.
![]() Factors in cellular differentiation: cytoplasmic distribution, induction, and homeotic genes.
Factors in cellular differentiation: cytoplasmic distribution, induction, and homeotic genes.
Introduction
Finally, the racy chapter you have all been waiting for: human reproduction! The topic was introduced in Chapter 9 in our discussion of cell division—meiosis and mitosis. This chapter begins by examining the differences between the sexes. A discussion of reproductive anatomy and the wild ride that a sperm must take to fertilize the female egg will follow. Then we will review the formation of gametes and the development of the embryo. Embryology is excessively detailed and not something you should get hung up on. You will want to know some details about development, but like glycolysis, the big picture is key. The AP Biology exam is not an embryology exam. Finally, the chapter concludes with a discussion of hormones and their effects on the reproductive system.
Sex Differences
What are the biologic differences between a man and a woman? For the purposes of this exam, you should keep in mind that one of the first distinctions is that boys have a Y chromosome in the nuclei of their cells, and girls do not. Another major difference lies in the sex characteristics. Primary sex characteristics are the structures that assist in the vital process of procreation. Among these are the testes, ovaries, and uterus. Secondary sex characteristics are the noticeable physical characteristics that differ between males and females such as facial hair, deepness of voice, breasts, and muscle distribution. These characteristics come into play as indicators of reproductive maturity to those of the opposite sex.
Anatomy
Since males tend to be a bit impatient, we will cover male anatomy first. The male sexual anatomy is designed for the delivery of sperm to the female reproductive system. Let’s follow the journey of a sperm from the beginning to the end.
Sperm’s “Wild Ride”
Here we stand in the testis. The male has two testes, located in a sac called the scrotum. This is the sperm factory—a portion of the testis called the seminiferous tubules is where the sperm are actually made. We return later to look at how these sperm are created. Notice in the other corner of the testis the structures called the interstitial cells. These are the structures that produce the hormones involved in the male reproductive system. Remember that the testis is the site of sperm and hormone production in the male reproductive system.
We are going to move along the production line to the epididymis —the coiled structure that extends from the testes. The epididymis is where the sperm completes its maturation and waits until it is called on to do its duty. From here, when called into action, the sperm moves through a tunnel called the vas deferens. Each epididymis connects to the urethra via this tunnel. The urethra is the passageway through which the sperm exits during ejaculation. Yes . . . that is indeed the same tunnel that the urine uses to get out . . . good observation in back.
We’re not done yet—let’s look at some other important players in this process (see also Figure 16.1 ). we are sure you have all heard about the prostate gland and how prostate cancer is currently one of the major cancers among men. But do you know what the prostate gland does? Here we are standing by this fine structure whose function in the male reproductive system is to add a basic (pH > 7) liquid to the mix to help neutralize any urine that may remain in the common urethral passage. It also helps to combat the acidity of the vaginal region of the female toward which the sperm is heading.
Follow us, everyone, more to see, more to see. . . . Here, on either side of us, are the structures called the seminal vesicles. These characters play an important role in the success of the sperm on its way to the female ovum. When the male ejaculates, the seminal vesicles dump fluids into the vas deferens to send along with the sperm. Think of the seminal vesicle as a convenience store. It provides three important goods to the sperm: energy by adding fructose; power to progress through the female reproductive system by adding prostaglandins (which stimulates uterine contraction); and mucus, which helps the sperm swim more effectively. The sperm is ready to enter the female reproductive system at this point, but before we observe the sperm as it does so, we want to take a quick tour of the female reproductive structures.
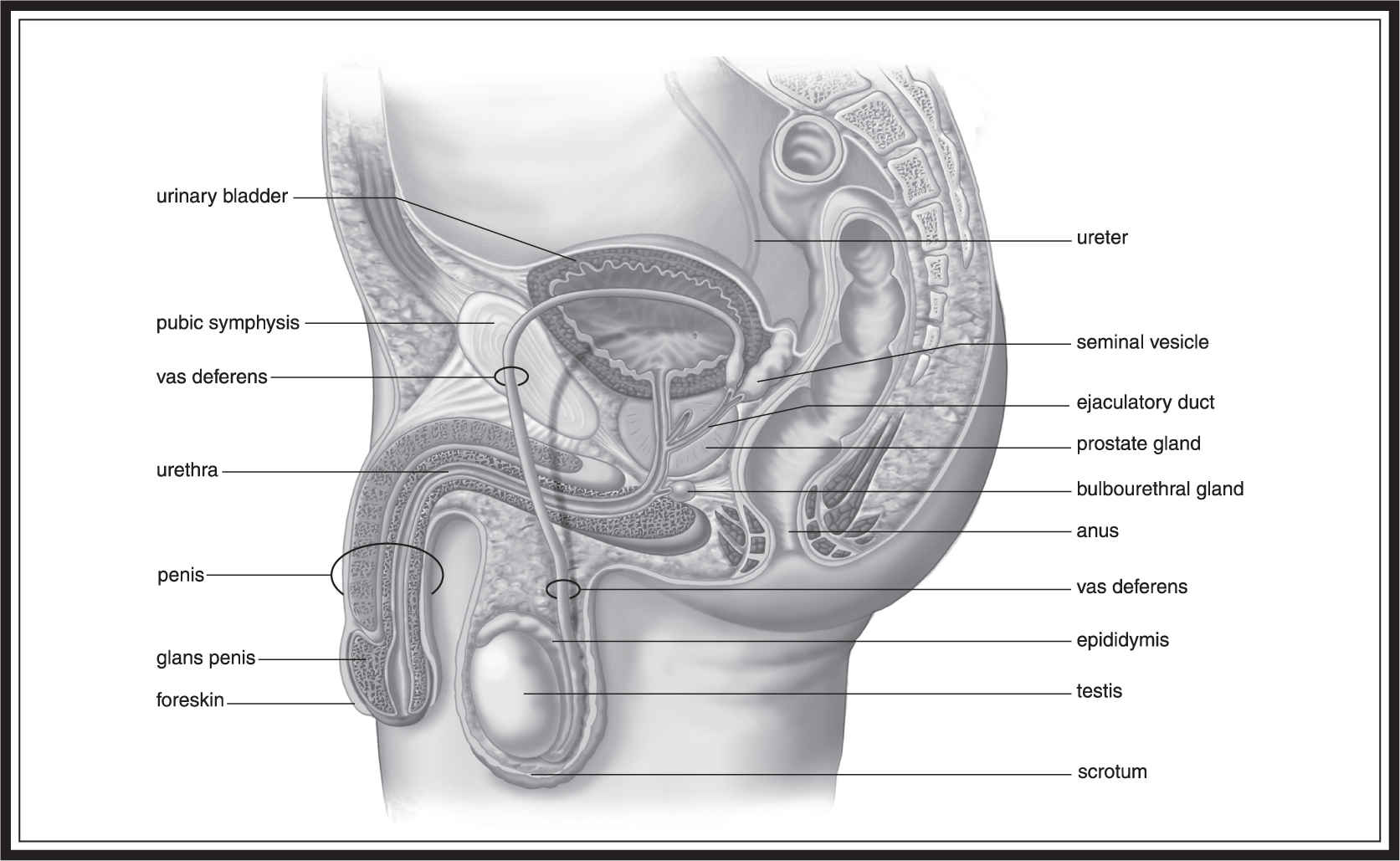
Figure 16.1 The human male reproductive system. (From Biology, 8th ed., by Sylvia S. Mader, © 1985, 1987, 1990, 1993, 1996, 1998, 2001, 2004 by the McGraw Hill Companies, Inc. Reproduced with permission of The McGraw-Hill Companies .)
We begin in the ovary, the site of egg production. Females have two ovaries—one on either side of the body. The egg leaves the ovary before it has fully matured and enters a structure called the oviduct. The oviduct is also known as the fallopian tube —you may be more familiar with that term. Eggs travel through here from the ovary to the uterus. When fertilized by an incoming sperm in the fallopian tube, after several days’ transit from the tube to the uterus, the egg usually attaches itself to the inner wall of the uterus, which is known as the endometrium. The uterus connects to the vaginal opening via a narrowed portion called the cervix. As we pass through the cervical area, we now find ourselves in the vagina, and it is here that the sperm enters the female reproductive system.
As the sperm enters, it must survive the different environment that the female body presents (Figure 16.2 ). Its task is to find its way to the fallopian tube, where it must meet the egg and penetrate its outer surface to achieve successful fertilization. The sperm works its way through the vaginal region, up through the cervix, through the uterus, and into the fallopian tube. Here, if the timing is appropriate, there will be a willing and waiting egg that is hoping to meet with a sperm to produce a new diploid zygote. After successful fertilization, the new happy couple moves down to the uterus and builds a nice house in the endometrium where it will develop into an embryo and remain until it is ready to be born.
The Formation of Gametes
In Chapter 9 , we discussed cell division and mentioned the process by which gametes are formed. Remember that the mechanics of gamete formation are different in women and men.
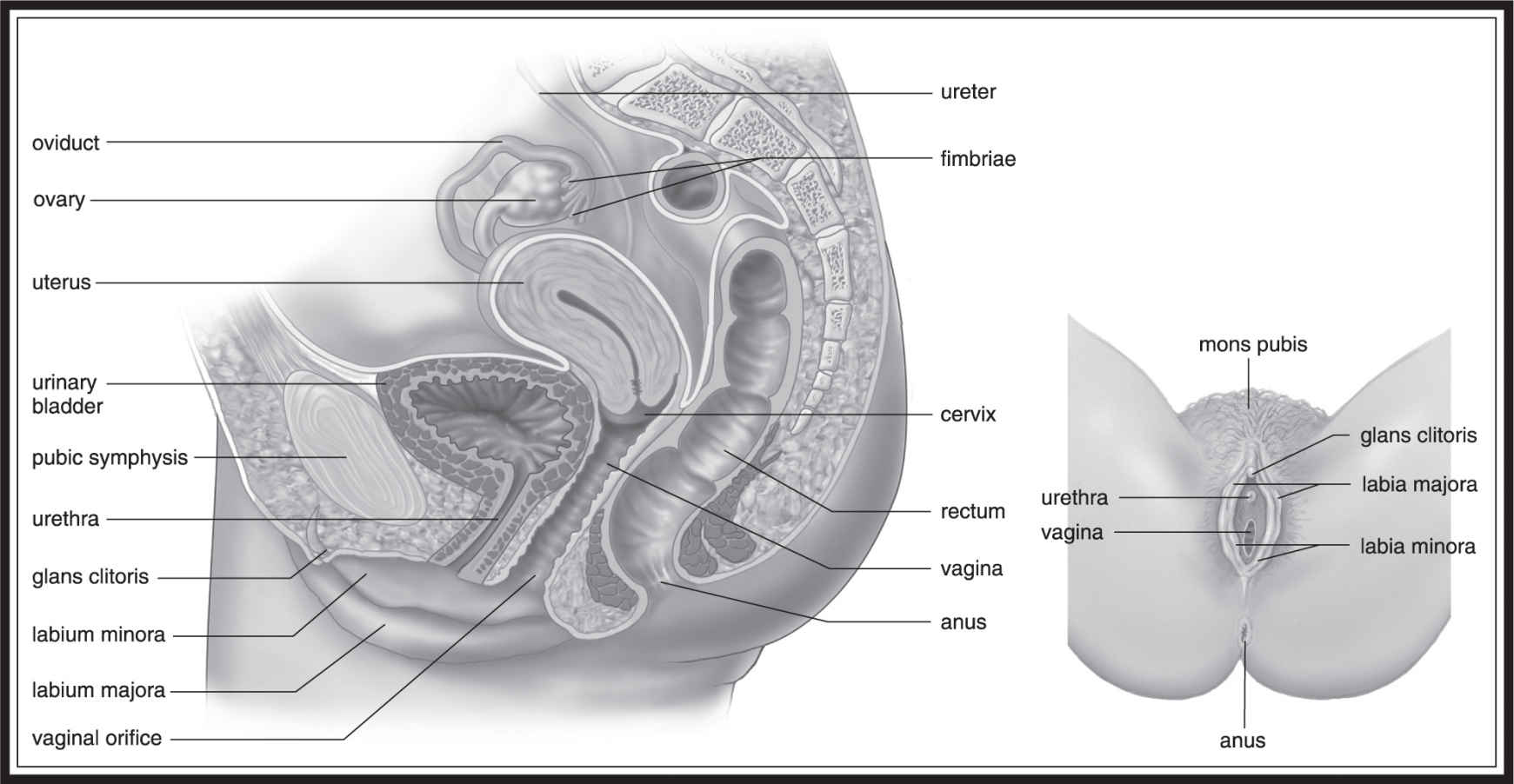
Figure 16.2 The human female reproductive system. (From Biology, 8th ed., by Sylvia S. Mader, © 1985, 1987, 1990, 1993, 1996, 1998, 2001, 2004 by the McGraw Hill Companies, Inc. Reproduced with permission of The McGraw-Hill Companies .)
Oogenesis
In women, the process of gamete formation is called oogenesis (Figure 16.3 ), which begins quite early—as the embryo develops. Mitotic division turns fetal cells into cells known as primary oocytes, which begin the process of meiosis and progress until prophase I; then the wait begins. The primary oocyte sits halted in prophase I until the host female enters puberty a number of years later. This is where the menstrual cycle begins. Each month, one of the primary oocytes frozen in the first act of meiosis returns to action and completes meiosis I. As we saw earlier, this phase produces a polar body, which has almost no cytoplasm and half of the genetic information of the parent cell, and a secondary oocyte, which has half the genetic information of the parent cell but the majority of its cytoplasm. This asymmetrical meiosis occurs because the developing embryo will need enough food, organelles, mitochondria, and other such structures for proper development.
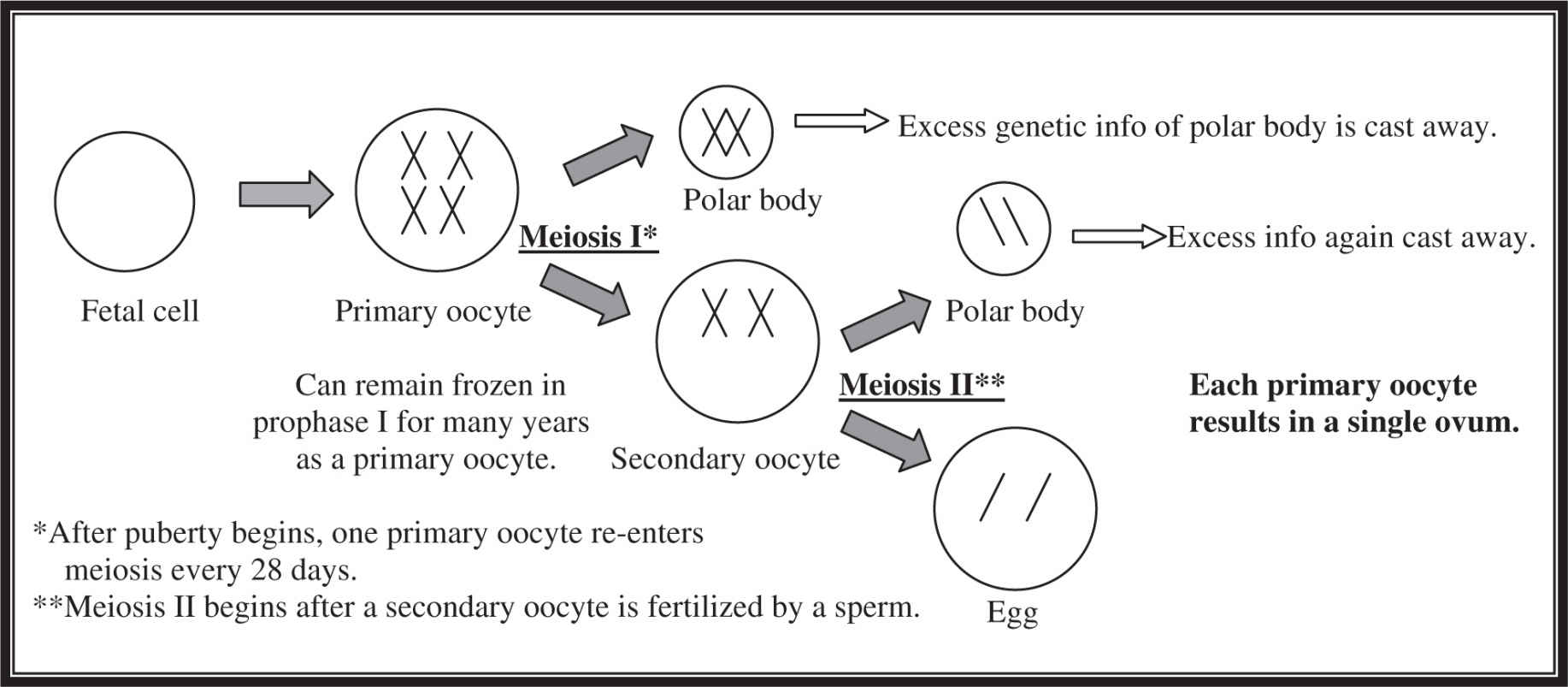
Figure 16.3 Oogenesis.
As the menstrual cycle continues, ovulation frees the secondary oocyte to travel into the fallopian tube to make its way down to the uterus. Fertilization usually occurs in the oviduct. If a successful fertilization occurs, the secondary oocyte enters meiosis II, again producing a polar body, as well as an egg that combines with the sperm to form a zygote.
What Is Important to Remember About This Oogenesis Business?
1. It doesn’t all happen at once for the ova. A primary oocyte could sit in the ovary for 40 years before completing the first stage of meiosis.
2. The beginning of each menstrual cycle causes a primary oocyte to resume meiosis I.
3. Oocytes undergo meiosis II only after fertilization with the sperm.
Spermatogenesis
For men, the process is less time-intensive. Let’s face it, guys . . . we are lazy. Less effort is better. Less time makes sense and leaves us more time and energy to watch sports and play video games. Males produce gametes through a process called spermatogenesis (Figure 16.4 ). Unlike females, males do not begin forming gametes until puberty. Spermatogenesis occurs in our old friends, the seminiferous tubules. Here, primary spermatocytes are produced by mitotic division. These primary spermatocytes undergo meiosis I to produce two secondary spermatocytes, which undergo meiosis II to produce four spermatids, which are immature sperm. After production, they enter the epididymis, where their waiting game begins and the maturation completes.
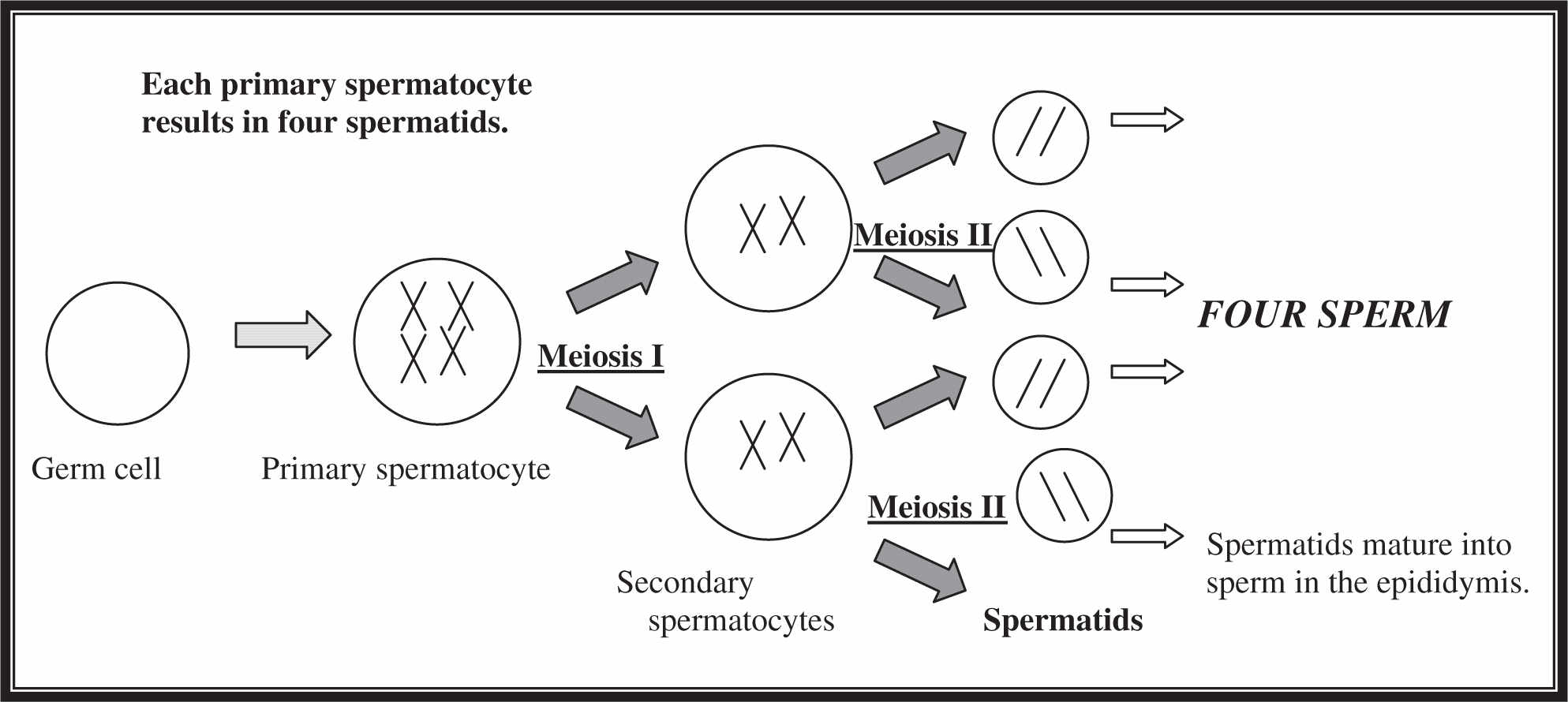
Figure 16.4 Spermatogenesis.
Embryonic Development
Embryology, the study of embryonic development, is a detailed and complex field. Fortunately, you are not taking an AP exam in embryology. Stick to the basics here and do not let the complex details bog you down. Follow along with the pretty pictures, and the review questions at the end of this chapter will give you a good indication of the level of detail required for success on the embryology questions of the AP Biology exam.
Cleavage
Embryonic development begins as soon as the egg is fertilized to produce a diploid zygote (2n ). This zygote then divides mitotically many times without increasing the zygote’s overall size. During these “cleavage” divisions(Figure 16.5 ), cytoplasm is distributed unevenly to the daughter cells but genetic information is distributed equally. This disparity exists because different cells will later produce different final products and the uneven distribution of cytoplasm plays a role in that process.
These cleavage divisions take a while in humans. The first three divisions take three days to complete. After the fourth division, the one cell has become 16 cells and is now called a morula. As it undergoes its next round of cell divisions, fluid fills the center of the morula to create the hollow-looking structure known to embryologists as the blastula. The fluid-filled cavity in the blastula is known as the blastocoel. Up to this point, much of the dividing has occurred as the zygote moves toward the uterus through the fallopian tube. By the time the blastula has formed, it has reached the uterus and has implanted on the wall. The blastula contains two parts: an inner cell mass, which later becomes the embryo, and a trophoblast, which becomes the placenta for the developing fetus and aids in attachment to the endometrium. The trophoblast also produces human chorionic gonadotropin (hCG), which maintains the endometrium by ensuring the continued production of progesterone and estrogen. The trophoblast later gives rise to the chorion, which we will discuss later.
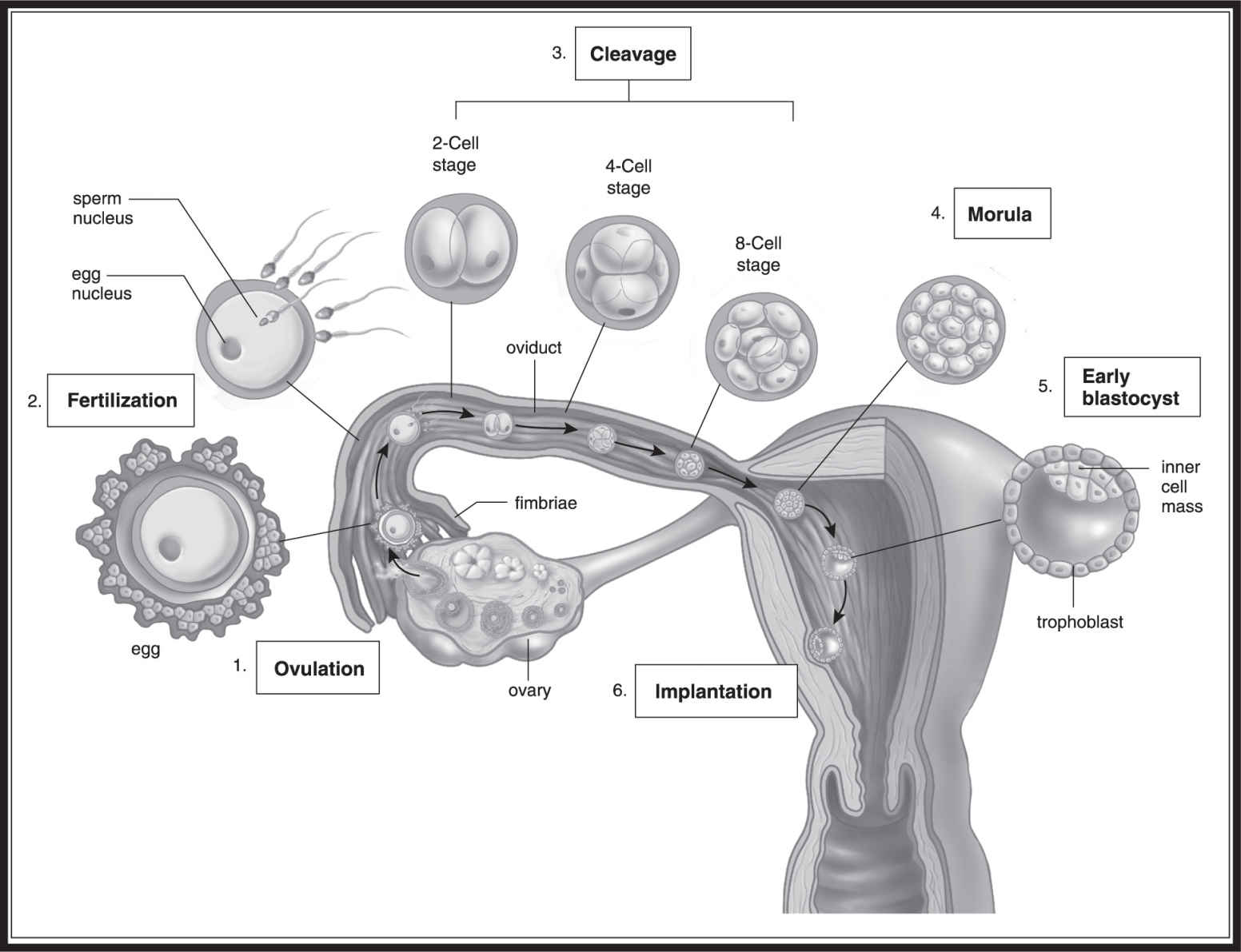
Figure 16.5 Embryonic cleavage divisions. (From Biology, 8th ed., by Sylvia S. Mader, © 1985, 1987, 1990, 1993, 1996, 1998, 2001, 2004 by the McGraw Hill Companies, Inc. Reproduced with permission of The McGraw-Hill Companies .)
Gastrulation
Okay, here’s where the discussion of embryology gets a little bit tricky. The next major stage of embryonic development after cleavage is gastrulation (also called morphogenesis ). During gastrulation, cells separate into three primary layers called germ layers, which eventually give rise to the different tissues of an adult.
Let’s look at this process in a bit more detail. (See also Figure 16.6 .) After the blastocyst attaches to the uterine wall, the inner cell mass divides into two major cell masses: the epiblast and the hypoblast. The hypoblast gives rise to the yolk sac, which produces the embryo’s first blood cells. In birds and reptiles, the yolk sac provides nutrients to the embryo. In humans, the placenta fills this role.
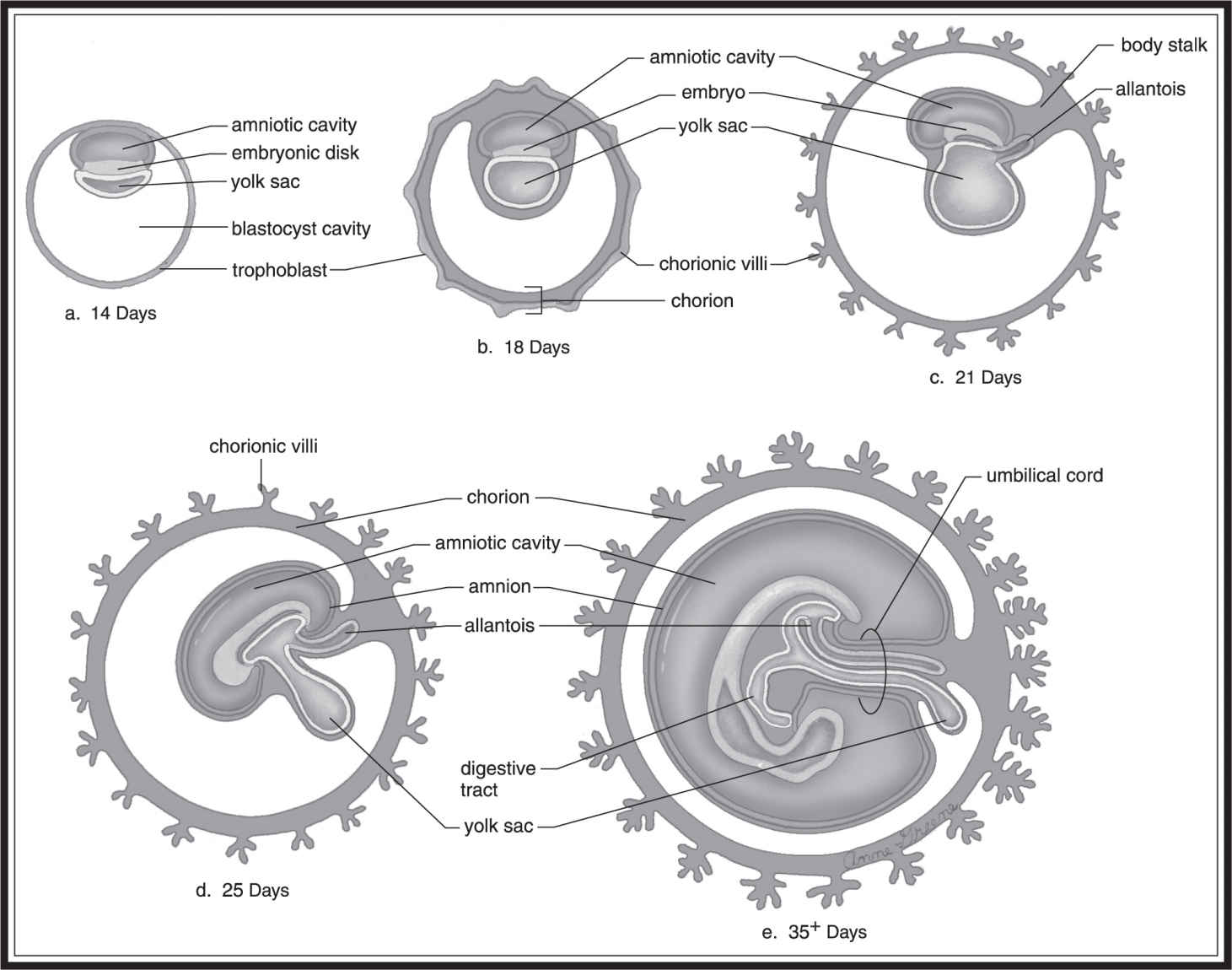
Figure 16.6 Components in the gastrulation process. (From Biology, 8th ed., by Sylvia S. Mader, © 1985, 1987, 1990, 1993, 1996, 1998, 2001, 2004 by the McGraw Hill Companies, Inc. Reproduced with permission of The McGraw-Hill Companies .)
The epiblast develops into the three germ layers of the embryo: the endoderm, the mesoderm, and the ectoderm.
Lindsay (12th grade): “Take the time to learn these. Know which layer produces what. It’s worth a point on the exam.”
Endoderm: inner germ layer; gives rise to the inner lining of the gut and the digestive system, liver, thyroid, lungs, and bladder.
Mesoderm: intermediate germ layer; gives rise to muscle, the circulatory system, reproductive system, excretory organs, bones, and connective tissues of the gut and exterior of the body.
Ectoderm: outer germ layer; gives rise to nervous system and skin, hair, and nails.
The separation of cells into the three primary germ layers sets the stage for cellular differentiation by which different cells develop into different structures with different functions. As far as this specific structural and functional differentiation is concerned, keep your focus on the basic development of the nervous system.
BIG IDEA 2.E.1
The timing and coordination of specific events are necessary for normal development .
The human nervous system derives primarily from the ectoderm, but the mesoderm contributes a structure known as the notochord, which serves to support the body. In vertebrates, this is present only in the embryo. The cells of the ectoderm that lie above the notochord form the neural plate, which becomes the neural groove, which eventually becomes the neural tube. This neural tube later gives rise to the central nervous system. One other term you should be familiar with in the development of the mammalian embryo is the somite, which gives rise to the muscles and vertebrae in mammals.
There are four extraembryonic structures necessary for the healthy development of the embryo:
1. Yolk sac: derived from the hypoblast; site of early blood cell creation in humans. Source of nutrients for bird and reptile embryos.
2. Chorion: formed from the trophoblast; the outer membrane of the embryo. Site of implantation onto the endometrium. Contributes to formation of the placenta in mammals.
3. Allantois: mammalian waste transporter. Later it becomes the umbilical cord, which carries oxygen, food, and wastes (including CO2 ) back and forth from placenta to embryo.
4. Amnion: formed from epiblast. Surrounds fluid-filled cushion that protects the developing embryo. Present in birds, lizards, and humans, to name only a few.
How Do Cells Know What to Do?
How do the various cells of the developing embryo differentiate into cells with different functions if they come from the same parent cell? As mentioned earlier, not every cell receives the same amount of cytoplasm during the cleavage divisions. It is thought that this asymmetric distribution of cytoplasm plays a role in the differentiation of the daughter cells. Cells containing different organelles or other cytoplasmic components are able to perform different functions. Two other factors, induction and homeotic genes, contribute to cellular differentiation.
Induction is the influence of one group of cells on the development of another through physical contact or chemical signaling. Just in case you are asked to write an essay on induction, it is good to know a bit about the experiments of the German embryologist Hans Spemann. His experiments revealed that the notochord induces cells of the dorsal ectoderm to develop into the neural plate. When cells from the notochord of an embryo are transplanted to a different place near the ectoderm, the neural plate will develop in the new location. The cells from the notochord region act as “project directors,” telling the ectoderm where to produce the neural tube and central nervous system.
BIG IDEA 3.B.2
Signal transmission by homeotic genes mediates cell function .
Homeotic genes regulate or “direct” the body plan of organisms. For example, a fly’s homeotic genes help determine how its segments will develop and which appendages should grow from each segment. Scientists interfering with the development of these poor creatures have found that mutations in these genes can lead to the production of too many wings, legs in the wrong place, and other unfortunate abnormalities. The DNA sequence of a homeotic gene that tells the cell where to put things is called the homeobox. It is similar from organism to organism and has been found to exist in a variety of organisms—birds, humans, fish, and frogs.


The Influence of Hormones
In Chapter 15 we discussed the hormones that will be included in the AP exam. A few of those play a critical role in human sexual development and reproduction. The hormones involved include LH, FSH, estrogen, progesterone, and testosterone. You do not need to know every detail, just the big picture. As proper etiquette requires, ladies first. Let’s talk about the hormones involved in the female reproductive system.
BIG IDEA 2.C.1
Organisms use feedback mechanisms .
Estrogen and progesterone continually circulate in the female bloodstream, and the hypothalamus monitors these levels to determine when to release certain hormones. For example, when the concentrations of estrogen and progesterone are low, the hypothalamus secretes GnRH, which travels to the anterior pituitary gland to induce the release of FSH and LH. (Just to remind you, FSH is follicle-stimulating hormone, LH is luteinizing hormone, and GnRH is gonadotropin-releasing hormone.) FSH induces the development of the follicle that contains the primary oocyte during its development. It also causes the follicular cells to release estrogen, which triggers the hypothalamus to dump more GnRH into the system. This GnRH acts on the anterior pituitary to produce the LH surge that initiates ovulation —the release of a secondary oocyte from the ovary.
This LH surge causes further release of estrogen and progesterone from the follicular cells, which have now become a structure called the corpus luteum. The corpus luteum induces the thickening of the endometrium, the site of future fertilized egg attachment. At this point in the cycle, the levels of estrogen and progesterone elevate enough to make the hypothalamus cut off production of GnRH so that the LH and FSH levels drop back down. (This decrease in production of LH and FSH, due to high levels of estrogen and progesterone, is called negative feedback. ) Here lies a fork in the road for the female reproductive system. If fertilization has occurred in the fallopian tube, and if the blastocyst attaches successfully to the uterine wall, hCG will be secreted, which works to keep the corpus luteum alive. As a result, the levels of estrogen and progesterone remain high and keep the endometrium intact. If a blastocyst does not implant, production of estrogen or progesterone from the corpus luteum will cease, causing the destruction of the endometrium.
This cycle of hormonal activity is known as the menstrual cycle . A woman repeats this cycle, on an average, every 28 days. This cycle is disrupted when a sperm fertilizes the egg and successful implantation occurs. During pregnancy, hormone levels in the body change as a result of the presence of the corpus luteum, which maintains constant levels of estrogen and progesterone. This halts ovulation for the remainder of the pregnancy. If a sperm does not fertilize the egg, however, negative feedback reduces the levels of LH and FSH and leads to the deterioration of the endometrium, which then sloughs off during the menstrual cycle. When the levels of hormones circulating in the blood drop low enough, the cycle will begin again with the release of LH and FSH, culminating in the next menstrual cycle.
In males, as in females, GnRH causes the pituitary to release LH and FSH. The LH causes the continual production of testosterone in men. FSH and testosterone work together to assist the maturation of sperm produced during spermatogenesis. The baseline levels of testosterone are vital to the development of secondary sex characteristics in men.
![]() Review Questions
Review Questions
For questions 1–4, please use the following answer selections:
A. Blastula
B. Morula
C. Somite
D. Trophoblast
E. Hypoblast
1 . After the fourth cleavage division, the one cell has become 16 cells and is now given this name.
2 . Gives rise to the yolk sac of the developing embryo.
3 . Forms the placenta for the developing fetus.
4 . Gives rise to the muscles and vertebrae in mammals.
5 . Which of the following is not a structure involved in the ejaculation of sperm?
A. Epididymis
B. Seminal vesicles
C. Cervix
D. Vas deferens
E. Interstitial cells
6 . Which of the following hormones feeds back to cause the LH surge of the menstrual cycle?
A. Estrogen
B. Progesterone
C. FSH
D. LH
E. GnRH
7 . Which of the following structures is not derived from the endoderm of a developing embryo?
A. Liver
B. Thyroid
C. Heart
D. Bladder
E. Lungs
For questions 8–11, please use the following answer selections:
A. FSH
B. LH
C. Testosterone
D. Estrogen
E. hCG
8 . This hormone ultimately triggers ovulation in females.
9 . This hormone is produced in the interstitial cells.
10 . This hormone is responsible for maintenance of the corpus luteum during early pregnancy.
11 . This hormone works with testosterone to assist in maturation of the sperm produced during spermatogenesis.
12 . Which structure is usually the site of fertilization in humans?
A. Cervix
B. Uterus
C. Oviduct
D. Ovary
E. Endometrium
13 . Which of the following explains the mechanism by which the neural plate develops in human embryos?
A. Induced fit
B. Homeotic gene determination
C. Induction
D. Negative feedback
E. Gastrulation
![]() Answers and Explanations
Answers and Explanations
1 . B
2 . E
3 . D
4 . C
5 . C —The cervix is the only structure listed here that is a part of the female reproductive anatomy. The epididymis is the site of sperm storage and maturation while it awaits ejaculation. The seminal vesicles are the convenience store, providing the sperm with the necessary materials to survive its journey from ejaculation to fertilization. The vas deferens is the tunnel connecting the epididymis to the urethra. The interstitial cells are the cells that produce the hormones, such as testosterone, vital to male sexual function.
6 . A —At the beginning of each menstrual cycle, GnRH is released from the hypothalamus and travels to the anterior pituitary gland to induce the release of FSH and LH. FSH induces the development of the follicle and causes the follicle to release estrogen, which triggers the hypothalamus to dump more GnRH into the system. This GnRH acts on the anterior pituitary to produce the LH surge, which triggers ovulation. The estrogen feeds back to the hypothalamus to induce the release of large amounts of LH that ultimately lead to increased production of even more estrogen.
7 . C —The heart is part of the circulatory system and is derived from the mesoderm.
8 . B
9 . C
10 . E
11 . A
12 . C —The oviduct, or the fallopian tube, is where fertilization normally occurs in humans. The uterus is where implantation and development of the embryo normally occur. The embryo usually implants on the wall of the uterus—the endometrium. The cervix is the narrow pathway from the uterus to the vaginal opening. The ovary is the site of egg production.
13 . C —Remember induction. It is a concept loved by the AP Biology exam writers. Induction is the ability of cells to influence the development of other cells by either physical contact or chemical signals. Homeotic genes are genes that determine how segments of an organism will develop. Induced fit is how enzymes and substrates interact. Gastrulation is the separation of the cells of the developing embryo into the three primary germ layers. Negative feedback is the reduction in production of a substance due to high levels already present in circulation.
![]() Rapid Review
Rapid Review
Quickly review the following terms:
Primary sex characteristics: sexual organs that assist in reproduction.
Secondary sex characteristics: physical characteristics that differ between men and women.
Male anatomy:
• Two testes enclosed in the scrotum— site of sperm and testosterone production, which occurs in the seminiferous tubules.
• Interstitial cells, which produce testosterone involved in male reproduction.
• Epididymis, a coiled structure where sperm completes maturation.
• Vas deferens, a tunnel that connects epididymis to urethra, where sperm and urine are ejected.
• Prostate gland, a gland that adds basic liquid to neutralize urine acidity so that sperm don’t die on the way out.
• Seminal vesicles, glands that produce fluid to help sperm in various ways (adds energy, power, help with swimming).
Female anatomy:
• Ovary: site of egg, estrogen, and progesterone production; eggs move from here through the fallopian tube (oviduct ) to the uterus, which is where a fertilized egg attaches to the endometrium.
• Cervix: narrowed portion of the uterus that connects the uterus and vagina.
Formation of gametes:
• Oogenesis: formation of eggs; starts in embryonic development and doesn’t finish for each egg until that egg matures during a menstrual cycle (hence, an egg could wait 40 years to finish maturation).
• Meiosis II: oocytes undergo this process only after fertilization by a sperm in the oviduct.
• Spermatogenesis: one primary spermatocyte produces four spermatids, which mature in the epididymis.
Embryology (the study of embryonic development):
• Cleavage divisions: mitotic divisions that occur as soon as a zygote is formed; these divisions don’t increase the overall size of the zygote; cytoplasm distributed unevenly, genetic information distributed evenly.
• Morula: what we call the zygote when it has become 16 cells.
• Blastula: when a zygote has become 32 cells—by this time it is implanted in the endometrial wall.
• Gastrulation: cells separate into three germ layers, which give rise to different adult tissues.
Endoderm: gives rise to inner layer; lining of gut and digestive system, liver, lungs.
Mesoderm: gives rise to intermediate layer; muscle, circulation, bones, reproductive system.
Ectoderm: gives rise to outer layer; nervous system, skin, hair, nails.
Factors in cellular differentiation:
1. Cytoplasmic distribution: different amounts of cytoplasm signal different structures.
2. Induction: ability of one group of cells to influence another.
3. Homeotic genes: regulate or direct the body plan of organisms.
Hormones play a major role in directing reproductive development and reproduction:
• FSH: stimulates oogenesis in females and spermatogenesis in males. Creates follicle that surrounds the primary oocyte during development.
• LH: stimulates the ovulation and production of estrogen and progesterone in females; stimulates production of testosterone and sperm in males. Surge in this hormone triggers ovulation (release of secondary oocyte from ovary).
• GnRH: causes pituitary to release LH and FSH.
• Progesterone and estrogen: female sex hormones involved in reproduction.
• Testosterone: male sex hormone involved in reproduction.
CHAPTER 16
Human Reproduction
1 . Which of the following structures is derived from the endoderm?
(A) Skin
(B) Nails
(C) Heart
(D) Bladder
2 . Which of the following structures is derived from the mesoderm?
(A) Skin
(B) Nails
(C) Heart
(D) Bladder
3 . Which of the following is an extraembryonic structure that is derived from the hypoblast and is the site of early blood cell creation in humans?
(A) Yolk sac
(B) Chorion
(C) Allantois
(D) Amnion
4 . Which kind of genes determine how segments of an organism will develop?
(A) Dimorphic
(B) Homeotic
(C) Heterotrophic
(D) Dysplastic
![]() Answers and Explanations
Answers and Explanations
1 . D
2 . C
3 . A —The chorion is formed from the trophoblast and contributes to the formation of the placenta in mammals. The allantois becomes the umbilical cord. The amnion is formed from epiblast.
4 . B —Homeotic genes regulate, or “direct,” the body plan of organisms. For example, a fly’s homeotic genes help determine how its segments will develop and which appendages should grow from each segment.