CONCEPTS IN BIOLOGY
PART VI. PHYSIOLOGICAL PROCESSES
24. Materials Exchange in the Body
24.2. Circulation: The Cardiovascular System
The cardiovascular system of all vertebrates, including humans, is the organ system that pumps blood around the body; and consists of the blood, heart, and blood vessels. Blood is the fluid tissue that assists in the transport of materials and heat. The heart is a muscular pump that forces the blood from one part of the body to another. The heart pumps blood into blood vessels. Arteries are the vessels that carry blood away from the heart and distribute it to the organs. The blood flows through successively smaller arteries until it reaches tiny vessels called capillaries. Capillaries are the thinnest blood vessels where exchange of materials between the blood and tissues that surround the vessels takes place. The blood flows from the capillaries into veins, the vessels that return blood to the heart.
The Nature of Blood
Blood is a fluid tissue consisting of several kinds of cells and platelets, called formed elements, suspended in a watery solution called plasma (table 24.1). This fluid plasma also contains many kinds of dissolved molecules, including nutrients, wastes, salts and proteins. The blood’s primary function is to transport molecules, cells, and heat from one part of the body to another. The major kinds of molecules distributed by the blood are respiratory gases (oxygen and carbon dioxide), nutrients of various kinds, waste products, disease-fighting cells and antibodies, and chemical messengers (hormones). Also, substances in the blood are capable of forming clots or plugs to prevent blood loss.
Heat is generated by metabolic activities and must be removed from the body. To handle excess body heat, blood is moved through the vessels to the surface of the body, where it can be radiated away. In addition, humans and some other animals have the ability to sweat. The evaporation of sweat (released from glands in the skin) from the body surface also gets rid of excess heat. If the body is losing heat too rapidly, blood is moved away from the skin, and metabolic heat is conserved. Vigorous exercise produces an excess of heat, so that, even in cold weather, blood is moved to the skin and the skin feels hot.
TABLE 24.1. Components of Blood
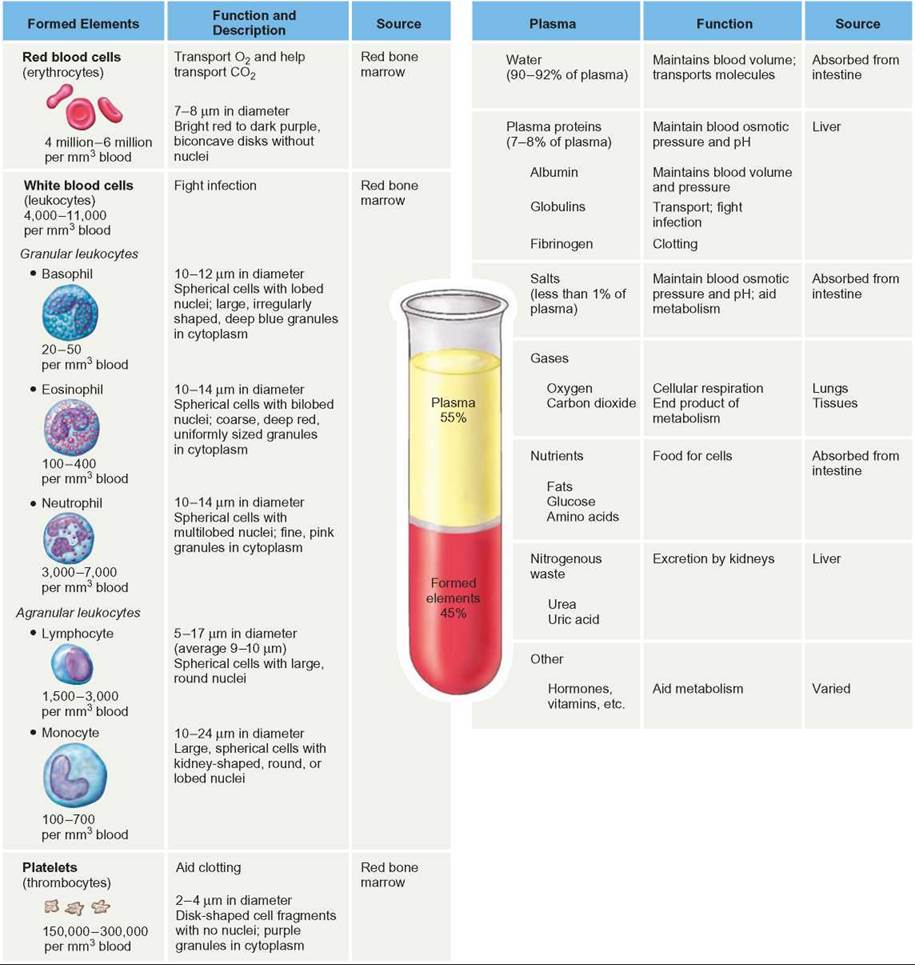
Formed Elements
The most numerous formed elements are red blood cells (rbcs), which are small, disk-shaped cells that lack a nucleus. Their primary function is to allow the blood to distribute respiratory gases efficiently (Outlooks 24.1). RBCs have the iron-containing pigment hemoglobin, the protein molecule to which oxygen molecules bind readily. Red blood cells transport oxygen around the body attached to their hemoglobin molecules. Very little oxygen is carried as free, dissolved oxygen in the plasma.
Because hemoglobin is inside red blood cells, some health problems can be diagnosed by counting the number of red blood cells a person has. If the number is low, the person’s blood cannot carry oxygen efficiently and he or she tires easily. Anemia is a condition in which a person has reduced oxygen-carrying capacity. Anemia can also result when a person does not consume enough iron. Because iron is a central atom in hemoglobin molecules, people with an iron deficiency cannot manufacture sufficient hemoglobin; they can be anemic even if their number of red blood cells is normal.
Red blood cells are also important in the transport of carbon dioxide. Carbon dioxide is a result of the normal aerobic cellular respiration of food materials in the cells of the body. If carbon dioxide is not eliminated, it causes the blood to become more acidic (lowers its pH), eventually resulting in death. Carbon dioxide can be carried in the blood in three forms: about 7% is dissolved in the plasma, about 23% is carried attached to hemoglobin molecules, and 70% is carried as bicarbonate ions. The enzyme carbonic anhydrase in red blood cells helps convert carbon dioxide into bicarbonate ions (HCO3-), which can be carried as dissolved ions in the plasma of the blood. The following reversible chemical equation shows the changes that occur.
![]()
When the blood reaches the lungs, dissolved carbon dioxide is lost from the plasma, and carbon dioxide is released from the hemoglobin molecules. In addition, the bicarbonate ions reenter the red blood cells and can be converted back into molecular carbon dioxide by the same enzyme-assisted process that converts carbon dioxide to bicarbonate ions. The importance of this mechanism will be discussed in the section “Gas Exchange: The Respiratory System.”
White blood cells (wbcs), also called leukocytes, are formed elements in the blood that lack hemoglobin and are involved in defending the body from disease-causing agents. There are several kinds of wbcs that vary in size and function (see table 24.1). When wbcs are stained with dyes and viewed under the microscope, they all have a conspicuous nucleus, and some kinds have granules in their cytoplasm. The granule-containing leukocytes are basophils, eosinophils, and neutrophils. Those without granules are lymphocytes and monocytes. All of these cells have specific roles to play in protecting the body from bacteria, viruses, fungi, worms, toxins, and cancer cells.
Platelets (also called thrombocytes), another kind of formed element in the blood, are actually fragments of a specific kind of white blood cell. Platelets are important in blood clotting. About 200 billion are formed each day. When a wound occurs, they collect at the site of the wound, where they form an initial plug and release compounds that cause other platelets to collect at the site. They also release compounds that begin a series of reactions among chemicals in the plasma called clotting factors. There are at least 13 known clotting factors. The interactions of the various clotting factors ultimately result in the formation of fibers that trap platelets and blood cells and form a stronger plug than the initial platelet plug in the opening of the wound. Blood clots at the site of wounds are sometimes called scabs. They have a reddish or brownish color because they contain the leftovers of destroyed rbcs. Scabs are short-lived and are replaced by healthy tissue as the wound heals.
Plasma
Recall that plasma is the liquid part of the blood, consisting of water and dissolved materials, such as a variety of salts, proteins, nutrients, and waste products. Salts serve as buffers that help maintain the blood’s pH. They also play a role in maintaining the proper osmotic balance between the blood and surrounding tissues.
Plasma proteins perform a variety of functions. The most plentiful plasma protein is albumin. It makes up about 60% of all plasma proteins, is the primary molecule involved in maintaining osmotic balance, and is also important in maintaining the proper blood pH. Albumin also assists in the transport of compounds that enter the blood (Outlooks 24.2). Globulins (antibodies), many of the clotting factors, regulatory proteins, and many other proteins circulate freely in the plasma.
Because the blood is under pressure from the pumping of the heart, it is normal for some fluid to leak from the smallest blood vessels (capillaries) into the surrounding tissues. This fluid that bathes the body’s cells is called tissue fluid. It is similar to plasma but contains less dissolved albumin because the proteins are too large to pass through the walls of the capillaries, whereas salts can pass. Although the tissue fluid carries nutrients and other materials to the cells, it must be returned to the circulatory system, or swelling will occur. The albumin in the blood maintains the osmotic balance such that tissue fluid tends to return to the circulatory system.
In addition to water, salts, and proteins, plasma carries a variety of other important molecules. Nutrient molecules from the gut are carried to other locations, where they are modified, metabolized, or incorporated into cell structures. Amino acids and simple sugars are carried as dissolved molecules in the blood. Lipids, which are not water-soluble, are combined with proteins and carried as suspended particles called lipoproteins. Some organs manufacture or modify molecules for use elsewhere; therefore, they must constantly receive raw materials and distribute their products to the cells that need them through the blood. In addition, many kinds of hormones are produced by the brain, reproductive organs, digestive organs, and glands. These are secreted into the bloodstream and transported throughout the body. Tissues with appropriate receptors bind to these molecules and respond to these chemical messengers.
OUTLOOKS 24.1
Blood Doping
The use of performance-enhancing techniques and drugs in sports is not new. For example, one way to increase the amount of oxygen available to muscles is to inhale higher concentrations of the gas. You may have seen athletes breathing from an oxygen tank while on the sidelines during a sporting event. Another approach to increasing the amount of available oxygen is to increase the number of oxygen-carrying red blood cells. This can be accomplished in several ways. An athlete can have a pint of his or her blood removed and put into storage about three weeks before an event. During that time, the athlete's body replaces the removed red blood cells. Just before the event, the "donated" blood is transfused back into the athlete, increasing the total number of red blood cells. This method of enhancing an athlete's performance has been banned because it is considered to give an unfair advantage and because there can be dangerous side-effects.
Another technique involves artificially stimulating the body to produce more red blood cells by injecting the protein hormone erythropoietin, commonly referred as EPO. The kidney produces EPO, and after it is released into the bloodstream, it binds to receptors on stem cells in the red bone marrow, where it stimulates the production of new red blood cells. The increased red blood cell production in turn increases the oxygen-carrying capacity of the blood. This fact has resulted in some members of the athletic community using EPO as a performance-enhancing drug to artificially increase the amount of red blood cells.
Still another method of increasing available oxygen is the use of synthetic oxygen carriers, such as hemoglobin-based oxygen carriers (HBOCs) or perfluorocarbons (PFCs). These are purified proteins or chemicals that have the ability to carry oxygen. They can be useful in emergencies when human blood is not available, when the risk of blood infection is high, or when there is not enough time to properly cross-match donated blood with a recipient. However, their misuse for doping carries the risk of cardiovascular disease, in addition to other side-effects such as stroke, heart attack, or blood clot.
The use of blood transfusions, EPO, and synthetic oxygen carriers is prohibited under the World Anti-Doping Agency's (WADA) List of Prohibited Substances and Methods.

OUTLOOKS 24.2
Newborn Jaundice
Albumin transports bilirubin, a yellowish molecule that is a breakdown product of hemoglobin from destroyed rbcs. Normally, bilirubin is transported to the liver, where it is destroyed and the broken-down products are released with the bile into the intestine. However, some newborns become jaundiced (a yellowing of the skin and whites of the eyes) because their liver has not matured enough to do this important job. If bilirubin is allowed to accumulate in their blood, jaundiced babies can develop deafness, cerebral palsy, or brain damage. Placing babies under a special ultraviolet ("bili") light helps relieve the problem. The light has a wavelength that helps break down the bilirubin to a form that can be eliminated through the kidneys until the baby's liver matures and can adequately handle the bilirubin.
The Heart
Blood can perform its transportation function only if it moves. The heart is responsible for providing the energy to pump the blood throughout the body. For a fluid to flow through a tube, there must be a pressure difference between the two ends of the tube; water flows through pipes because it is under pressure. Because the pressure is higher behind a faucet than at the spout, water flows from the spout when the faucet is opened. The circulatory system can be understood from the same point of view. The heart is the muscular pump that provides the pressure necessary to propel the blood throughout the body. It must continue its cycle of contraction and relaxation or the blood stops flowing and the body’s cells cannot obtain nutrients or get rid of wastes. Some cells, such as brain cells, are extremely sensitive to interruptions in the flow of blood, because they require a constant supply of glucose and oxygen. Others, such as muscle cells and skin cells, are much better able to withstand temporary interruptions of blood flow.
The hearts of humans, other mammals, and birds consist of four chambers and four sets of valves, that work together to ensure that blood flows in one direction only. Two of these chambers, the right and left atria (singular, atrium), are relatively thin-walled structures that collect blood from the major veins and empty it into the larger, more muscular ventricles (figure 24.1). Most of the blood is drawn in from the atria to the ventricles by the lowered pressure produced within the ventricles as they relax. The contraction of the thin-walled atria helps empty them more completely.
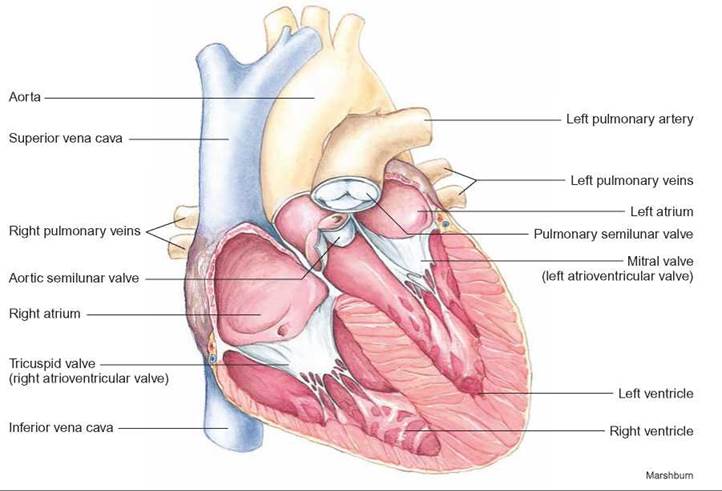
FIGURE 24.1. The Anatomy of the Heart
The heart consists of two thin-walled chambers, called atria, which contract to force blood into the two muscular ventricles. When the ventricles contract, the atrioventricular valves close, and blood is forced into the aorta and pulmonary artery. (The left atrioventricular valve is also known as the mitral or bicuspid valve and the right atrioventricular valve is also known as the tricuspid valve.) Semilunar valves in the aorta and pulmonary artery prevent the blood from flowing back into the ventricles when they relax.
The right and left ventricles are chambers with powerful muscular walls, whose contractions force blood to flow through the arteries to all parts of the body. The valves between the atria and the ventricles, the atrioventricular valves, are important one-way valves that allow blood to flow from the atria to the ventricles but prevent flow in the opposite direction. Similarly, there are valves in both the aorta and pulmonary artery, known as the semilunar valves. The aorta is the large artery that carries blood from the left ventricle to the body, and the pulmonary artery carries blood from the right ventricle to the lungs. The semilunar valves act as “check valves” to prevent blood from flowing back into the ventricles. If the atrioventricular or semilunar valves are damaged or function improperly, the heart’s efficiency as a pump is diminished, and the person may have insufficient blood flow, which can cause shortness of breath, swelling in the feet, or other symptoms.
Malfunctioning heart valves are often diagnosed because they cause abnormal sounds—called heart murmurs—as the blood passes through them. Similarly, if the muscular walls of the ventricles are weakened because of infection, damage from a heart attack, or lack of exercise, the heart’s pumping efficiency is reduced and the person develops symptoms such as shortness of breath, fatigue, or chest pain. Shortness of breath and fatigue result because the heart is not able to pump blood, and the oxygen and nutrients it contains, efficiently to the lungs, muscles, and other parts of the body. Chest pain is caused by an increase in the amount of lactic acid in the heart muscle, because the muscle is not getting sufficient oxygen to satisfy its needs. The heart receives blood from coronary arteries that are branches of the aorta; it is not nourished by the blood that flows through its chambers. If heart muscle does not get sufficient oxygen for a period of time, the portion of the heart muscle not receiving blood dies.
The right and left sides of the heart have slightly different jobs, because they pump blood to different parts of the body. The right side of the heart receives blood from the general body and pumps it through the pulmonary arteries to the lungs, where the exchange of oxygen and carbon dioxide takes place and the blood returns from the lungs to the left atrium. This is called pulmonary circulation. The larger, more powerful left side of the heart receives blood from the lungs, delivers it through the aorta to all other parts of the body, and returns it to the right atrium by way of the veins. This is known as systemic circulation. Both circulatory pathways are shown in figure 24.2. The systemic circulation is responsible for gas, nutrient, and waste exchange in all parts of the body except the lungs.
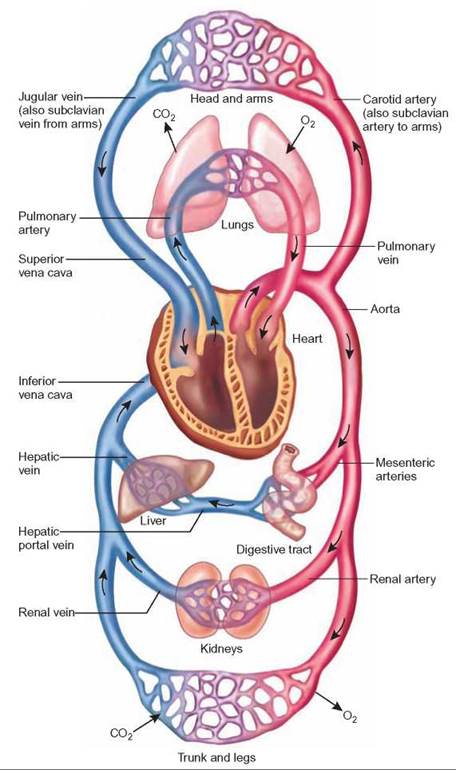
FIGURE 24.2. Pulmonary and Systemic Circulation
The right ventricle pumps blood that is poor in oxygen to the lungs by way of the pulmonary arteries, where it receives oxygen and turns bright red. The blood is then returned to the left atrium by way of four pulmonary veins. This part of the circulatory system is known as pulmonary circulation. The left ventricle pumps oxygen- rich blood by way of the aorta to all parts of the body except the lungs. This blood returns to the right atrium, depleted of its oxygen, by way of the superior vena cava from the head region and the inferior vena cava from the rest of the body. This portion of the circulatory system is known as systemic circulation.
Blood Vessels: Arteries, Veins, and Capillaries
Recall that arteries and veins are the tubes that transport blood from one place to another within the body. Arteries carry blood away from the heart. The contraction of the ventricle walls increases the pressure in the arteries. A typical pressure recorded in a large artery while the heart is in the process of contracting is about 120 millimeters of mercury (mmHg). This is known as the systolic blood pressure. The typical pressure recorded while the heart is relaxing is about 80 millimeters of mercury. This is known as the diastolic blood pressure. A blood pressure reading includes both numbers—for example, 120/80. (Originally, blood pressure was measured by how high the pressure of the blood caused a column of mercury [Hg] to rise in a tube. Although the devices used today have dials or digital readouts and contain no mercury, they are still calibrated in mmHg.)
Artery Structure and Function
The walls of arteries are relatively thick and muscular yet elastic (figure 24.3a). Healthy arteries have the ability to expand as blood is pumped into them and return to normal as the pressure drops. This ability to expand absorbs some of the pressure and reduces the peak pressure within the arteries, thus reducing the likelihood that they will burst. If arteries become hardened and less elastic, peak systolic blood pressure rises and the arteries are more likely to rupture. The elastic nature of the arteries also helps in blood flow. When the arteries return to normal from their stretched condition, they give a little push to the blood flowing through them.

Blood is distributed from the large aorta through smaller and smaller blood vessels to millions of tiny capillaries. Some of the smaller arteries, called arterioles, contract or relax to regulate the flow of blood to specific parts of the body. The major parts of the body that receive differing amounts of blood, depending on need, are the digestive system, muscles, and skin. When you exercise, blood flow to the muscles increases to accommodate their higher metabolic needs—the muscles need to take in more oxygen and glucose and to get rid of wastes. Exercise also results in an increased blood flow to the skin, which allows your body to get rid of excess heat. At the same time, the amount of blood flowing to the digestive system is reduced. Athletes do not eat a full meal before exercising. The additional blood flow to the digestive system reduces the amount of blood available to the muscles and lungs and they are not able to perform as well. In addition, muscular cramps can result if insufficient blood flows to the muscles.
Vein Structure and Function
Veins collect blood from the capillaries and return it to the heart. The pressure in veins is very low. Some of the largest veins may have a blood pressure of 0.0 mmHg for brief periods. The walls of veins are not as muscular as those of arteries (figure 24.3b). Because of the low pressure, veins must have valves to prevent the blood from flowing backwards, away from the heart. Veins are often found on the surface of the body and are seen as blue lines. Varicose veins result when veins contain faulty valves, which do not allow the efficient return of blood to the heart. Therefore, blood pools in these veins, and they become swollen, bluish networks.
Because the pressure in veins is so low, muscular movements of the body are important in helping return blood to the heart. When the muscles of the body contract, they compress nearby veins, and this pressure pushes blood along in the veins. Because the valves allow blood to flow only toward the heart, this activity acts as an additional pump to help return blood to the heart (figure 24.3c). People who sit or stand for long periods without using their leg muscles tend to have a considerable amount of blood pool in the veins of their legs and lower body. Thus, less blood may be available to go to the brain, causing people to faint. Although the arteries are responsible for distributing blood to various parts of the body and arterioles regulate where blood goes, it is the function of capillaries to assist in the exchange of materials between the blood and cells.
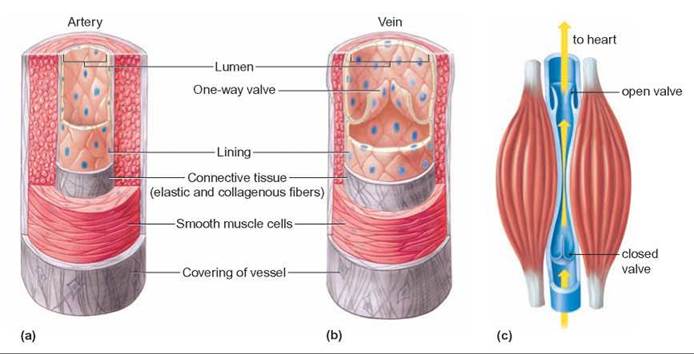
FIGURE 24.3. The Structure of Arteries and Veins
The walls of (a) arteries are much thicker than the walls of (b) veins. (The pressure in arteries is much higher than the pressure in veins.) The pressure generated by the ventricles of the heart forces blood through the arteries. Veins often have very low pressure. The valves in the veins prevent the blood from flowing backward, away from the heart. (c) Contractions of skeletal muscle along with valves in the veins help move blood in the veins back to the heart.
Capillary Structure and Function
Capillaries are tiny, thin-walled tubes that receive blood from arterioles. They are so small that red blood cells must go through them in single file. They are so numerous that each cell in the body has a capillary located near it. It is estimated that there are about 1,000 square meters of capillary surface area in a typical human. Each capillary wall consists of a single layer of cells and, therefore, presents only a thin barrier to the diffusion of materials between the blood and the cells in the surrounding tissue. The flow of blood through these smallest blood vessels is relatively slow. This allows time for the diffusion of such materials as oxygen, glucose, and water from the blood to surrounding cells, and for the movement of waste products such as carbon dioxide, lactic acid, and ammonia from the cells into the blood.
It is also possible for liquid to flow through tiny spaces between the cells of most capillaries. This fluid, tissue fluid, bathes individual cells. This assists in the exchanges of materials between the blood and the cells. Ultimately this fluid must be returned to the circulatory system. Some simply diffuses back into the capillaries. The remainder is collected by lymph vessels and moves through these vessels until it empties into veins near the heart (figure 24.4).
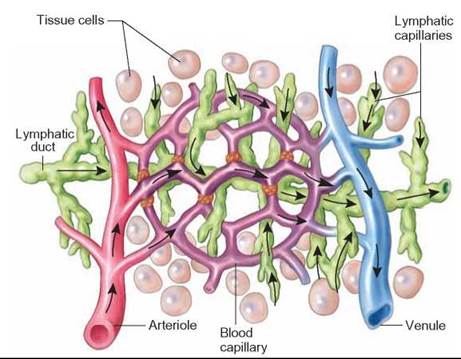
FIGURE 24.4. Capillaries
Capillaries are tiny blood vessels. Exchange of molecules between blood and tissues occurs by diffusion through the thin walls of capillaries. Some water and dissolved materials actually pass through the walls of capillaries and bathe cells. The lymph vessels collect any excess fluid and return it to the circulatory system.
24.2. CONCEPT REVIEW
2. List the functions of the salts and proteins found in the plasma.
3. What are the functions of the heart, arteries, veins, arterioles, blood, and capillaries?
4. How do red blood cells assist in the transportation of oxygen and carbon dioxide?