CONCEPTS IN BIOLOGY
PART VI. PHYSIOLOGICAL PROCESSES
27. Human Reproduction, Sex, and Sexuality
27.9. Fertilization, Pregnancy, and Birth
In most women, an egg (actually a secondary oocyte) is released from the ovary about 14 days before the next menstrual period. The menstrual cycle is usually said to begin on the first day of menstruation. Therefore, if a woman has a regular 28-day cycle, the egg is released approximately on day 14 (review figure 27.15). If a woman normally has a regular 21-day menstrual cycle, ovulation occurs about day 7 in the cycle. If a woman has a regular 40-day cycle, ovulation occurs about day 26. Some women, however, have very irregular menstrual cycles, and it is difficult to determine just when the egg will be released to become available for fertilization. Once the egg is released, it is swept into the oviduct and moved toward the uterus. If sperm are present, they swarm around the egg as it passes down the oviduct, but only one sperm penetrates the outer layer to fertilize it and cause it to complete meiosis. The other sperm contribute enzymes, which digest away the protein and mucous barrier between the egg and the successful sperm.
During the second meiotic division, the second polar body is pinched off and the larger of the two cells, the true ovum, is formed. Because chromosomes from the sperm are already inside, they simply intermingle with those of the ovum, forming a diploid zygote. As the zygote continues to travel down the oviduct, it begins to divide by mitosis into smaller and smaller cells, without an increase in the mass of cells (figure 27.16). This division process is called cleavage.
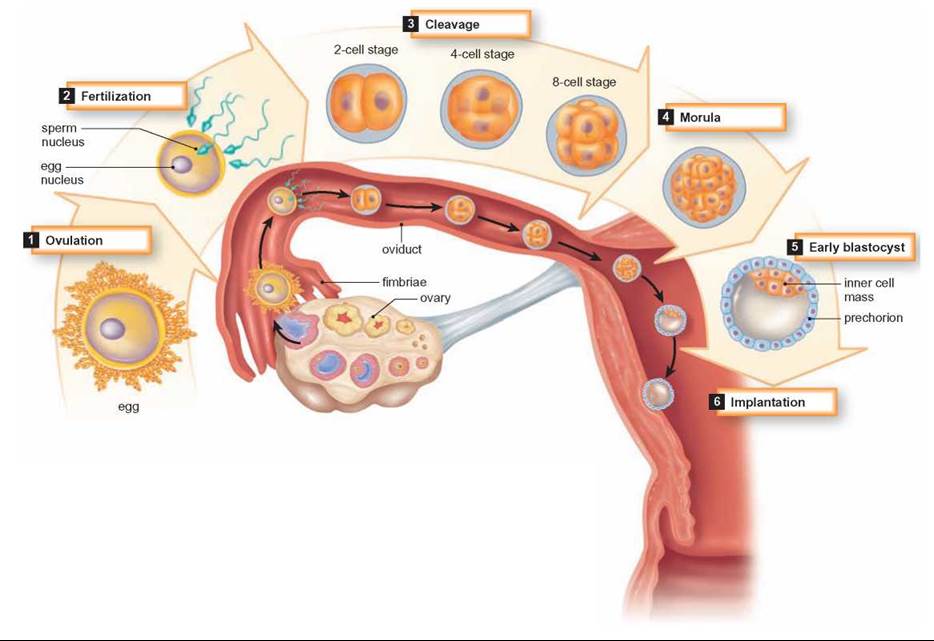
FIGURE 27.16. Human Embryonic Development
Between fertilization and birth, many changes take place in the embryo. Fertilization of the egg takes place in the oviduct and early stages of development take place as the embryo travels to the uterus. By about day 7 following fertilization, the blastocyst has embedded in the lining of the uterus.
Eventually, a solid ball of cells is produced, known as the morula stage of embryological development. The morula continues down the oviduct and continues to divide by mitosis. The result is called a blastocyst. The blastocyst becomes embedded or implanted in the uterine lining when it reaches the uterus (How Science Works 27.2).
The blastocyst stage of the embryo eventually develops a tube, which becomes the gut. The formation of the primitive digestive tract is just one of a series of changes that result in an embryo that is recognizable as a miniature human being.
Most of the time during its development, the embryo is enclosed in a water-filled membrane, the amnion, which protects it from blows and keeps it moist. Two other membranes, the chorion and allantois, fuse with the lining of the uterus to form the placenta (figure 27.17). A fourth sac, the yolk sac, is well developed in reptiles, fish, amphibians, and birds. The yolk sac in these animals contains a large amount of food used by the developing embryo. Although a yolk sac is present in mammals, it is small and does not contain yolk. The embryo’s nutritional needs are met through the placenta. The placenta also produces the hormone chorionic gonadotropin, which stimulates the corpus luteum to continue producing progesterone and thus prevents menstruation and ovulation during pregnancy.
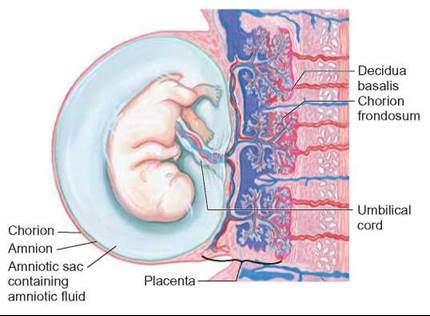
FIGURE 27.17. Placental Structure
The embryonic blood vessels that supply the developing embryo with nutrients and remove the metabolic wastes are separate from the blood vessels of the mother. Because of this separation, the placenta can selectively filter many types of incoming materials and microorganisms.
As the embryo’s cells divide and grow, some of them become differentiated into nerve cells, bone cells, blood cells, or other specialized cells. In order to divide, grow, and differentiate, cells must receive nourishment. This is provided by the mother through the placenta, in which both fetal and maternal blood vessels are abundant, allowing for the exchange of substances between the mother and embryo. The materials diffusing across the placenta include oxygen, carbon dioxide, nutrients, and a variety of waste products. The materials entering the embryo travel through blood vessels in the umbilical cord. The diet and behavior of the mother are extremely important. Any molecules consumed by the mother can affect the embryo. Cocaine; alcohol; heroin; the chemicals in cigarette smoke; and medications, such as Phenytoin (or Dilantin) and Accutane (acne treatment), can all cross the placenta and affect the development of the embryo. Infections by such microbes as rubella virus (German measles), Varicella (chicken pox), and the protozoan Toxoplasma can also result in fetal abnormalities or even death.
The growth of the embryo results in the development of major parts of the body by the tenth week of pregnancy. After this time, the embryo continues to increase in size, and the structure of the body is refined.
HOW SCIENCE WORKS 27.2
History of Pregnancy Testing
The answer to the question "Am I pregnant?" once demanded a combination of guesswork, "old wives' tales" and time. An ancient Egyptian papyrus described a test in which a woman who might be pregnant urinated on wheat and barley seeds over the course of several days: "If the barley grows, it means a male child. If the wheat grows, it means a female child. If both do not grow, she will not bear at all."
In the Middle Ages, so-called "piss prophets" said they could tell if a woman was pregnant by the color of her urine. Urine was described as a "clear, pale lemon color leaning toward off-white, having a cloud on its surface" if she was pregnant. Some mixed wine with urine and watched for changes. In fact, alcohol reacts with certain proteins in urine, so they may have had a little help in guessing.
In 1927, a test was developed that required the injection of a women's urine into an immature female rat or mouse. If the woman was not pregnant, the animal showed no reaction. If she was pregnant, the animal went into heat (displayed behaviors associated with a desire to mate) despite its immaturity. This test implied that, during pregnancy, there was an increased production of certain hormones, and that they were excreted in the urine. In the 1930s, a similar test involved injecting urine into rabbits, frogs, toads, and rats. If pregnancy hormones were in the urine, they induced ovulation in the animals.
However, in 1976, advertisements proclaimed "a private little revolution," the first home pregnancy tests. The FDA granted approval to four tests: Early Pregnancy Test, Predictor, ACU-TEST, and Answer. All the tests identified changes in hormone levels in the urine of pregnant women.
The next generation of home pregnancy tests arrived in 2003, when the FDA approved Clearblue Easy's digital pregnancy test. Instead of showing a thin blue line, the indicator screen now displayed the words "pregnant" or "not pregnant."

Twins
In the United States, women giving birth have a 1 in 40 chance of delivering twins and a 1 in 650 chance of triplets or other multiple births. Twins happen in two ways. In the case of identical twins (approximately one-third of all twins), the embryo splits during cleavage into two separate groups of cells. Each group develops into an independent embryo. Because they come from the same single fertilized ovum, they have the same genes and are the same sex.
Should separation be incomplete, the twins would be born attached to one another, a condition referred to as conjoined twins. Conjoined twins occur once in every 70,000 to 100,000 live births.
Fraternal twins result from the fertilization of two separate eggs by two different sperm. Therefore, they resemble each other no more than do regular brothers and sisters. They do not contain the same genes and are not necessarily the same sex.

Birth
The process of giving birth is also known as parturition, or birthing. At the end of about 9 months, hormonal changes in the mother’s body stimulate contractions of the uterine muscles during a period prior to birth called labor. These contractions are stimulated by the hormone oxytocin, which is released from the posterior pituitary. The contractions normally move the baby headfirst and face down through the vagina, or birth canal. One of the first effects of these contractions may be the bursting of the amnion (“bag of water”) surrounding the baby. Following this, the uterine contractions become stronger, and shortly thereafter the baby is born (figure 27.18). In some cases, the baby becomes turned in the uterus before labor. If this occurs, the feet or buttocks appear first. Such a birth is called a breech birth. This can be a dangerous situation, because the baby’s source of oxygen may be cut off as the placenta begins to separate from the mother’s body before the baby’s head emerges. If for any reason the baby does not begin to breathe on its own, it will not receive enough oxygen to prevent the death of nerve cells; thus, brain damage or death can result.
FIGURE 27.18 Childbirth
What many people refer to as “natural” childbirth is really called a vaginal delivery.
Occasionally, a baby cannot be born vaginally because of its position in the uterus. Other factors include the location of the placenta on the uterine wall and the size of the birth canal. A procedure to resolve this problem is the surgical removal of the baby through the mother’s abdomen. This procedure is known as a cesarean, or C-section. The procedure was apparently named after Roman Emperor Julius Caesar, who was said to have been the first child to be delivered by this method. While C-sections are known to have been performed before Caesar, the name stuck.
Following the birth of the baby, the placenta, also called the afterbirth, is expelled. Once born, the baby begins to function on its own. The umbilical cord collapses and the baby’s lungs, kidneys, and digestive system must now support all bodily needs. Birth is quite a shock, but the baby’s loud protests fill the lungs with air and stimulate breathing.
Over the next few weeks, the mother’s body returns to normal, with one major exception. The breasts, which underwent changes during pregnancy, are ready to produce milk to feed the baby. Following birth, prolactin, a hormone from the pituitary gland, stimulates the production of milk, and oxytocin stimulates its release. If the baby is breast-fed, the stimulus of the baby’s sucking prolongs the time during which milk is produced. This response involves both the nervous and endocrine systems. The sucking stimulates nerves in the nipples and breasts, resulting in the release of prolactin and oxytocin from the pituitary.
Recent studies have found that breast-fed babies are 20% less likely to die between the ages of 1 and 12 months than are those who are not breast-fed. In addition, the longer babies are breast-fed, the lower their risk for early death. The American Academy of Pediatrics has recommended exclusive breastfeeding (that is, only human breast milk—no formula, water, or solids) for the first 6 months of life. Breast-feeding should continue throughout the second half of the baby’s first year with the introduction of solid foods.
In some cultures, breast-feeding continues for 2 to 3 years, and the continued production of milk often delays the reestablishment of the normal cycles of ovulation and menstruation. Many people believe that a woman cannot become pregnant while she is nursing a baby, a method of birth control called Lactation Amenorrhea Method (LAM). For a woman breastfeeding, the probability of becoming pregnant during the first three months is practically zero. However, because there is so much variation among women, relying on this as a natural conception-control method after the first three months is not a good choice. Many women have been surprised to find themselves pregnant again a few months after delivery.
27.9. CONCEPT REVIEW
18. What changes occur in ovulation and menstruation during pregnancy?
19. What are the functions of the placenta?
20. What causes the genetic differences between fraternal twins?