THE LIVING WORLD
Unit Six. Animal Life
27. How the Animal Body Defends Itself
27.11. AIDS: Immune System Collapse
AIDS (acquired immunodeficiency syndrome) was first recognized as a disease in 1981. By the end of 2007 in the United States, 583,298 individuals had died of AIDS, and more than 1 million others were thought to be infected with HIV (human immunodeficiency virus), the virus that causes the disease. Worldwide, 33.4 million are infected, over 25 million have died, and 2 million more die each year. HIV apparently evolved from a very similar virus that infects chimpanzees in Africa when a mutation arose that allowed the virus to recognize a human cell surface receptor called CD4. This receptor is present in the human body on certain immune system cells, notably macrophages and helper T cells. It is the identity of these immune system cells that leads to the devastating nature of the disease.
How HIV Attacks the Immune System
HIV attacks and cripples the immune system by inactivating cells that have CD4 receptors (CD4+ cells), including helper T cells. The significance of killing helper T cells is that it leaves the immune system unable to mount a response to any foreign antigen. AIDS is a deadly disease for just this reason.
HIV’s attack on CD4+ T cells progressively cripples the immune system because HIV-infected cells die after releasing replicated viruses that proceed to infect other CD4+ T cells. Over time, the body’s entire population of CD4+ T cells is destroyed. In a normal individual, CD4+ T cells make up 60% to 80% of circulating T cells; in AIDS patients, CD4+ T cells often become too rare to detect, wiping out the human immune defense. With no defense against infection, any of a variety of otherwise commonplace infections proves fatal. Also, with no ability to recognize and destroy cancer cells when they arise, death due to cancer becomes far more likely. Indeed, AIDS was first recognized because of a cluster of cases of a rare cancer, Kaposi’s sarcoma. More AIDS victims die of cancer than from any other cause.
The fatality rate of AIDS is 100%; no patient exhibiting the symptoms of AIDS has recovered. The disease is not highly contagious because it is only transmitted from one individual to another through the transfer of internal body fluids, typically in semen or vaginal fluid during sexual intercourse and in blood transmitted by needles during drug use. However, symptoms of AIDS do not usually show up for several years after infection with HIV, apparent in the delay of the onset of AIDS in the United States (the red line in figure 27.20) after initial infection with HIV (the green line). Because of this symptomless delay, infected individuals can unknowingly spread the virus to others. Awareness campaigns in the United States have helped reduce the numbers of new AIDS cases.
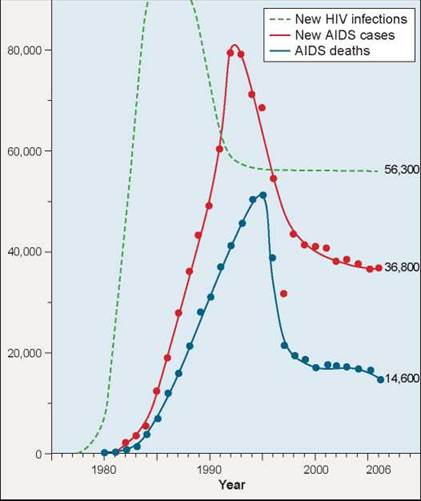
Figure 27.20. The AIDS epidemic in the United States.
The U.S. Centers for Disease Control (CDC) reports that 37,041 new AIDS cases were reported in 2007 in the United States, with a total of over one million cases and nearly 600,000 deaths.
A variety of drugs inhibit HIV in the test tube. These include AZT and its analogs (which inhibit virus nucleic acid replication) and protease inhibitors (which inhibit the production of functional viral proteins). A combination of a protease inhibitor and two AZT analog drugs entirely eliminates the HIV virus from many patients’ bloodstreams. Widespread use of this combination therapy has cut the U.S. AIDS death rate by almost two-thirds since its introduction in the mid-1990s, from 51,414 AIDS deaths in 1995 to 38,074 in 1996, and ten years later in 2006, deaths remained low, at approximately 14,600.
Unfortunately, this sort of combination therapy does not appear to actually succeed in eliminating HIV from the body. While the virus disappears from the bloodstream, traces of it can still be detected in lymph tissue of the patients. When combination therapy is discontinued, virus levels in the bloodstream once again rise. Because of demanding therapy schedules and many side effects, long-term combination therapy does not seem a promising approach.
Scientists continue to seek a vaccine to protect people from this deadly and incurable disease. But over 30 years and 1 million American AIDS cases later, an effective AIDS vaccine so far still eludes the best efforts of researchers. Because the HIV virus generates mutations at such a prodigious rate, few of those infected have exactly the same virus. For this reason, clinical trials of vaccines targeted against one version of HIV have been ineffective against others. The suggestion that portions of the HIV virus do not vary (see page 577) offers encouragement that an effective AIDS vaccine may yet be developed.
Key Learning Outcome 27.11. HIV cripples the vertebrate immune defense by infecting and killing key lymphocytes.
Biology and Staying Healthy
AIDS Drugs Target Different Phases of the HIV Infection Cycle
AIDS is so devastating because it dismantles the very process that the body uses to fight infections. While the search for an AIDS vaccine continues, scientists are also trying to find ways to slow down or halt the process whereby the virus spreads throughout the body, infecting other cells. This doesn't cure the person; he or she still has an HIV infection that can be spread to others. But by slowing down HIV's ability to replicate inside a person, these drugs might help to curb the effects of HIV that lead to the development of AIDS.
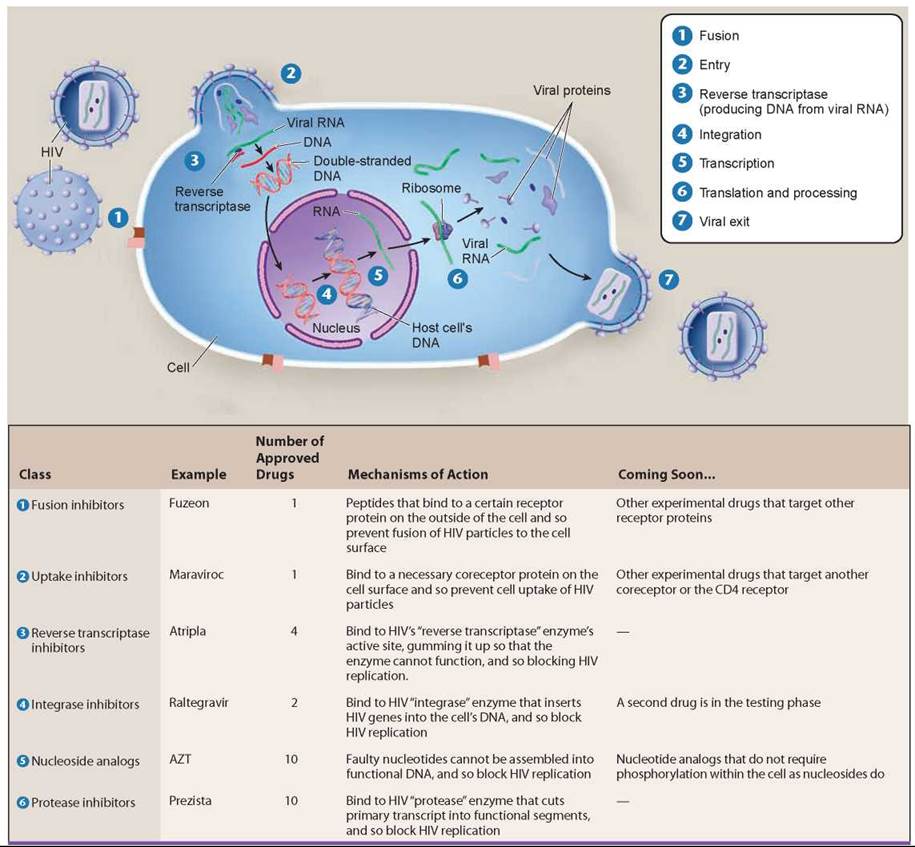
Many new drugs are being developed that target different phases of the viral infection cycle. To date there are six classes of drugs (described below and keyed to the diagram) that disrupt the ability of HIV to enter the cell, to replicate its DNA, and to form new viral particles. As of yet, there has been little drug development targeting the final phase of the infection cycle, viral exit (7 where new viruses leave the cell).
Inquiry & Analysis
The immune response provides a valuable protection against infection because it can remember prior experiences. We develop lifelong immunity to many infectious diseases after one childhood exposure. This long-term immunity is why vaccines work. A key question about immune protection is whether or not it is specific. Does exposure to one pathogen confer immunity to only that one, or is the immunity you acquire a more general response, protecting you from a range of infections?
The graph to the right displays the results of an experiment designed to answer this question. A colony of rabbits is immunized once with antigen A, and the level of antibody directed against this antigen monitored in each individual. After 40 days, each rabbit is reinjected, some with antigen A and others with antigen B, and the level of antibody directed against the reinjected antigens is monitored. The red line is typical of results for antigen A, the blue line for antigen B.
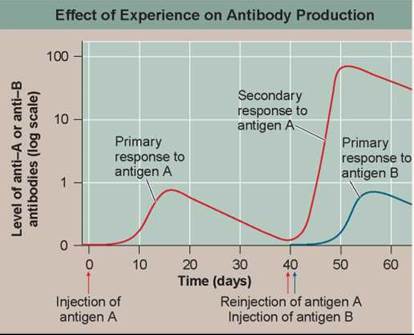
1. Applying Concepts
a. Variable. In the graph, what is the dependent variable?
b. Reading a Continuous Curve. Does each injection of antigen A result in detectable antibody production? antigen B?
2. Interpreting Data
a. The initial response to antigen A is called the "primary" response, and the second response to antigen A administered 40 days later is called the "secondary" response. Compare the speed of the primary and secondary responses—which reaches maximal antibody response quicker?
b. Compare the magnitude of the primary and secondary immune responses to antigen A—are they similar, or is one response of greater magnitude?
3. Making Inferences
a. Why is the secondary response induced by a second exposure to antigen A different from the primary response?
b. Is the response to antigen B more similar to the primary or secondary response of antigen A?
4. Drawing Conclusions
a. Does the prior exposure to antigen A have any impact on the speed or magnitude of the primary response to antigen B?
b. Is the immune response to these antigens antigen-specific?
5. Further Analysis. If you were to inject both sets of rabbits with antigen B on day 80, what would you expect the results to be? Explain the difference you would expect in the immune responses of the two groups of rabbits to this injection, if any.
1. Skin is a physical barrier but also provides chemical protection generated with
a. sweat and oil glands.
b. mucus.
c. the skin’s basal layer.
d. the stratum corneum of the skin.
2. The immune system can identify foreign cells in the bloodstream because these foreign cells
a. are observed destroying other cells by the immune system.
b. have cell surface proteins that are different from the body’s own cell surface proteins.
c. have CD4 receptors similar to T cells.
d. All of the above.
3. The purpose of the inflammatory response is to
a. increase the temperature of an infected area.
b. reduce pain of an infected area.
c. increase the number of immune system cells in an infected area.
d. form a barrier around the infected area.
4. Increasing human body temperature—that is, causing a fever— assists the immune system because
a. increased temperature speeds up the chemical reactions used by the immune system.
b. pathogenic bacteria do not grow well at high temperatures.
c. increased temperature causes body cell proteins to denature.
d. All of the above.
5. Immune responses tailored to specific antigens involve
a. T cells.
b. macrophages.
c. monocytes.
d. neutrophils.
6. Antibody production takes place in
a. T cells.
b. natural killer cells.
c. B cells.
d. mast cells.
7. Cytotoxic T cells
a. produce antibodies.
b. destroy pathogens directly.
c. destroy foreign antigens floating freely in the bloodstream.
d. destroy cells infected by pathogens.
8. Immunity to future invasion of a specific pathogen is accomplished by production of
a. plasma cells.
b. memory T and B cells.
c. helper T cells.
d. monocytes.
9. When a body’s immune system attacks the body’s own cells, this is called
a. an inflammatory response.
b. a temperature response.
c. an autoimmune response.
d. an allergic response.
10. HIV-infected people with advanced AIDS usually die of an infectious disease or cancer. This is because HIV attacks
a. helper T cells.
b. neutrophils.
c. memory T and B cells.
d. mast cells.