MCAT Biology Review
Chapter 8: The Immune System
Introduction
Over the past few decades, the public’s imagination has been captured by alarming reports of “flesh-eating” bacteria and diseases. In fact, these bacteria do not actually eat flesh, but that doesn’t make them any less dangerous. “Flesh-eating” bacteria cause a condition called necrotizing fasciitis, a serious disease that requires aggressive medical and surgical treatment, including intravenous antibiotics, surgical debridement (removal) of the necrotic tissue, and sometimes even amputation. Many different types of bacteria, including group A Streptococcus, Clostridium perfringens, and methicillin-resistant Staphylococcus aureus (MRSA), can cause necrotizing fasciitis. The pathological and life-threatening impact of this disease is a massive destruction of skin, muscle, and connective tissue by the release of bacterial toxins called superantigens. These proteins cause the immune system to become nonspecifically overactivated. Necrotizing fasciitis is dangerous not only because of the bacteria and subsequent inflammatory response, but also because the destruction of skin—a nonspecific immune defense—leaves the body susceptible to superinfection (infection with another pathogen).
In this chapter, we will consider this type of nonspecific defense as well as specific immune defenses. The human body relies on the interaction between the innate (nonspecific) and adaptive (specific) immune systems in order to protective itself from disease. However, the immune system is not always perfect in its responses. Sometimes the immune system may become overactivated, as is the case with necrotizing fasciitis, or it may become activated against the same human it is supposed to protect. In this chapter, we will discuss the individual parts of the immune system and how these parts work together to protect from disease. In addition, we will discuss the concept of autoimmunity, or disease that results from immune attack against self. We’ll briefly touch on vaccines, which take advantage of our understanding of the immune system to protect us from life-threatening infections. The immune system is largely integrated with the lymphatic system, which will be discussed in this chapter as well.
8.1 Structure of the Immune System
Each day, the human body is exposed to numerous bacteria, viruses, fungi, and even parasites. Yet our bodies are able to protect us from infection most of the time. Even when we do get sick, the immune system is usually able to contain and eliminate the infection.
INNATE AND ADAPTIVE IMMUNITY
In order to fight infection, the human body has two different divisions of the immune system: innate and adaptive immunity, compared in Figure 8.1. Innate immunity is composed of defenses that are always active against infection, but lack the ability to target specific invaders over others; for this reason, it is also called nonspecific immunity. Adaptive or specific immunity refers to the defenses that target a specific pathogen. This system is slower to act, but can maintain immunological memory of an infection to be able to mount a faster attack in subsequent infections.
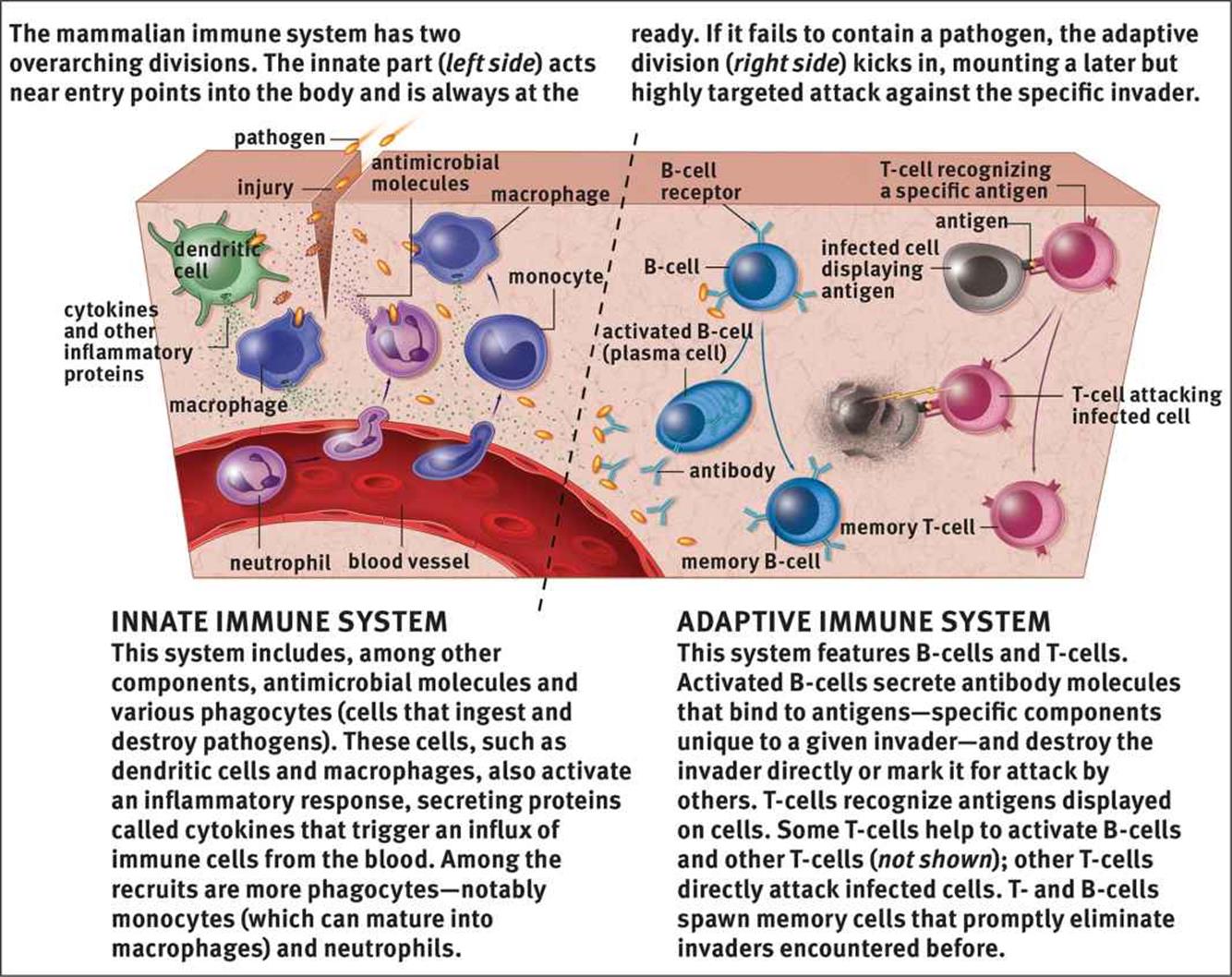 Figure 8.1. Divisions of the Immune System
Figure 8.1. Divisions of the Immune System
MCAT EXPERTISE
The immune system is a topic where cell biology, biochemistry, anatomy, and biology interact. Thus, it is a topic that allows the MCAT to ask questions that integrate these four topics. As we discuss these complex ideas, focus on the big picture first, creating a mental image to help you to put these concepts together. Then go back and plug in the details. This approach will foster your ability to associate structure with function and to think critically about the topic on Test Day.
ANATOMY
The immune system is not housed in a single organ, as shown in Figure 8.2. The structure and components that serve as nonspecific defenses often serve functions in other organ systems. The bone marrow produces all of the leukocytes (white blood cells) that participate in the immune system through the process of hematopoiesis, discussed in Chapter 7 of MCAT Biology Review. The spleen is a location of blood storage and activation of B-cells, which turn into plasma cells to produce antibodies as part of adaptive immunity. Note that when B-cells leave the bone marrow, they are considered mature but naïve (because they have not yet been exposed to an antigen). Because these antibodies dissolve and act in the blood (rather than within cells), this division of adaptive immunity is called humoral immunity. T-cells, another class of adaptive immune cells, mature in the thymus, a small gland just in front of the pericardium, the sac that protects the heart. T-cells are the agents of cell-mediated immunity because they coordinate the immune system and directly kill virally infected cells. Finally, lymph nodes, a major component of the lymphatic system, provide a place for immune cells to communicate and mount an attack; B-cells can be activated here as well. Other immune tissue is found in close proximity to the digestive system, which is a site of potential invasion by pathogens. These tissues are commonly called gut-associated lymphoid tissue (GALT) and include the tonsils and adenoids in the head, Peyer’s patches in the small intestine, and lymphoid aggregates in the appendix.
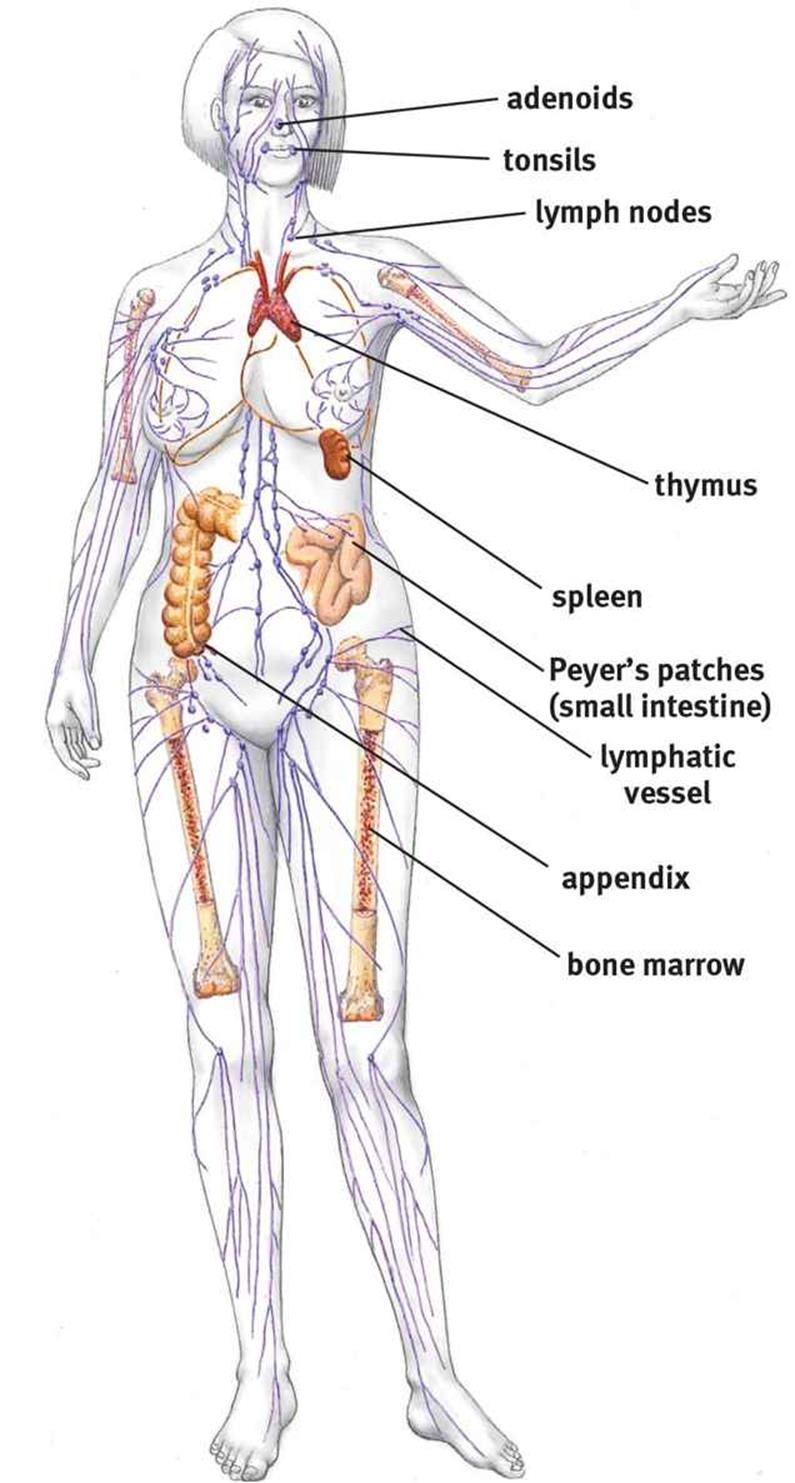 Figure 8.2. Anatomy of the Immune and Lymphatic Systems
Figure 8.2. Anatomy of the Immune and Lymphatic Systems
REAL WORLD
Lay people not involved in medicine often say that their “glands” are swollen when they feel a sensation of fullness around the throat. From a biological standpoint, lymph nodes are not glands—they do not secrete products into the bloodstream (endocrine) or ducts (exocrine). What they are actually experiencing is known medically as lymphadenopathy, or the swelling of the lymph nodes that occurs with activation of the immune system.
KEY CONCEPT
Organs of the immune system:
· Lymph nodes filter lymph and are a site where immune responses can be mounted.
· Bone marrow is the site of immune cell production.
· The thymus is the site of T-cell maturation.
· The spleen is a storage area for blood, filters blood and lymph, and is a site where immune responses can be mounted.
Leukocytes are produced in the bone marrow through hematopoiesis, shown in Figure 8.3. (Note: This is the same image shown in Figure 7.7, but is copied here for convenience.) Leukocytes are divided into two groups of cells: granulocytes and agranulocytes. This name refers to the presence or absence of granules in the cytoplasm. These granules contain toxic enzymes and chemicals, which can be released by exocytosis, and are particularly effective against bacterial, fungal, and parasitic pathogens. Both granulocytes and agranulocytes come from a common precursor: hematopoietic stem cells. Remember from Chapter 7 that hematopoietic stem cells are also the cell type that gives rise to red blood cells and platelets. Granulocytes include cells such as neutrophils, eosinophils, and basophils. The names of these cells actually refer to the way that the cells appear after staining with certain chemicals. Agranulocytes include the lymphocytes, which are responsible for antibody production, immune system modulation, and targeted killing of infected cells. Monocytes, which are phagocytic cells in the bloodstream, are also considered agranulocytes. They become macrophages in tissues; many tissues have resident populations of macrophages with specific names (such as microglia in the central nervous system, Langerhans cells in the skin, and osteoclasts in bone).
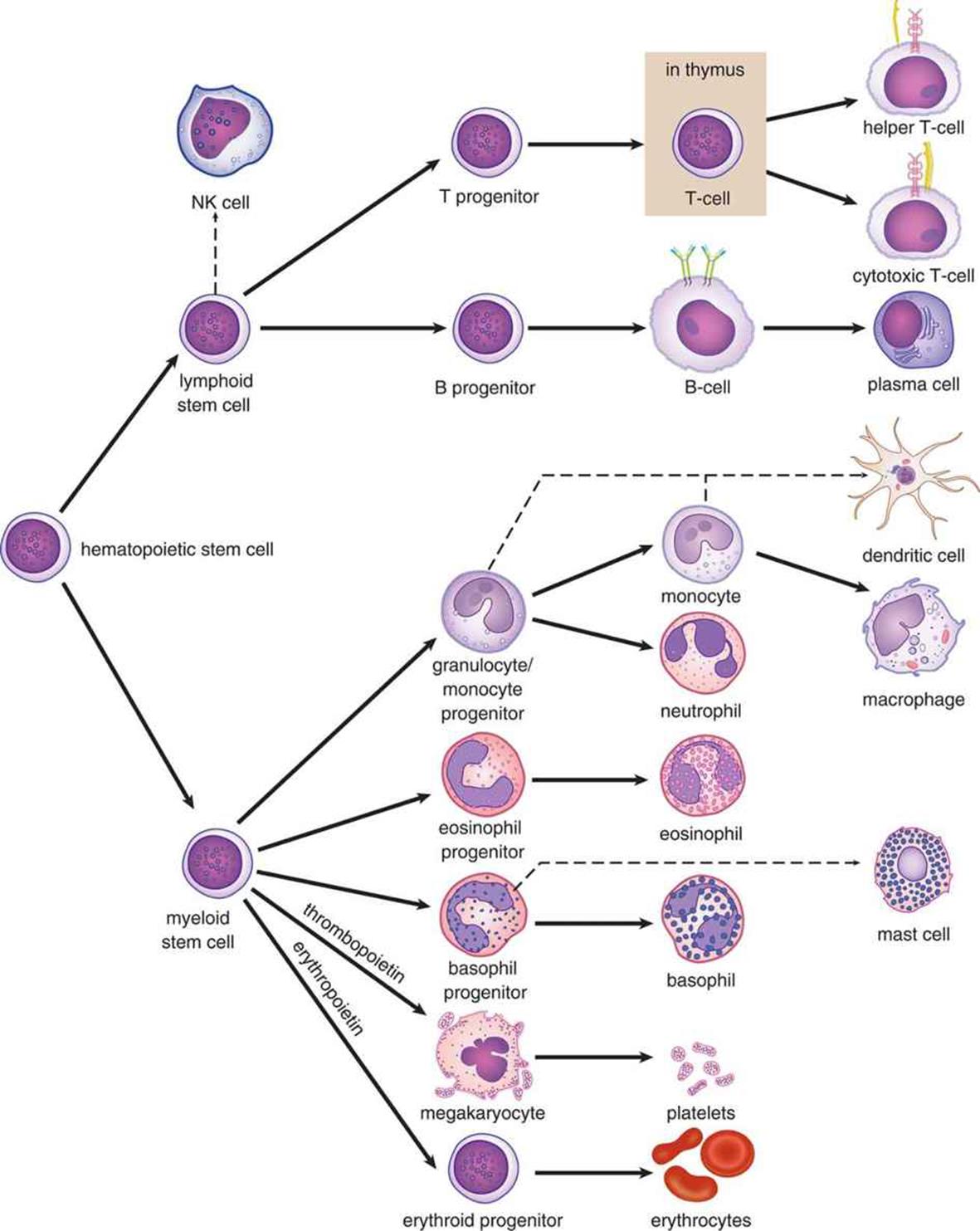 Figure 8.3. Hematopoiesis
Figure 8.3. Hematopoiesis
REAL WORLD
One of the tests often ordered by physicians is known as a complete blood count (CBC). This test counts the number of red blood cells, platelets, and white blood cells. If the CBC is ordered with a differential, it means that each type of white blood cell is counted. Any cell populations that are abnormal may indicate a particular type of infection given the right clinical conditions. For example, if 90 percent of the white blood cells are neutrophils, it is possible that a bacterial infection is present. If 20 percent of the white blood cells are eosinophils, it is possible that an invasive parasitic infection is present.
Innate immunity refers to the responses cells can carry out without learning; for this reason, it is also known as the nonspecific immune response. Conversely, adaptive immunity is developed as immune cells learn to recognize and respond to particular antigens and is often aptly referred to as the specific immune response. We can also divide the specific immune system into humoral immunity (driven by B-cells and antibodies) and cell-mediated immunity (provided by T-cells).
MCAT Concept Check 8.1:
Before you move on, assess your understanding of the material with these questions.
1. What are the differences between innate and adaptive immunity?
· Innate immunity:
· Adaptive immunity:
2. Compare and contrast B- and T-cells:
|
Cell Type |
Site of Development |
Site of Maturation |
Major Functions |
Specific or Nonspecific? |
Humoral or Cell-Mediated? |
|
B-cell |
|||||
|
T-cell |
3. Which cells are considered granulocytes? Which are considered agranulocytes?
· Granulocytes:
· Agranulocytes: