The Biology Book: From the Origin of Life to Epigenetics, 250 Milestones in the History of Biology (2015)
Bacterial Resistance to Antibiotics
1967
When penicillin was first introduced in the 1940s, it ushered in a new era in the treatment of infectious diseases that were previously untreatable and often fatal. Penicillin was the first antibiotic, a substance derived from bacteria or fungi that kills or controls the growth of other microbes. More antibiotics were developed that were chemical modifications of natural antibiotics and drugs made in the laboratory.
DASHED HOPES. Early on, many experts believed that antibiotics would eradicate infectious diseases that had long plagued humans and animals, relegating such diseases to medical history books. Unfortunately, that initial enthusiasm was tempered when many infectious microbes were found resistant to these drugs. For example, in 1967, the first penicillin-resistant strain of the staphylococcus that caused pneumonia appeared in Australia. More frightening is a recent report that 70 percent of bacteria causing hospital-acquired infections are now resistant to at least one of the antibiotics used to treat them.
Bacterial resistance results from two general mechanisms: mutations and horizontal gene transfer. Normally, an antibiotic binds to a critical microbial protein, preventing the protein from functioning normally. If that function involves the synthesis of DNA that codes for the manufacture of an essential protein or the bacterial cell wall, the bacteria will be killed. If, however, bacteria have a mutation in their DNA that interferes with the antibiotic’s attachment to that protein, the bacteria will survive. Based on the process of natural selection, the surviving mutant bacteria will better compete for resources and survive. Resistance can also result from horizontal gene transfer (swap DNA), where one microbe receives a resistant (R) gene or DNA from another antibiotic-resistant microbe. This mechanism does not involve evolution, since no new DNA is being formed.
Resistant bacteria can chemically inactivate the antibiotic, prevent it from attaching to the bacteria, or prevent it from gaining access or building up inside the bacterial cell. Many consequences of bacterial resistance may occur: higher and more dangerous doses of the antibiotic must be used; more expensive drugs may be required; or the patient may fail to recover.
SEE ALSO: Prokaryotes (c. 3.9 Billion BCE), Fungi (c. 1.4 Billion BCE), Darwin’s Theory of Natural Selection (1859), Genes on Chromosomes (1910), Antibiotics (1928), Bacterial Genetics (1946), Plasmids (1952), Human Microbiome Project (2012).
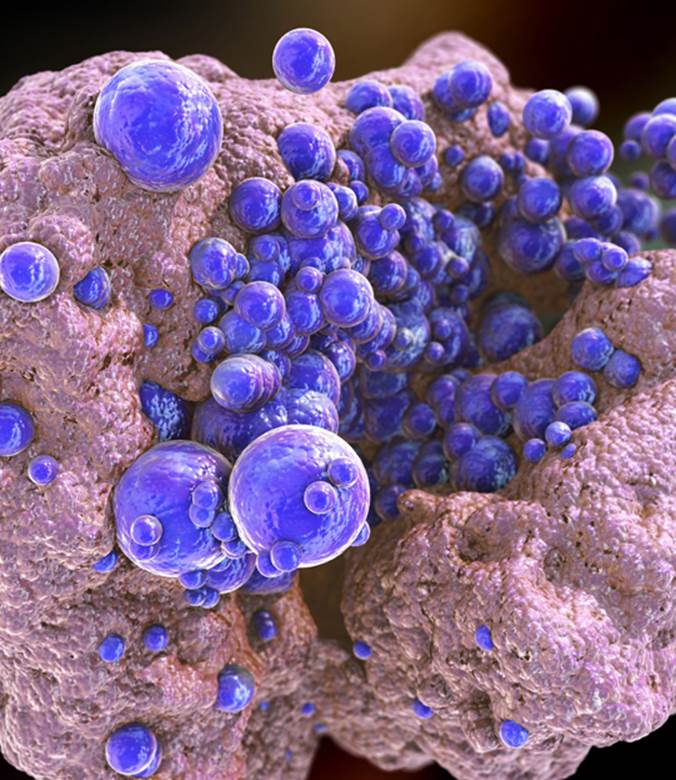
Several years after the introduction of the antibiotic methicillin in 1959, reports surfaced of methicillin-resistant Staphlococcus aureus (MRSA, shown). The development of resistance has been attributed to horizontal gene transfer via plasmids.