CHEMICAL BIOLOGY
Metals in Medicine, Imaging Agents
Peter Caravan, A. A. Martinos Center for Biomedical Imaging, Department of Radiology, Massachusetts General Hospital, Harvard Medical School, Charlestown, Massachusetts
doi: 10.1002/9780470048672.wecb332
The use of metal ions in diagnostic medicine is widespread. Metal complexes and nanoparticles are used clinically in magnetic resonance imaging, nuclear medicine (gamma scintigraphy and positron emission tomography), and X-ray imaging. Preclinically, additional advances are being made in these fields through the creative application of metal complexes and metal-containing nanoparticles. This article briefly describes different clinical imaging modalities and the physico-chemical properties required for imaging agents. Commercial agents are used to illustrate these properties and to describe the clinical state of the art. Selected examples of exciting preclinical imaging agents that have shown efficacy in vivo also are described.
Imaging agents are defined here as compounds that either are required to generate an in vivo image or provide additional contrast to an existing in vivo image. This article describes the use of metal-containing compounds for clinical or preclinical in vivo imaging. This topic covers modalities such as magnetic resonance imaging (MRI), nuclear imaging [gamma scintigraphy, single photon emission computed tomography (SPECT), and positron emission tomography (PET)], X-ray imaging, and computed tomography (CT). Ultrasound contrast agents are used clinically, but these agents do not require a metal ion. For space constraints, cell tracking studies by MRI, reporter gene imaging with PET, and in vitro imaging will not be discussed. The focus will be on compounds used in clinical medicine and those with potential for clinical use. References are limited to 40, so where possible, relevant reviews have been cited. This article aims to provide a sense for the properties (chemical, magnetic, nuclear, etc.) required for an imaging agent, the current clinical practice, and the current promising directions in preclinical research.
Overview of Imaging Agents and Imaging Modalities
General requirements
Imaging agents are used for noninvasive in vivo diagnosis. They generally have found usage where the diagnostic information yielded impacts a life-threatening and/or expensive clinical decision or where the imaging test replaces a more invasive, risky procedure. An example of this use is imaging myocardial perfusion to test for the presence of coronary artery disease. Absence of disease sees the patient sent home, whereas presence of disease results in cardiac catheterization and possible percutaneous or bypass intervention.
For approval, the agent must demonstrate efficacy compared with an accepted gold standard (biopsy, other established imaging modality, or patient outcome). Because imaging agents themselves offer no therapeutic benefit, the safety requirement is quite high. Potential side effects must be minimized, and for nonendogenous metals, such as gadolinium, it is critical that the entire dose be eliminated from the body. The effective concentration range of the agent depends on the technique. For X-ray agents, millimolar tissue concentrations are required to generate contrast. For such highly concentrated agents, it is important to minimize the osmolality of the injected solution to prevent osmotic shock. Nuclear agents are effective at nanomolar or lower concentrations, and toxicity is usually less of an issue; however, receptor-targeted agents should not show any agonist activity.
Metal-essential versus metal-tagged imaging agents
For the compounds described here, the metal is essential for providing image contrast or for creating the image. However, the biologic distribution of the agent can depend primarily on the metal (metal essential) or the distribution can be dependent on a conjugated targeting vector, such as an antibody (metal-tagged) (Fig. ??). In all modalities, metal-essential imaging agents exist. These compounds often have nonspecific targeting and are used to image the blood vessels or organs in an elimination pathway (e.g., the liver or the kidney). However, other agents exhibit more specific targeting and require the metal for this targeting.
Metal-tagged agents exploit the imaging properties of the metal, but they are guided by a small molecule, peptide, or protein-targeting vector. It has become recognized that the metal complex and linker group (Fig. ??) also can impact targeting, especially with smaller targeting vectors. The complex and the linker can represent points to alter lipophilicity, charge, and nonspecific protein binding.
Comparison of imaging modalities
Clinical imaging modalities have different strengths and weaknesses. CT relies on X-ray radiation as a source. Multislice CT scanning is very fast and provides excellent spatial resolution (submillimeter) in a clinical setting. However, the radiation dose to the patient is high, soft tissue contrast is poor, and exogenous contrast agents are required at very high concentrations (millimolar) to create CT contrast. MRI does not require ionizing radiation, has excellent spatial resolution (routinely 1 mm3 clinically), and has good soft tissue contrast; however, scan times are longer than for CT and may be prone to motion artifacts. MRI contrast agents currently require concentrations in the micromolar regime to generate robust contrast. PET and SPECT both require radioactive isotopes to generate the image. Very low chemical concentrations (nanomolar) can be detected, which enables the imaging of low-concentration targets, like neurotransmitters, with these techniques. PET imaging can provide quantitative data on receptor occupancy. However, spatial resolution is much worse with these nuclear techniques (>5 mm clinically) than with CT or MRI and the images are susceptible to attenuation and motion artifacts. Nuclear agents typically must be prepared on the day of use because of their short half-lives. These agents also bring a radiation dose to the patient.
Clinical hybrid PET-CT and PET-MRI systems are being developed now. These approaches combine the high-resolution anatomical imaging of CT or MRI with the sensitive molecular targeting of PET.
X-ray or CT Contrast Agents
Planar X-ray imaging is the oldest and most common radiographic technique. CT (formerly, computed axially tomography—CAT scan) is a method in which a series of two-dimensional X-ray images are acquired around an axis of rotation and these images are combined mathematically to generate a three-dimensional image. Contrast in X-ray imaging derives from heavier atoms (Ca, P) and denser tissue (bone) absorbing and scattering the X rays. Compounds administered to provide additional contrast are termed contrast agents, contrast media, or X-ray dyes. These compounds contain atoms with a large atomic number, Z, such as iodine (Z = 53).
The most common X-ray agents are based on highly soluble tri-iodo aryl derivatives. However, some metal-containing X-ray contrast media exist. The most common is barium sulfate, administered as a suspension to provide contrast in imaging the gastrointestinal tract. Barium (Z = 56) is quite opaque to X rays, and the sulfate salt is very insoluble, which results in negligible oral bioavailability. The insolubility of BaSO4 obviates its use for intravenous applications, and soluble Ba(II) complexes are quite labile, releasing the toxic free metal ion.
Gadolinium MRI contrast agents have been used clinically for X-ray contrast (1). These agents have been used mainly with patients known to have an allergy to iodinated contrast. The use of Gd(III) complexes has derived from the excellent safety profile of these agents, the ability to formulate them at the molar concentrations required for injection, the high atomic number of Gd, and the fact that they are available clinically. These compounds are given intravenously or intra-arterially for angiographic imaging.
Animal studies have been reported with other Gd(III) compounds and also where the Gd(III) was replaced by other lanthanides, such as Yb(III) or Dy(III). The liver-specific agent [Gd(EOB-DTPA)]2-and its Yb(III) and Dy(III) analogs were evaluated in rat, rabbit, and dog models and could provide good contrast to distinguish liver tumors (2). Recently, bismuth sulphide nanoparticles coated with the biocompatible polymer polyvinylpyrrolidone were described (3). Analogous to the iron oxide particles (see below), these nanoparticles were shown to provide contrast in the blood pool and in lymph nodes. Coated gold nanoparticles also have been studied in an animal model (4). Earlier efforts involved metal clusters such as polyoxotungstates; Yu and Watson give an excellent review of metal-based X-ray contrast media up to 1999 (5).
MRI Contrast Agents
Clinical MRI typically involves imaging the hydrogen atoms in water and fat. These molecules are the most abundant molecules in the body, and hydrogen has the highest NMR sensitivity of elements found in the body. A strong magnetic field is required for detection (clinical fields range from 0.3 to 7.0 tesla, most common is 1.5 T ~ 64 MHz). Applied magnetic field gradients provide spatial encoding that allows an image to be reconstructed.
In CT, contrast occurs solely because of the attenuation of the X-ray beam by its interaction with tissue. Contrast in MRI depends on how the image is acquired. Proton density images reflect the different amounts of water content in different tissues. Chemical shift imaging can distinguish water from fat, based on the different chemical shifts of these protons. Contrast also can be altered in other ways: by the exploitation of differences in water diffusion in tissue, by chemical exchange, and by magnetization transfer effects, to name a few. The majority of scans used clinically derive contrast from differences in the relaxation times T1, T2, and T2*.
When nuclei are excited by a radiofrequency (rf) pulse, T1 is the time constant for the realignment of spins with the static magnetic field (along the z-axis, the longitudinal relaxation). T1 ranges from about 300 ms for fat to several seconds for cerebrospinal fluid. If the delay between repeated acquisitions is not long enough, then magnetization will not have recovered fully. For a given delay time (repetition time, TR), tissue with a short T1 will recover more magnetization and generate more signal than tissue with a long T1. This occurrence will give rise to a T1-weighted contrast where areas of short T1 appear bright.
After excitation, spins do not behave uniformly in the xy plane but begin to dephase because of magnetic interactions with neighboring nuclei. This relaxation is denoted T2. In addition, a relaxation time called T2* incorporates T2 but also depends on spatial variation in the local magnetic field. T2 and T2* values in tissue are much shorter (<100ms) than T1. In a spin-echo sequence, an initial 90° pulse is followed by a delay, TE. Then, the dephasing nuclei are refocused because of a 180° pulse and the signal of this spin echo is acquired. Tissue with T2 long compared with TE will produce more signal than tissue with T2 < TE, which gives rise to T2-weighted contrast.
By changing the pulse sequence or the imaging variables TE and TR, different degrees of soft tissue contrast can be obtained. MRI contrast agents provide increased contrast by acting on T1, T2, and T2*.
Paramagnetic agents—gadolinium and manganese
The most widely used clinical MRI contrast agents are based on Gd(III). Approved agents are shown in Fig. ??. These neutral or anionic complexes (as the meglumine or sodium salt) are highly soluble and formulated at 0.25-1 M. They consist of a Gd(III) ion sequestered by an octadentate ligand with a water coligand. Gd(III) has seven unpaired electrons and a symmetric 8S ground state (Mn(II), S = 5/2, 6S state). The high spin number and relatively slow electronic relaxation make these complexes potent nuclear relaxation agents. The octadentate ligand is required for high thermodynamic stability to prevent the potentially toxic Gd(III) ion from being released in vivo. The ligand also directs the biodistribution of the complex (metal-essential). The coordinated water is critical for transmitting the relaxation effect. The water ligand is in fast exchange (105-107 s-1 at 37° C) with bulk water. Relaxation of this water coupled with fast exchange results in an overall shortening of the bulk water relaxation time, which affects image contrast.
MRI agents are characterized in terms of relaxivity. Relax- ivity is defined as the extent to which the contrast agent can change the relaxation rate of solvent water protons normalized to the concentration of the metal ion M (Equation 1)
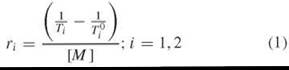
where Ti0 is the relaxation time in the absence of contrast agent. Increased relaxivity enables detection at lower concentrations of agent. Gadolinium and manganese complexes shorten both T1 and T2. However, because tissue T1 is usually much longer than T2, these contrast agents affect T1 on a much greater percentage basis and often are referred to as T1-agents. T1-agents provide positive (bright signal) contrast.
Some relaxivities of Gd, Mn, and Fe agents are listed in Table ??. For discrete chelates, differences in relaxivity occur mainly because of differences in innersphere hydration number (q), in molecular tumbling, and in the rate of water exchange from the inner coordination sphere. Small paramagnetic molecules tumble in solution at GHz frequencies generating a fluctuating magnetic field that can induce nuclear relaxation. However, for imaging studies done at 65 MHz, relaxation is not as efficient as it could be. Compare the relaxivities of GdDTPA and MS-325. MS-325 targets serum albumin and has a much higher relaxivity than GdDTPA in plasma at 0.47 T or 1.5 T (20 or 64 MHz) because when MS-325 is protein -bound, it tumbles much more slowly and relaxation is more efficient. GdDTPA does not bind to proteins and has a lower relaxivity. At higher fields, the frequency match of tumbling with Larmor frequency decreases for protein-bound MS-325 and relaxivity drops as well. Strategies for slowing molecular tumbling through protein binding, through increased molecular size, or through increased rigidity have proved useful for increasing relaxivity (6).
For fast-tumbling complexes, it is fast motion and not slow water exchange that limits relaxivity. In Table ??, relaxivities for the first four compounds are very similar because they have similar size and molecular weight and tumble in solution at about the same rate, even though they have water exchange rates differing by a factor of 10 (GdDTPA vs. GdDTPA-BMA). When tumbling is slowed, water exchange can be limiting. The water exchange rate also can be adjusted by changing the donor atoms or chelate geometry (7). Amide oxygen donors generally decrease water exchange relative to the carboxylate analog, whereas phosphonate donors will increase it. Slow water exchange can limit relaxivity, but it only becomes pronounced when molecular tumbling is slowed.
The hydration number, q, also can be increased, but it may make the complex less stable to transmetallation in vivo. Another commonly observed drawback of opening up additional sites for water coordination is competition with endogenous ligands (for example, citrate) for metal binding. However, Raymond and coworkers (8, 9) have described a series of q = 2 or 3 complexes with fast water exchange that are resistant to transmetallation and/or anion binding. Increasing q also should be coupled with slowed tumbling to achieve very high relaxivity. Aime et al. (10) recently have demonstrated this with a novel q = 2 complex bound to albumin.
Another approach is to assemble multiple chelates either covalently (11) (oligomer, polymer, and dendrimer) or noncovalently (12, 13) (micelle, liposome, and emulsion). These approaches all yield higher molecular relaxivities because of the assembly, but the per-ion relaxivity also is increased because motion is slowed. Fast internal motions can limit these relaxiv- ity gains, but this limitation can be overcome by rigidifying the structure in some way (14).
Iron oxide particles
A different class of MRI contrast agents are the iron oxide particles (15). These particles mainly are referred to as ultrasmall particles of iron oxide (USPIO), small particles of iron oxide (SPIO), or large particles. Sometimes the term microcrystalline iron oxide nanoparticle (MION) is used. USPIO and SPIO are superparamagnetic, which means that they become magnetic in the presence of an applied field but revert to being nonmagnetic when taken out of the field. USPIO have a single Fe3O4 core about 4-5 nm in diameter, and it is coated to make the particle biocompatible. SPIO have more than one crystal of iron oxide and are larger than USPIO but still submicron. The small size allows SPIO and USPIO to be formulated as suspensions and administered intravenously. Large particles have been used for GI tract imaging after oral administration.
No innersphere water molecules in iron particles exist, and the relaxation of water derives from the water molecules diffusing near the particle. Some generalities exist about relaxivity in these particles. For the USPIO, longitudinal relaxivity (r1) can be quite high, and these can function as effective T1 agents, especially at lower fields. The r2/r1 ratio for USPIO is significantly larger than for gadolinium complexes, and r2/r1 increases with increasing magnetic field. When an aggregation of crystals exists, which is the case in SPIO, r1 decreases while r2 increases. Thus, both for the particles themselves as well as for aggregates of particles, the ratio of r2/r1 typically increases as the size of the particles or aggregates increases, although the T2-relaxivity as a function of particle size can be quite complicated.
These agents are used mainly as T2-agents where they provide negative image contrast (destroy signal) wherever they localize. The mechanism is predominantly through altering the local magnetic susceptibility, T2*. Gadolinium agents need to interact directly with water to cause relaxation. The T2* effect of iron oxides is a through space effect and means that even if the agent is compartmentalized in a small space, it still can provide significant contrast. A good example of this effect is in brain perfusion imaging. Even though the blood vessels represent only about 3% of the brain, the T2* effect of the contrast agent extends well beyond the vessels and yields robust contrast.
Iron particles have been coated with different biocompatible reagents, such as dextran and citrate. The coating and particle size both impact biodistribution. Recent efforts (16, 17) have focused on using chemically functionalizable coatings.
Clinical applications
The first generation of gadolinium-based agents are tracers of extracellular space and often are referred to as extracellular fluid (ECF) agents. The various ECF agents are almost indistinguishable from an efficacy perspective and, as a result, often are referred to by physicians as “gado” or “gadolinium.” They are used to detect or rule out lesions in the brain because of the disrupted blood-brain barrier in the presence of tumor. They are used to generate blood vessel images immediately when injection (dynamic first-pass angiography) occurs as well as for assessment of cerebral, myocardial, and renal perfusion. Although nonspecific, the ECF agents are used widely in clinical practice and are by far the most commonly used MRI contrast agents.
The ECF agents are eliminated almost exclusively via the kidneys. The next generation of contrast agents were designed for liver imaging (18). Three different approaches are seen in approved agents. SPIO such as AMI-25 (ferumoxide, Feridex, Bayer Healthcare, USA and Endorem, Guerbet, France) and SHU-555A (ferucarbotran and Resovist, Bayer-Schering, Germany) are recognized by the reticuloendothelial system and transported to Kuppfer cells in the liver. The SPIO make the normal-functioning liver appear dark. Tumors and fibrotic lesions do not take up the particles and appear bright on a T2-weighted image (Fig. ??). The Gd-based agents Gd-EOB- DTPA and Gd-BOPTA have mixed renal and hepatobiliary clearance. The complexes are taken up by hepatocytes and transported through the liver and gall bladder. Here, the healthy liver appears bright on a T1-weighted image, while lesions are not enhanced. The manganese compound Mn-DPDP (mangafodipir and Teslascan) is unstable with respect to transmetallation (19). The complex partially dissociates in plasma. Both the complex and free Mn2+ are taken up rapidly by the liver. In hepatocytes, the manganese ion binds to cellular proteins, which results in increased relaxivity. Like the Gd-based liver agents, the normal liver appears bright on a T1-weighted scan.
Although ECF agents are used for blood vessel imaging, the imaging must be done immediately after injection (so-called dynamic MRA). The blood concentration drops quickly with time as the agent both distributes outside the vessels into the interstitial space and is cleared via the kidney. There was a push to develop “blood pool” agents (20) that are present only in the vascular space to maximize blood:tissue contrast and that provide persistent contrast in the blood such that slightly longer, higher resolution scans can be used (the rapid imaging required with ECF agents sacrifices spatial resolution). Three approaches have been employed resulting in compounds that have progressed to the clinic or to clinical trials:
1. Serum albumin targeting: MS-325 was designed to bind reversibly to serum albumin. Albumin binding serves to localize the agent in the vascular space; it increases the relaxivity of the protein-bound complex, and the unbound fraction is available for renal clearance. MS-325 is approved for use in the EU and other countries. The bile acid-GdDTPA conjugate gadocoletic acid (a.k.a. B22956, Fig. ??) being developed by Bracco functions similarly; Phase II clinical trials have demonstrated its efficacy.
2. Increased size, Fig. ??: A different approach was taken with the compound Gadomer (also called Gadomer-17, Bayer Schering Pharma). Gadomer is a dendrimer with 24 gadolinium DO3A-monoamide chelates on the periphery of the dendrimer. Its size is large enough to restrict the dendrimer to the vascular compartment and to increase relaxivity relative to ECF agents, but it is still small enough to be renally eliminated. A related approach was taken by Guerbet with the compound P792 (gadomelitol, Vistarem, Guerbet, France). P792 is retained in the vascular space because of its size; the relaxivity is high because the gadolinium sits at the center of the molecule, which gives it a long correlation time.
3. USPIO: The ultrasmall iron oxide particles have good T1 relaxation properties, especially at lower fields (1.5 T). Their small size and coating enables them to evade the RES and remain in the blood pool; they are too large to extravasate. The dextran-coated formulation NC100150 was evaluated in multicenter trials and found to be effective, but ultimately, it was abandoned. The citrate-coated VSOP particle has entered Phase II trials.
The USPIO AMI-227 (ferumoxtran, Combidex, Advanced Magnetics, USA or Sinerem, Guerbet, France) has undergone clinical trials for lymph node imaging. In addition to being useful for angiography, these particles are trafficked slowly to the lymph nodes. A day after injection, normal-functioning lymph nodes appear dark on a T2-weighted image. If a tumor is present in the node, then it appears brighter because the cancer cells do not take up the iron particle. These particles also are taken up by macrophages and may prove useful as a marker of inflammatory response.
EP-2104R is a peptide-based agent that targets fibrin. Fibrin is an abundant component of blood clots (thrombi). The fibrin-specific peptide is conjugated to several gadolinium chelates to create a high-relaxivity, thrombus-specific contrast agent that worked well in animal models (21) of coronary, cardiac, and pulmonary thrombosis. Figure ?? shows an EP-2104R-enhanced image of a right atrial thrombus in a porcine model and highlights the difference between positive, T1-weighted contrast agents and negative, T2-weighted contrast agents (e.g., Fig. ??). Recently, this compound has entered clinical trials.
Newer agents
Apart from EP-2104R, the compounds described above rely on distribution and passive targeting for their imaging efficacy. Newer contrast agents are targeted actively. Some examples that have been studied in animal models are described below and shown in cartoon form in Fig. ??.
The Weissleder group (16, 17) have developed a platform technology based on iron oxide particles called cross-linked iron oxides (CLIO). These particles have amine groups on the surface that can be used to attach multiple targeting vectors as well as fluorochromes for multimodality (MRI, near IR) imaging. Examples from this group include particles targeted to vascular cell adhesion molecule (VCAM) for atherosclerotic plaque detection, particles targeted to E-selectin in cancer, particles targeted to mucin-1 expression (MUC-1) in cancer, and derivatized particles with annexin V for imaging apoptosis. Iron oxides usually provide higher sensitivity than gadolinium-based agents and, as mentioned above, extend their contrast-enhancing effect through space.
The Wickline/Lanza group (22) uses a perfluorocarbon emulsion as a contrast agent platform. Gadolinium chelates with lipophilic tails can incorporate into the emulsion such that thousands of Gd(III) ions per particle exist. Targeting is achieved by derivatizing a targeting vector (antibody, small molecule, peptide, etc.) with a lipid chain to incorporate into the emulsion. They have demonstrated targeting to thrombus and also to angiogenesis by targeting the integrin αv β3.
Considerable effort has been expended for imaging atherosclerosis using a variety of approaches (12, 23), in addition to those described above: gadolinium chelates noncovalently associated with high density lipoprotein (HDL), immunomicelles containing gadolinium chelates targeted to the macrophage scavenger receptor, and micelles formed from gadolinium chelates with perfluorocarbon chains.
Another approach has been to make the contrast agent responsive to its environment. The molecular parameters affecting relaxivity (hydration, tumbling time, and water exchange) can be altered by an enzymatic transformation, by pH change, or when binding an analyte (e.g., Ca or glucose). For instance, Meade and coworkers (24) developed a gadolinium complex that changed its relaxivity in the presence of the enzyme beta-galactosidase (Fig. ??). The complex has a galactose residue conjugated to it that blocks the access of water into the innercoordination sphere of the gadolinium. When the sugar is cleaved by the enzyme, relaxivity is enhanced and can be detected by MRI. Querol and Bogdanov (25) recently reviewed these amplification strategies.
Radiopharmaceuticals
A radiopharmaceutical is a pharmaceutical with a radioactive element incorporated in it. Radiopharmaceuticals that emit gamma rays are used for imaging, whereas those that emit alpha particles, beta particles, or Auger electrons are used for therapeutic purposes, mainly in cancer. Because most of the periodic table consists of metals, it is not surprising that many radionuclides with useful imaging or therapy properties are metallic. Therapeutic radiopharmaceuticals are outside the scope of this article but will be discussed where imaging is used to guide the therapy. The nuclear imaging agents described will be split into gamma emitters, such as 99mTc, and positron emitters, such as 64Cu.
Gamma ray (γ-ray) emitters
The most widely used metal-based imaging agent is based on the metastable isotope technetium-99m. The hexakis (isonitrile) 99mTc(I) complex, Tc-MIBI (Cardiolite, sestamibi) (Fig. ??), is used routinely for myocardial perfusion imaging to evaluate coronary artery disease. Imaging is done either in two dimensions or in three. Planar imaging with a gamma camera is a 2-D projection of the gamma rays emitted from a 3-D source (the patient) and is analogous to planar X-ray imaging. SPECT generates 3-D images by using a gamma camera to acquire multiple 2-D images from different angles and by reconstructing the image.
For gamma imaging, the ideal agent should have a half-life for decay on the order of the examination, and it should be eliminated from the body with a half-life on the order of the examination. This minimizes the radiation exposure to the patient. The isotope should be readily available for widespread use and should only emit γ-rays. The emission energy should be high enough (>50 keV) to penetrate tissue but low enough (<300 keV) that it is efficiently detectable by the camera. The agent should be easily prepared and on administration should be rapidly taken up by the area of interest with quick background clearance. 99mTc is the best isotope for γ-imaging based on its physical properties and availability; 99mTc is the isotope employed in about 80% of diagnostic nuclear medicine scans. It has a 6-hour half-life—long enough for straightforward manipulation, but short enough that it has passed 4 half-lives in a day. It decays solely by γ emission with an ideal energy for tissue penetration and detection, 141 keV. 99mTc is a decay product of 99Mo (t1/2 = 66 hr). The technetium generator consists of reactor-produced 99MoO42- immobilized on an anion exchange column encased in lead. Each day pertechnetate, 99mTcO4-, is produced, which can be eluted off the column. The generator provides a readily available on-site source of 99mTc to hospital radiopharmacies.
Applications of nuclear medicine imaging agents
The most common nuclear medicine procedure is myocardial perfusion imaging. Here, the imaging agent is administered while the patient is exercising (treadmill or bicycle) or given a drug to increase blood flow. The imaging agent is taken up rapidly by the heart muscle and retained there. Imaging is performed later, and the image reflects blood flow during exercise. Areas of reduced flow are indicative of coronary artery disease. Originally, the tracer used was the thallous ion as the chloride salt, 201Tl+, which enters myocytes through potassium ion channels. Thallium still is used, but the majority of exams are done with Tc agents, the most common being 99mTc-sestamibi and 99mTc-tetrafosmin (Myoview, GE Healthcare, USA) (Fig. ??). Figure ?? also shows approved brain and kidney perfusion agents. Bone imaging is done routinely to search for metastases. Bone-seeking agents are structurally ill-defined 99mTc complexes of pyrophosphate (PYP, also useful in imaging myocardial infarction), methylenediphosphonate (MDP), or hydroxmethylenediphosphonate (HDP). The 99mTc complex of DTPA is used in perfusion imaging. 99mTc also is coordinated directly to micron-sized aggregated particles of serum albumin for lung perfusion studies. 111In forms a lipophilic insoluble complex with 8-hydroxyquinoline (111In-oxine), and this complex is used to label white blood cells for infection imaging. 67Ga either as the citrate or nitrate behaves as a mimic of Fe3+ and has been used in imaging inflammation and tumors.
Initially, imaging agents were discrete metal-essential complexes. Increasingly, the metal is complexed by a bifunctional chelator that is tagged to a small molecule, peptide, or antibody-targeting group. Clinical examples include 99mTc-Arcitumomab, a Fab’ monoclonal antibody fragment directed toward the carcinoembryonic antigen (CEA) expressed on most colorectal cancers; mIn-DTPA labeled capromab antibody for imaging of prostate cancer and prostate metastases; 111In-DTPA conjugated to a synthetic peptide analog of somatostatin (111In-pentetreotide, Octreoscan, Covidien, USA) is used for the detection of cancers overexpressing the somatostatin receptor; 99mTc-P829 (NeoTect, Bayer Healthcare, USA), is a peptide-based analog of somatostatin with the 99mTc chelator built into the peptide (Fig. ??). An active research effort into Tc-tagged imaging agents is underway (26-29); Figure ?? illustrates tumor-targeted planar y-imaging in a mouse model using a Tc-tagged bombesin peptide fragment.
Receptor-targeted radiotherapy is a growing field. Imaging plays a key role in the efficacy of these therapeutic radiopharmaceuticals (30). Not all tumors express a given receptor, and in those that do, receptor density can vary in time and as a response to treatment. Imaging tumor uptake with a diagnostic analog can select patients for therapy and be used to monitor treatment. Imaging also can help with dosimetry because it is critical to deliver enough radiation to kill the tumor while minimizing damage to other organs or nearby bone marrow. 90Y is a pure y-emitter used in therapy. The chemistry of Y3+ and In3+ is similar enough that 111In often is incorporated for imaging studies. 177Lu is another isotope used in therapy, and it also emits a gamma with suitable energy for imaging.
Bioconjugate approaches for Tc and In labeling
The bioconjugate chemistry of technetium is more specialized (26-28) because of how the isotope is produced and because of the rich redox chemistry of technetium (oxidation states from — 1 to +7). Pertechnetate eluted from the generator sometimes is used for thyroid imaging, but for any other use the metal must be reduced and chelated. For clinical applications, a kit containing a ligand and a reducing agent must be produced that will yield a pure radiopharmaceutical when mixed with TcO4—. The most common oxidation states for medical applications are Tc(V) and Tc(I). A variety of donor atoms have been used to stabilize a given oxidation state (Fig. ?? gives a flavor). Many permutations exist of the co-ligands used, reducing agents, and methods for conjugation to the targeting vector; these are the subject of excellent review articles (26-29). For conciseness, the three most common bifunctional approaches are described.
The oxotechnetium core, [Tc = O]3+, in Tc(V) is readily accessible from stannous chloride reduction of pertechnetate. The Tc(V) oxidation state can be stabilized by thiolate, amide N, and amine N donors. As a result, many examples exist of NxS(4-x) ligands (see, e.g., Figs. ?? and ??) that form the base of square pyramidal complexes with Tc(V) where the oxo group is the pyramid apex. As Tc(V) is capable of deprotonating an amide N-H and coordinating to the amide nitrogen, amino acids make useful building blocks for NxS(4-x) ligands. The MAG3 ligand in Fig. ?? is assembled from mercaptoacetate coupled to three glycines. The resultant [Tc(O)(MAG3)] complex has a pendant carboxylate group that can be activated and coupled to the amine of a targeting vector. One can appreciate that ligands assembled from other amino acids would generate functionalizable side chains for conjugation, for example, as in the Tc(O)-depreotide complex shown in Fig. ??. In principle, one can form the Tc(V) complex and then couple to the targeting group (prelabeling technique). This process avoids exposing a potentially sensitive moiety to harsh reduction/chelation conditions and may be useful for proof-of-concept studies. However, for clinical use, usually it is preferred to conjugate the ligand first to the targeting group and to react this purified product with technetium for ease of use in the hospital setting.
Another widely used approach to targeting 99mTc is through the hydrazinonicotinic (HYNIC) technique (29). This approach involves reacting an activated ester of HYNIC acid with an amine group of the targeting moiety (peptide or protein) and purifying it. A Tc(V) oxo complex is prepared by Sn(II) reduction of TcO4- in the presence of a coligand such as tricine, mannitol, or glucoheptonate. Sometimes tri(phenylsulfonic acid)phosphine is used as a reducing agent and coligand. The HYNIC derivative then is reacted with this Tc(V) complex and the hydrazine group coordinates to the Tc, which displaces the oxo group as shown in Fig. ??. Labeling efficiencies are quite high, and the product can be quite stable with suitable choice of coligands. The coligand(s) can be varied to alter the lipophilicity/charge of the complex and to tune the pharmacokinetics. An important example of a HYNIC conjugate is the Tc-HYNIC-(Annexin V) conjugate for imaging apoptosis (31).
The fac-[Tc(CO)3(H2O)]+ cation is a versatile synthon for labeling (32). It is prepared quantitatively from boranocarbonate ([H3B-CO2H]-) and TcO4-. The complex is water-soluble and readily undergoes aquo ligand exchange with mono-, bi-, or tri-dentate ligands, whereas the Tc(CO)3 fragment is chemically robust under a range of conditions. Originally, this exchange was used to label histidine on the N- or C-terminus of a peptide where the terminal amine (or carboxylate) and the imidazole N of the histidine coordinated to the technetium. This technology has been used to provide one-step labeling of recombinant proteins that contain His-tags (33). Using a bidentate link allows the introduction of an additional monodentate ligand to alter the lipophilicity/charge; however, the bidentate link was found to be less stable in vivo and, subsequently, tridentate ligands have been employed. The single amino acid chelator (SAAC) approach (34) involves a protected unnatural amino acid that contains a tridentate chelator as shown in Fig. ??. The SAAC can be incorporated into the targeting peptide at any point using solid-phase peptide synthesis and represents a smaller perturbation to the peptide compared with the NxS(4-x) chelators. Labeling with Tc is quick, after the [Tc(CO)3(H2O)]+ has been prepared.
In-111 often is used for initial proof-of-concept studies or as an imaging surrogate for radiotherapuetics such as 90Y. The +3 oxidation state is the only relevant oxidation state for aqueous indium chemistry. Indium complexes have coordination numbers from six to eight, and ligands used in medicine to chelate Y3+ and the lanthanides (e.g., Gd3+ and Lu3+) also form stable complexes with In3+. The ligand is conjugated first to the targeting group (protein, peptide, etc.), and this conjugate is reacted with mInCl3. The ligand is based usually on DTPA or DOTA and is derivatized such that it can react selectively with an amine, a thiol, or a carboxylic acid. This bioconjugation chemistry and these synthons also are useful for designing targeted 90Y or 177Lu complexes for therapy or gadolinium complexes for MRI.
Positron emission tomography (PET)
Radionuclides that decay by positron emission also are detectable with a gamma camera. The positron undergoes an annihilation reaction with an electron in tissue resulting in two gamma rays (511 keV) being emitted at 180° apart. PET scanning involves acquiring a series of 2-D images at different orientations and reconstructing them to give a 3-D image. PET imaging has the benefit of higher resolution than SPECT and also offers the potential for getting quantitative data. This quantitative aspect has been exploited in obtaining absolute measures of blood perfusion as well as in determining receptor occupancy numbers. A resurgence of PET has occurred in recent years mainly because of the success of 18F-fluorodeoxyglucose (FDG) in oncology and the development of the combined PET/CT scanner. PET/CT provides a high resolution CT anatomical image onto which the lower resolution molecular image of the PET tracer is superimposed.
The majority of PET research involves 18F (t3/2 = 110 min) and nC (t1/2 = 20 min). With considerable effort, these isotopes can be incorporated into organic molecules such as hormones or drugs. The benefit is that the tracer does not alter the pharmacokinetics of the molecule being labeled in the same way that the conjugation of a metal complex will. Nevertheless, applications of metallic PET tracers exist. Rubidium-82 (t3/2 = 1.27 min) has a very short half-life but is easily obtained from a strontium-82 generator. The rubidium ion is a potassium analog, and 82Rb+ is used in myocardial perfusion studies.
Although useful, rubidium is limited in half-life and chemistry. The other more studied PET metal isotopes are 68Ga (t3/2 = 68 minutes) and 64Cu (t3/2 = 12.7 hours). 68Ga can be produced on site by a generator. 64Cu production requires a cyclotron, but its relatively long half-life allows it to be shipped from a central source. Most in vivo work with 68Ga has involved targeting the somatostatin receptor with a peptide-gallium conjugate (35). Often a DOTA derivative is used to chelate the 68Ga, but the hexadentate NOTA ligand (Fig. ??) also offers high stability.
The thiosemicarbazone complexes 64CuPTSM and 64CuA- TSM, Fig. ??, have been used to image perfusion and hypoxia, respectively (36). It is believed that these compounds freely diffuse into cells. Reduction from Cu(II) to Cu(I) inside the cell causes the complex to fall apart, and the copper is trapped inside the cell. The redox potential of CuATSM is lower than that of CuPTSM, and this redox potential is believed to be the root of the selectivity of CuATSM for hypoxic tissue.
Copper complexes also are used as bifunctional chelators (37), however, transmetallation remains an issue. The CuDOTA complex is known to lose copper in vivo. Increasing the macrocycle size by two carbons (cyclen to cyclam) to give TETA results in a more stable/inert complex. Cross-bridged macrocycles also have been used to give more inert complexes. However, it is important to have facile incorporation of the copper into the chelate, and some ligands giving more stable complexes do not exhibit efficient/mild labeling kinetics. The coordination chemistry here still is evolving (37). Several in vivo studies have been reported that involve bifunctional 64Cu compounds that are targeted, for example, to vascular endothelial growth factor (VEGF) receptor (38), to malignant melanoma (39), or to the αv β3 integrin (40) for tumor detection or for monitoring cancer therapy.
Conclusions
Metal-based imaging agents comprise a broad and growing field with compounds ranging from simple aqua ions to small molecules to supramolecular assemblies and nanoparticles. The imaging modality and chemical approach to the agent are best chosen based on the question that needs to be addressed by imaging. The imaging field continues to embrace advances in chemical biology to meet the challenges of in vivo imaging: the diagnosis and etiology of disease, the characterization of the disease at the molecular level, understanding the metabolic pathways, and monitoring the response to therapy.
References
1. Esteban JM, Alonso A, Cervera V, Martinez V. One-molar gadolinium chelate (gadobutrol) as a contrast agent for CT angiography of the thoracic and abdominal aorta. Eur. Radiol. 2007; 17:2394-2400.
2. Krause W, Schuhmann-Giampieri G, Bauer M, Press WR, Muschick P. Ytterbium-and dysprosium-EOB-DTPA. A new prototype of liver-specific contrast agents for computed tomography. Invest. Radiol. 1996; 31:502-511.
3. Rabin O, Manuel Perez J, Grimm J, Wojtkiewicz G, Weissleder R. An X-ray computed tomography imaging agent based on long-circulating bismuth sulphide nanoparticles. Nat. Mater. 2006; 5:118-122.
4. Kattumuri V, Katti K, Bhaskaran S, Boote EJ, Casteel SW, Fent GM, Robertson DJ, Chandrasekhar M, Kannan R, Katti KV. Gum arabic as a phytochemical construct for the stabilization of gold nanoparticles: in vivo pharmacokinetics and x-ray-contrast-imaging studies. Small 2007; 3:333-341.
5. Yu SB, Watson AD. Metal-based X-ray contrast media. Chem. Rev. 1999; 99:2353-2378.
6. Caravan P.Strategies for increasing the sensitivity of gadolinium based MRI contrast agents. Chem. Soc. Rev. 2006; 35:512-523.
7. Jaszberenyi Z, Sour A, Toth E, Benmelouka M, Merbach AE. Fine-tuning water exchange on Gd(III) poly(amino carboxylates) by modulation of steric crowding. Dalton Trans. 2005; (16):2713-2719.
8. Werner EJ, Avedano S, Botta M, Hay BP, Moore EG, Aime S, Raymond KN. Highly soluble tris-hydroxypyridonate Gd(III) complexes with increased hydration number, fast water exchange, slow electronic relaxation, and high relaxivity. J. Am. Chem. Soc. 2007; 129:1870-1871.
9. Raymond KN, Pierre VC. Next generation, high relaxivity gadolinium MRI agents. Bioconjug. Chem. 2005; 16:3-8.
10. Gianolio E, Giovenzana GB, Longo D, Longo I, Menegotto I, Aime S. Relaxometric and modelling studies of the binding of a lipophilic Gd-AAZTA complex to fatted and defatted human serum albumin. Chemistry 2007; 13:5785-5797.
11. Kobayashi H, Brechbiel MW. Nano-sized MRI contrast agents with dendrimer cores. Adv. Drug Deliv. Rev. 2005; 57:2271-2286.
12. Amirbekian V, Lipinski MJ, Briley-Saebo KC, Amirbekian S, Aguinaldo JG, Weinreb DB, Vucic E, Frias JC, Hyafil F, Mani V, Fisher EA, Fayad ZA. Detecting and assessing macrophages in vivo to evaluate atherosclerosis noninvasively using molecular MRI. Proc. Natl. Acad. Sci. U.S.A. 2007; 104:961-966.
13. Mulder WJ, Strijkers GJ, van Tilborg GA, Griffioen AW, Nicolay K. Lipid-based nanoparticles for contrast-enhanced MRI and molecular imaging. NMR Biomed. 2006; 19:142-164.
14. Zhang Z, Greenfield MT, Spiller M, McMurry TJ, Lauffer RB, Caravan P. Multilocus binding increases the relaxivity of protein-bound MRI contrast agents. Angew. Chem. Int. Ed. Engl. 2005; 44:6766-6769.
15. Thorek DL, Chen AK, Czupryna J, Tsourkas A. Superparamagnetic iron oxide nanoparticle probes for molecular imaging. Ann. Biomed. Eng. 2006; 34:23-38.
16. Schellenberger EA, Sosnovik D, Weissleder R, Josephson L. Magneto/optical annexin V, a multimodal protein. Bioconjug. Chem. 2004; 15:1062-1067.
17. Sosnovik DE, Weissleder R. Emerging concepts in molecular MRI. Curr. Opin. Biotechnol. 2007; 18:4-10.
18. Weinmann HJ, Ebert W, Misselwitz B, Schmitt-Willich H. Tissue- specific MR contrast agents. Eur. J. Radiol. 2003; 46:33-44.
19. Gallez B, Bacic G, Swartz HM. Evidence for the dissociation of the hepatobiliary MRI contrast agent Mn-DPDP. Magn. Reson. Med. 1996; 35:14-19.
20. Mohs AM, Lu ZR. Gadolinium(III)-based blood-pool contrast agents for magnetic resonance imaging: status and clinical potential. Expert Opin. Drug Deliv. 2007; 4:149-164.
21. Spuentrup E, Buecker A, Katoh M, Wiethoff AJ, Parsons EC. Jr, Botnar RM, Weisskoff RM, Graham PB, Manning WJ, Gunther RW. Molecular magnetic resonance imaging of coronary thrombosis and pulmonary emboli with a novel fibrin-targeted contrast agent. Circulation 2005; 111:1377-1382.
22. Winter PM, Caruthers SD, Yu X, Song SK, Chen J, Miller B, Bulte JW, Robertson JD, Gaffney PJ, Wickline SA, Lanza GM. Improved molecular imaging contrast agent for detection of human thrombus. Magn. Reson. Med. 2003; 50:411-416.
23. Barkhausen J, Ebert W, Heyer C, Debatin JF, Weinmann HJ. Detection of atherosclerotic plaque with Gadofluorine-enhanced magnetic resonance imaging. Circulation 2003; 108:605-609.
24. Louie AY, Huber MM, Ahrens ET, Rothbacher U, Moats R, Jacobs RE, Fraser SE, Meader TJ. In vivo visualization of gene expression using magnetic resonance imaging. Nat. Biotechnol. 2000; 18:321-325.
25. Querol M, Bogdanov A Jr. Amplification strategies in MR imaging: activation and accumulation of sensing contrast agents (SCAs). J. Magn. Reson. Imaging 2006; 24:971-982.
26. Banerjee SR, Maresca KP, Francesconi L, Valliant J, Babich JW, Zubieta J. New directions in the coordination chemistry of 99mTc: a reflection on technetium core structures and a strategy for new chelate design. Nucl. Med. Biol. 2005; 32:1-20.
27. Liu S.The role of coordination chemistry in the development of target-specific radiopharmaceuticals. Chem. Soc. Rev. 2004; 33:445-461.
28. Liu S, Edwards DS. 99mTc-Labeled small peptides as diagnostic radiopharmaceuticals. Chem. Rev. 1999; 99:2235-2268.
29. Liu, S.6-Hydrazinonicotinamide derivatives as bifunctional coupling agents for 99mTc-labeling of small biomolecules. Top. Curr. Chem. 2005; 252:117-153.
30. Panigone S, Nunn AD. Lutetium-177-labeled gastrin releasing peptide receptor binding analogs: a novel approach to radionuclide therapy. Quart. J. Nucl. Med. Mol. Imaging 2006; 50:310-321.
31. Boersma HH, Kietselaer BL, Stolk LM, Bennaghmouch A, Hofstra L, Narula J, Heidendal GA, Reutelingsperger CP. Past, present, and future of annexin A5: from protein discovery to clinical applications. J. Nucl. Med. 2005; 46:2035-2050.
32. Alberto R, Pak JK, van Staveren D, Mundwiler S, Benny P. Mono-, bi-, or tridentate ligands? The labeling of peptides with 99mTc-carbonyls. Biopolymers 2004; 76:324-333.
33. Waibel R, Alberto R, Willuda J, Finnern R, Schibli R, Stichelberger A, Egli A, Abram U, Mach JP, Pluckthun A, Schubiger PA. Stable one-step technetium-99m labeling of His-tagged recombinant proteins with a novel Tc(I)-carbonyl complex. Nat. Biotechnol. 1999; 17:897-901.
34. Stephenson KA, Banerjee SR, Sogbein OO, Levadala MK, Mc-Farlane N, Boreham DR, Maresca KP, Babich JW, Zubieta J, Valliant JF. A new strategy for the preparation of peptide-targeted technetium and rhenium radiopharmaceuticals. The automated solid-phase synthesis, characterization, labeling, and screening of a peptide-ligand library targeted at the formyl peptide receptor. Bioconjug. Chem. 2005; 16:1189-1195.
35. Maecke HR, Hofmann M, Haberkorn U. (68)Ga-labeled peptides in tumor imaging. J. Nucl. Med. 2005; 46(suppl 1):172S-178S.
36. Anderson CJ, Welch MJ. Radiometal-labeled agents (non-technetium) for diagnostic imaging. Chem. Rev. 1999; 99:2219-2234.
37. Wadas TJ, Wong EH, Weisman GR, Anderson CJ. Copper chelation chemistry and its role in copper radiopharmaceuticals. Curr. Pharm. Des. 2007; 13:3-16.
38. Cai W, Chen K, Mohamedali KA, Cao Q, Gambhir SS, Rosenblum MG, Chen X. PET of vascular endothelial growth factor receptor expression. J. Nucl. Med. 2006; 47:2048-2056.
39. Wei L, Butcher C, Miao Y, Gallazzi F, Quinn TP, Welch MJ, Lewis JS. Synthesis and biologic evaluation of 64Cu-labeled rhenium-cyclized alpha-MSH peptide analog using a cross-bridged cyclam chelator. J. Nucl. Med. 2007; 48:64-72.
40. Wu Y, Zhang X, Xiong Z, Cheng Z, Fisher DR, Liu S, Gambhir SS, Chen X. microPET imaging of glioma integrin avb3 expression using (64)Cu-labeled tetrameric RGD peptide. J. Nucl. Med. 2005; 46:1707-1718.
Further Reading
The thematic Chemical Reviews issue on metals in medicine from 1999 contains several thorough reviews on X-ray, MRI, and nuclear imaging probes. These reviews are cited here (Refs. 5, 6, 29, 36) and provide an excellent background on these topics and a good point from which to appreciate current literature.
Werner Krause has edited three recent volumes (221, 222, 252) in the Topics in Current Chemistry series that covers imaging agents in all modalities.
Edelman RR, Hesselink JR, Zlatkin MB, Crues JV, eds. Clinical Magnetic Resonance Imaging. 3rd edition. 2005. Saunders, Philadelphia. This text has well-written chapters on MR physics and techniques, contrast agents, and clinical practice.
See Also
Imaging Techniques: Overview of Applications in Chemical Biology
Metals in Medicine: Therapeutic Agents