MCAT Biology Review
Chapter 8: The Immune System
8.2 The Innate Immune System
The innate immune system consists of cells and structures that offer nonspecific protection.
NONCELLULAR NONSPECIFIC DEFENSES
Our first line of defense is the skin (integument). In Chapter 10 of MCAT Biology Review, we will discuss the more specific homeostatic functions of the skin; for now, we’ll focus on how skin protects the body. The skin provides a physical barrier between the outside world and our internal organs, excluding most bacteria, viruses, fungi, and parasites from entering the body. Additionally, antibacterial enzymes called defensins can be found on the skin. Sweat also has antimicrobial properties. The skin is an important first line of defense: a cut or abrasion on the skin provides an entry point for pathogens into the body. Deeper wounds allow pathogens to penetrate deeper into the body.
As discussed in Chapter 6 of MCAT Biology Review, the respiratory system also has mechanisms to prevent pathogens from entering the body. The respiratory passages are mucous membranes, lined with cilia to trap particulate matter and push it up toward the oropharynx, where it can be swallowed or expelled. While mucus helps to trap particulates like smoke and dirt, it also helps to prevent bacteria and viruses from gaining access to the deep lung tissue. Several other mucous membranes, including around the eye and in the oral cavity, produce a nonspecific bacterial enzyme called lysozyme, which is secreted in tears and saliva, respectively.
The Gastrointestinal Tract
The gastrointestinal tract also plays a role in nonspecific immunity. First, the stomach secretes acid, resulting in the elimination of most pathogens. In addition, the gut is also colonized by bacteria. Most of these bacteria lack the necessary characteristics to cause infection. Because there is already such a large bacterial population in the gut, many potential invaders are not able to compete and are thus kept at bay. Many antibiotics reduce the population of gut flora, thus providing an opportunity for the growth of pathogens.
REAL WORLD
The GI tract of a newborn baby is particularly susceptible to infection because the newborn’s immune system is underdeveloped and the GI tract is not yet colonized. Breast milk contains a family of antibodies that are particularly effective on mucosal surfaces and helps to defend newborn babies against gastrointestinal infections.
Complement
The complement system consists of a number of proteins in the blood that act as a nonspecific defense against bacteria. Complement can be activated through a classical pathway (which requires the binding of an antibody to a pathogen) or an alternative pathway (which does not require antibodies). The complement proteins punch holes in the cell walls of bacteria, making them osmotically unstable. Despite the association with antibodies, complement is considered a nonspecific defense because it cannot be modified to target a specific organism over others.
Interferons
To protect against viruses, cells that have been infected with viruses produce interferons, proteins that prevent viral replication and dispersion. Interferons cause nearby cells to decrease production of both viral and cellular proteins. They also decrease the permeability of these cells, making it harder for a virus to infect them. In addition, interferons upregulate MHC class I and class II molecules, resulting in increased antigen presentation and better detection of the infected cells by the immune system, as described in the next section. Interferons are responsible for many “flu-like” symptoms that occur during viral infection, including malaise, tiredness, muscle soreness, and fever.
CELLS OF THE INNATE IMMUNE SYSTEM
So, what happens when bacteria, viruses, fungi, or parasites breach these defenses? The cells of the innate immune system are always poised and ready to attack.
Macrophages
Macrophages, a type of agranulocyte, reside within the tissues. These cells derive from blood-borne monocytes and can become a resident population within a tissue (becoming a permanent, rather than transient cell group in the tissue). Many of these resident macrophages are highlighted throughout MCAT Biology Review, including microglia in the central nervous system, Langerhans cells in the skin, and osteoclasts in bone. When a bacterial invader enters a tissue, the macrophages become activated. The activated macrophage does three things. First, it phagocytizes the invader through endocytosis. Then, it digests the invader using enzymes. Finally, it presents little pieces of the invader (mostly peptides) to other cells using a protein called major histocompatibility complex (MHC). MHC binds to a pathogenic peptide (also called an antigen) and carries it to the cell surface, where it can be recognized by cells of the adaptive immune system. In addition, macrophages release cytokines—chemical substances that stimulate inflammation and recruit additional immune cells to the area.
MHC molecules come in two main classes: class I and class II. All nucleated cells in the body display MHC class I molecules. Any protein produced within a cell can be loaded onto MHC-I and presented on the surface of the cell, as shown in Figure 8.4. This allows the immune system to monitor the health of these cells and to detect if the cells have been infected with a virus or another intracellular pathogen; only those cells that are infected would be expected to present an unfamiliar (nonself) protein on their surface. Therefore, the MHC-I pathway is often called theendogenous pathway because it binds antigens from inside the cell. Cells that have been invaded by intracellular pathogens can then be killed by a certain group of T-cells (cytotoxic T-lymphocytes) to prevent infection of other cells.
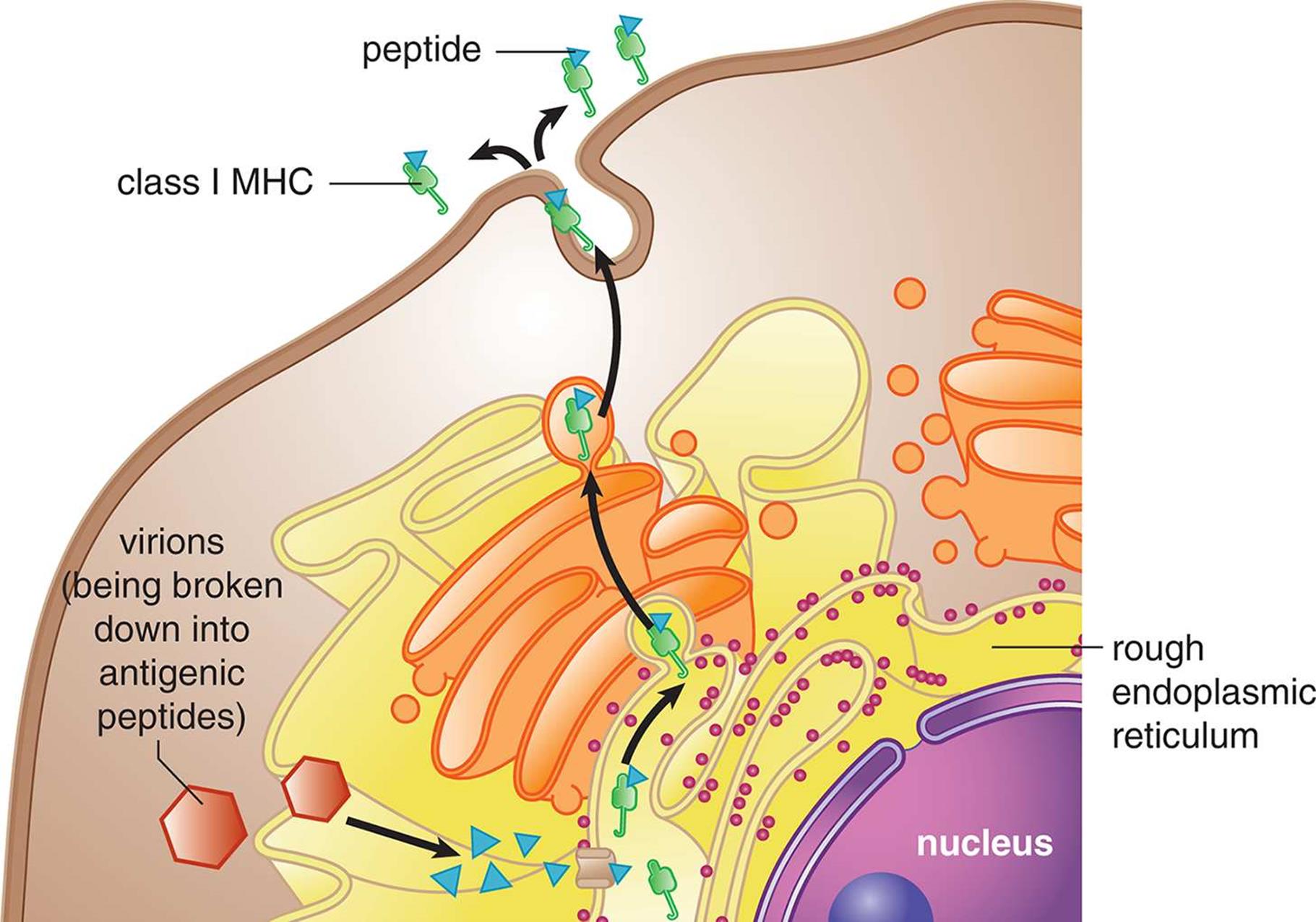 Figure 8.4. Endogenous Pathway for Antigen Presentation (MHC Class I) MHC-I exists in all nucleated cells.
Figure 8.4. Endogenous Pathway for Antigen Presentation (MHC Class I) MHC-I exists in all nucleated cells.
REAL WORLD
MHC molecules are highly variable among humans, but can usually be divided into particular subtypes. People with certain MHC subtypes have different susceptibility to disease, and some subtypes are considerably more susceptible to autoimmune diseases. It is also important to match the MHC types of the donor and recipient as closely as possible during transplants to avoid rejection of the graft.
MHC class II molecules are mainly displayed by professional antigen-presenting cells like macrophages, as shown in Figure 8.5. Remember that these phagocytic cells pick up pathogens from the environment, process them, and then present them on MHC-II. An antigen is a substance (usually a pathogenic protein) that can be targeted by an antibody. While antibody production is the domain of the adaptive immune system, it is important to understand that cells of the innate immune system also present antigens. Because these antigens originated outside the cell, this pathway is often called the exogenous pathway. The presentation of an antigen by an immune cell may result in the activation of both the innate and adaptive immune systems. Professional antigen-presenting cells include macrophages, dendritic cells in the skin, some B-cells, and certain activated epithelial cells.
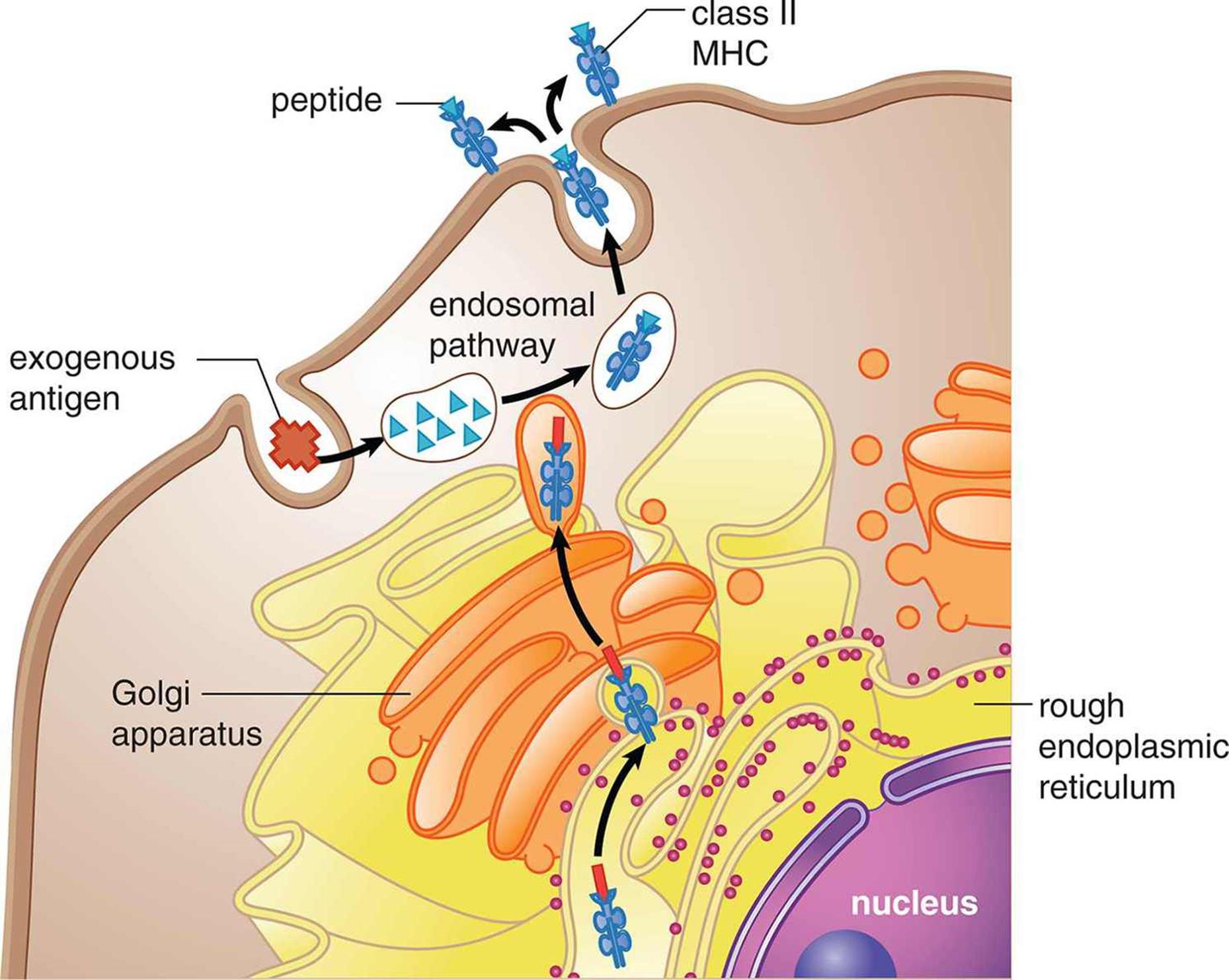 Figure 8.5. Exogenous Pathway for Antigen Presentation (MHC Class II) MHC-II exists only in professional antigen-presenting cells, like macrophages, dendritic cells, some B-cells, and some activated epithelial cells.
Figure 8.5. Exogenous Pathway for Antigen Presentation (MHC Class II) MHC-II exists only in professional antigen-presenting cells, like macrophages, dendritic cells, some B-cells, and some activated epithelial cells.
KEY CONCEPT
Major histocompatibility complex molecules are joined with antigens. The MHC–antigen complex then goes to the cell surface to display the antigen. This allows the immune system to monitor the health of cells. MHC-I is in all nucleated cells and presents endogenous antigens. MHC-II is in antigen-presenting cells and presents exogenous antigens.
Macrophages and dendritic cells also have special receptors known as pattern recognition receptors (PRR), the best-described of which are toll-like receptors (TLR). PRRs are able to recognize the category of the invader (bacterium, virus, fungus, or parasite). This allows for the production of appropriate cytokines to recruit the right type of immune cells; each immune cell has different weapons that can target particular groups of pathogens.
Natural Killer Cells
In the arms race between the human immune system and pathogens, some pathogens have found ways to avoid certain defenses. For example, some viruses cause downregulation of MHC molecules, making it harder for T-cells to recognize the presence of an infection. Natural killer (NK)cells, a type of nonspecific lymphocyte, are able to detect the downregulation of MHC and induce apoptosis in these virally infected cells. Cancer cells may also downregulate MHC production, so NK cells also offer protection from the growth of cancer as well.
Granulocytes
In addition to macrophages, the granulocytes, which include neutrophils, eosinophils, and basophils (and closely related mast cells) are also involved in nonspecific defense. Neutrophils are the most populous leukocyte in blood and are very short-lived (a bit more than five days). These cells are phagocytic, like macrophages, and target bacteria. Neutrophils can literally follow bacteria using chemotaxis—the sensing of certain products given off by bacteria and migration of neutrophils to follow these products back to the source (the bacterium itself). Neutrophils can also detect bacteria once they have been opsonized (marked with an antibody from a B-cell). Other cells, like natural killer cells, macrophages, monocytes, and eosinophils, also contain receptors for antibodies and can attack opsonized bacteria. Dead neutrophil collections are responsible for the formation of pus during an infection.
Eosinophils contain bright red-orange granules and are primarily involved in allergic reactions and invasive parasitic infections. Upon activation, eosinophils release large amounts of histamine, an inflammatory mediator. This results in vasodilation and increased leakiness of the blood vessels, allowing additional immune cells (especially macrophages and neutrophils) to move out of the bloodstream and into the tissue. Inflammation is particularly useful against extracellular pathogens, including bacteria, fungi, and parasites.
KEY CONCEPT
Histamine causes inflammation by inducing vasodilation and the movement of fluid and cells from the bloodstream into tissues.
Finally, basophils contain large purple granules and are involved in allergic responses. They are the least populous leukocyte in the bloodstream under normal conditions. Mast cells are closely related to basophils, but have smaller granules and exist in the tissues, mucosa, and epithelium. Both basophils and mast cells release large amounts of histamine in response to allergens, leading to inflammatory responses.
The functions of many cell types of both the innate and adaptive immune systems are highlighted in Figure 8.6.
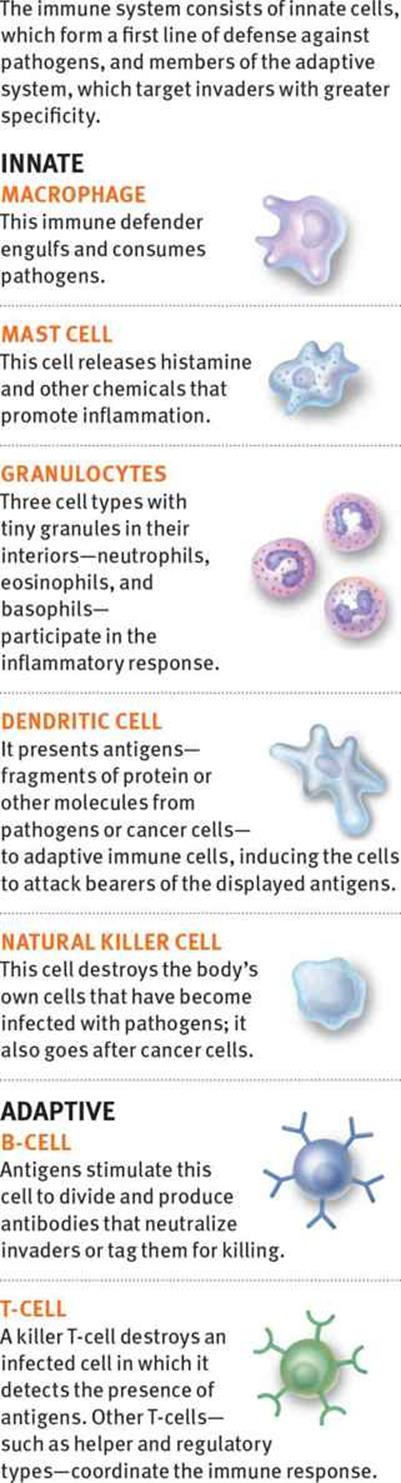 Figure 8.6. Cells of the Immune System
Figure 8.6. Cells of the Immune System
MCAT Concept Check 8.2:
Before you move on, assess your understanding of the material with these questions.
1. For each of the noncellular nonspecific immune defenses listed below, provide a brief description of its immunologic function:
· Skin:
· Defensins:
· Lysozyme:
· Mucus:
· Stomach acid:
· Normal gastrointestinal flora:
· Complement:
2. Which cells in the innate immune response are professional antigen-presenting cells?
3. What are the differences between MHC-I and MHC-II?
· MHC-I:
· MHC-II:
4. What stimulus activates each of the following types of cells?
· Natural killer cells:
· Neutrophils:
· Eosinophils:
· Basophils and mast cells: