MCAT Biology Review
Chapter 10: Homeostasis
10.2 Skin
By both weight and size, the skin (integument) is the largest organ in our bodies. It makes up about 16 percent of total body weight, on average. Skin is one of the major components of nonspecific immune defense, protecting us from exposure to the elements and invasion by pathogens.
STRUCTURE
The skin has several layers. Starting from the deepest layer and working outward, these layers are the hypodermis (subcutaneous layer), dermis, and epidermis, as shown in Figure 10.6. Skin is derived from the ectoderm.
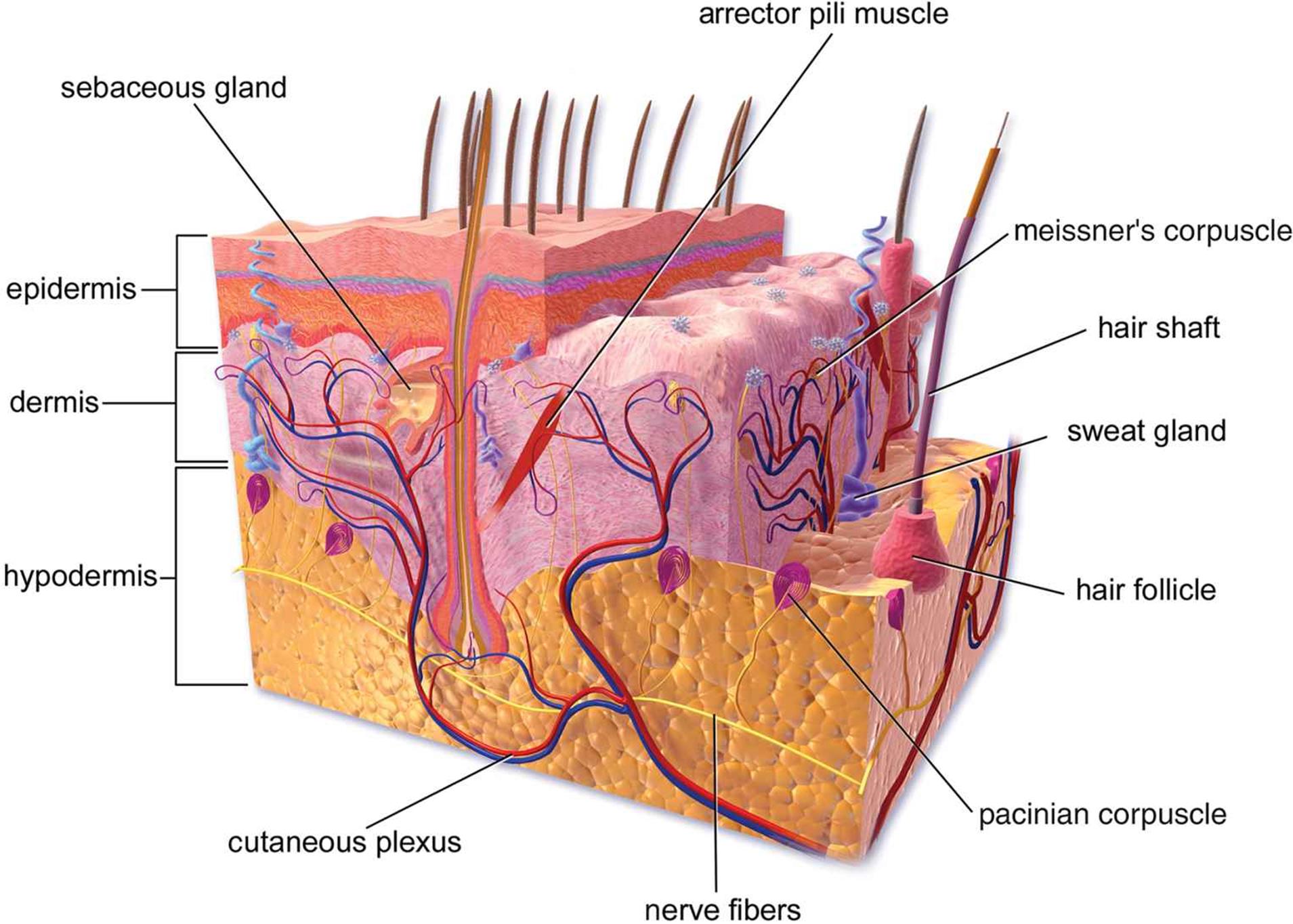 Figure 10.6. Anatomy of the Skin and Subcutaneous Tissue
Figure 10.6. Anatomy of the Skin and Subcutaneous Tissue
The Epidermis
The epidermis is also subdivided into layers called strata. From the deepest layer outward, these are the stratum basale, stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum, as shown in Figure 10.7. The stratum basale contains stem cells and is responsible for proliferation of keratinocytes, the predominant cells of the skin that produce keratin. In the stratum spinosum, these cells become connected to each other; this layer is also the site of Langerhans cells, described below. In the stratum granulosum, the keratinocytes die and lose their nuclei. The stratum lucidum is only present in thick, hairless skin, such as the skin on the sole of the foot or the palms, and is nearly transparent. Finally, the stratum corneum contains up to several dozen layers of flattened keratinocytes, forming a barrier that prevents invasion by pathogens and that helps to prevent loss of fluids and salt. Hair projects above the skin, and there are openings for sweat and sebaceous glands.
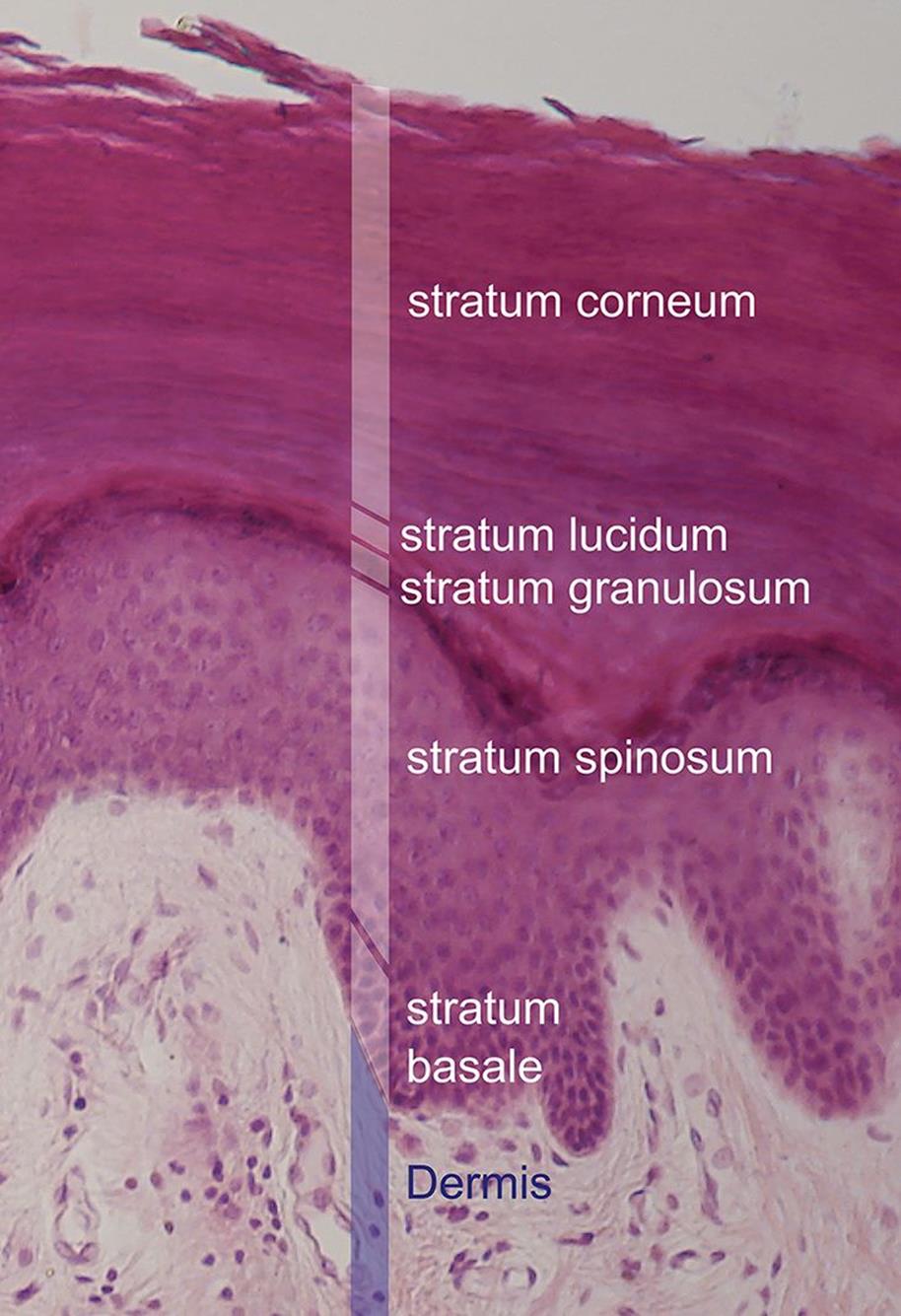 Figure 10.7. Layers of the Epidermis
Figure 10.7. Layers of the Epidermis
MNEMONIC
Layers of the skin (superficial to deep): Come, Let’s Get Sun Burned
· Stratum corneum
· Stratum lucidum
· Stratum granulosum
· Stratum spinosum
· Stratum basale
Other Cells of the Epidermis
In the epidermis, the main cells are keratinocytes. Keratin, mentioned above, is resistant to damage and provides protection against injury, water, and pathogens. Calluses form from excessive keratin deposition in areas of repeated strain due to friction; they provide protection to avoid damage in the future. Fingernails and hair are also formed from keratin and are produced by specialized cells in the skin.
REAL WORLD
People who have albinism suffer from a genetic metabolic disorder characterized by the inability to synthesize melanin. Typically, albinism is inherited in an autosomal recessive fashion. As would be expected, patients with albinism are extremely sensitive to the harmful effects of the sun. Depigmentation can also occur in vitiligo, an autoimmune disorder in which melanocytes are killed by the individual’s immune system.
Melanocytes are a cell type derived from neural crest cells and found in the stratum basale. These cells produce melanin, a pigment that serves to protect the skin from DNA damage caused by ultraviolet radiation. Once produced, the pigment is passed to the keratinocytes. All humans actually have comparable numbers of melanocytes; skin color is caused by varying levels of activity of the melanocytes. More active melanocytes result in darker skin tones. Upon exposure to ultraviolet radiation, melanocytes increase activity, resulting in a darker skin color.
Langerhans cells are actually special macrophages that reside within stratum spinosum. These cells are capable of presenting antigens to T-cells in order to activate the immune system.
The Dermis
The dermis also consists of multiple layers. The upper layer (right below the epidermis) is the papillary layer, which consists of loose connective tissue. Below the papillary layer is the denser reticular layer. Sweat glands, blood vessels, and hair follicles originate in the dermis.
Most sensory cells are also located in the dermis. Merkel cells (discs), for example, are sensory cells present at the epidermal–dermal junction. These cells are connected to sensory neurons and are responsible for deep pressure and texture sensation within the skin. Other sensory organs in the skin include free nerve endings, which respond to pain; Meissner’s corpuscles, which respond to light touch; Ruffini endings, which respond to stretch; and Pacinian corpuscles, which respond to deep pressure and vibration.
The Hypodermis
Finally, the hypodermis is a layer of connective tissue that connects the skin to the rest of the body. This layer contains fat and connective tissue.
THERMOREGULATION
We have already mentioned that the skin protects us from the elements and microbes. It also has other functions, including ultraviolet protection (via melanin) and transduction of sensory information from the outside world. In this section, we look at another function of the skin: thermoregulation.
BRIDGE
Evaporation is an endothermic process and, thus, absorbs energy from the surroundings to undergo this phase change. Further, the presence of dissolved solutes in sweat increases the boiling point of sweat slightly in comparison to pure water; this allows the absorption of even more heat energy. Boiling point elevation is a colligative property that is discussed in Chapter 9 of MCAT General Chemistry Review.
Thermoregulation is achieved by sweating, piloerection, vasodilation, and vasoconstriction. Sweating is an excellent cooling mechanism that is controlled by the autonomic nervous system. When body temperature rises above the set point determined by the hypothalamus, then thermoregulation processes must occur in order to rid the body of heat. Postganglionic sympathetic neurons that utilize acetylcholine innervate sweat glands and promote the secretion of water with certain ions onto the skin. Heat is then absorbed from the body as the molecules within the water undergo a phase change to evaporate. The production of sweat itself is not the main mechanism of cooling; it is the evaporation of water from the skin, which absorbs body heat. At the same time, arteriolar vasodilation occurs to maximize heat loss. This brings a large quantity of blood to the skin, which accelerates the evaporation of sweat by maximizing the heat energy available for the liquid–gas phase change.
BRIDGE
The neurons that innervate sweat glands are actually very unusual. Unlike all other postganglionic sympathetic neurons, these neurons are cholinergic—not adrenergic (that is, they release acetylcholine, not norepinephrine). All preganglionic neurons in the autonomic nervous system and postganglionic neurons in the parasympathetic nervous system are cholinergic as well. These neurons are discussed in Chapter 4 of MCAT Biology Review.
In cold conditions, arrector pili muscles contract, causing the hairs of the skin to stand up on end (piloerection). This helps to trap a layer of heated air near the skin. The arterioles that feed the capillaries of the skin constrict, limiting the quantity of blood reaching the skin. Skeletal muscle may also begin to contract rapidly, causing shivering. Shivering requires a sizeable amount of ATP; however, a significant portion of the energy from ATP is lost as heat. In addition to these mechanisms, humans possess a layer of fat just below the skin. This fat helps to insulate the body. In addition to this fat, which is called white fat, brown fat may also be present, especially in infants. Brown fat has a much less efficient electron transport chain, which means that more heat energy is released as fuel is burned.
The skin also helps to maintain the osmolarity of the body. This is because the skin is relatively impermeable to water. This prevents not only the entrance of water through the skin, but also the loss of water from the tissues. This becomes very important in cases such as burns or large losses of skin as dehydration of the tissues becomes a real threat to survival.
MCAT Concept Check 10.2:
Before you move on, assess your understanding of the material with these questions.
1. What is the predominant cell type in the epidermis?
2. What are the layers of the epidermis, from superficial to deep?
·
·
·
·
·
3. What are the layers of the dermis, from superficial to deep?
·
·
4. What are some mechanisms the body uses to cool itself? What are some mechanisms the body uses to retain heat?
· Cooling:
· Retaining heat: