THE LIVING WORLD
Unit Six. Animal Life
23.7. Mammalian and Bird Circulation
Mammals, birds, and crocodiles have a four-chambered heart that is really two separate pumping systems operating together within a single unit. One of these pumps blood to the lungs, while the other pumps blood to the rest of the body. The left side has two connected chambers, and so does the right, but the two sides are not connected with one another. The increased efficiency of the double circulatory system in mammals and birds is thought to have been important in the evolution of endothermy (warm-bloodedness), because a more efficient circulation is necessary to support the high metabolic rate required.
Circulation Through the Heart
Let’s follow the journey of blood through the mammalian heart in figure 23.13a, starting with the entry of oxygen-rich blood into the heart from the lungs. Oxygenated blood (the pink arrows) from the lungs enters the left side of the heart (which is on the right as you look at the figure), emptying directly into the left atrium through large vessels called the pulmonary veins. From the atrium, blood flows through an opening into the adjoining chamber, the left ventricle. Most of this flow, roughly 70%, occurs while the heart is relaxed. When the heart starts to contract, the atrium contracts first, pushing the remaining 30% of its blood into the ventricle.
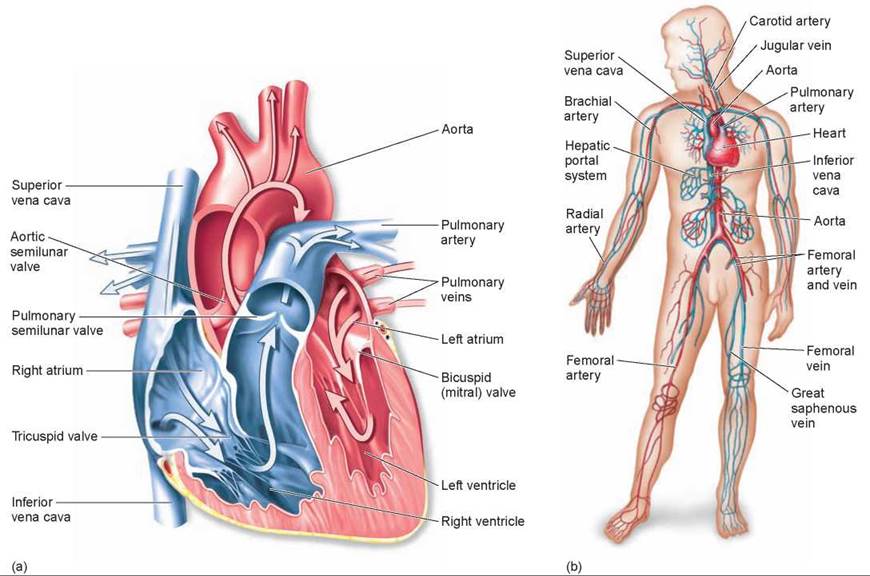
Figure 23.13. The heart and circulation of mammals and birds.
(a) Unlike the amphibian heart, this heart has a septum dividing the ventricle into left and right ventricles. Oxygenated blood from the lungs enters the left atrium of the heart by way of the pulmonary veins. This blood then enters the left ventricle, from which it passes into the aorta to circulate throughout the body and deliver oxygen to the tissues. When gas exchange has taken place at the tissues, veins return blood to the heart. After entering the right atrium by way of the superior and inferior venae cavae, deoxygenated blood passes into the right ventricle and then through the pulmonary valve to the lungs by way of the pulmonary artery. (b) Some of the major arteries and veins in the human circulatory system are shown.
After a slight delay, the ventricle contracts. The walls of the ventricle are far more muscular than those of the atrium (as seen in this cross section), and thus this contraction is much stronger. It forces most of the blood out of the ventricle in a single strong pulse. The blood is prevented from going back into the atrium by a large, one-way valve, the bicuspid (mitral) valve, or left atrioventricular valve, whose two flaps are pushed shut as the ventricle contracts.
Prevented from reentering the atrium, the blood within the contracting left ventricle takes the only other passage out (partially covered by the large blue vessel in the figure). It moves through a second opening that leads into a large blood vessel called the aorta. The aorta is separated from the left ventricle by a one-way valve, the aortic semilunar valve. The aortic valve is oriented to permit the flow of the blood out of the ventricle. Once this outward flow has occurred, the aortic valve closes, preventing the reentry of blood from the aorta into the heart. The aorta and its many branches are systemic arteries and carry oxygen-rich blood to all parts of the body.
Eventually, this blood returns to the heart after delivering its cargo of oxygen to the cells of the body. In returning, it passes through a series of progressively larger veins, ending in two large veins that empty into the right atrium of the heart. The superior vena cava drains the upper body (extending from the heart to the top of the figure), and the inferior vena cava drains the lower body (extending from the heart downward).
The right side of the heart is similar in organization to the left side. Blood (the blue-colored arrows) passes from the right atrium into the right ventricle through a one-way valve, the tricuspid valve or right atrioventricular valve. It passes out of the contracting right ventricle through a second valve, the pulmonary semilunar valve, into the pulmonary arteries, which carry the deoxygenated blood to the lungs. The blood then returns from the lungs to the left side of the heart with a new cargo of oxygen, which is pumped to the rest of the body. Figure 23.13b shows the major veins and arteries in the human body. Veins carry blood to the heart and arteries carry blood away from the heart.
Because the overall circulatory system is closed, the same volume of blood must move through the pulmonary circulation as through the much larger systemic circulation with each heartbeat. Therefore, the right and left ventricles must pump the same amount of blood each time they contract. If the output of one ventricle did not match that of the other, fluid would accumulate and pressure would increase in one of the circuits. The result would be increased filtration out of the capillaries and edema (as occurs in congestive heart failure, for example). Although the volume of blood pumped by the two ventricles is the same, the pressure they generate is not. The left ventricle, which pumps blood through the systemic pathway, is more muscular and generates more pressure than the right ventricle.
The evolution of multicellular organisms has depended critically on the ability to circulate materials throughout the body efficiently. Vertebrates carefully regulate the operation of their circulatory systems and are able to integrate their body activities. Indeed, the metabolic demands of different vertebrates have shaped the evolution of circulatory systems.
Monitoring the Heart's Performance
The simplest way to monitor heartbeat is to listen to the heart at work, using a stethoscope. The first sound you hear, a low-pitched lub, is the closing of the bicuspid and tricuspid valves at the start of ventricular contraction. A little later, you hear a higher-pitched dub, the closing of the pulmonary and aortic valves at the end of ventricular contraction. If the valves are not closing fully, or if they open incompletely, a turbulence is created within the heart. This turbulence can be heard as a heart murmur, a liquid sloshing sound.
A second way to examine the events of the heartbeat is to monitor the blood pressure. This is done using a device called a sphygmomanometer, which measures the blood pressure in the brachial artery found on the inside part of the arm, at the elbow (figure 23.14). A cuff wrapped around the upper arm is tightened enough to stop the flow of blood to the lower part of the arm 1. As the cuff is loosened, blood begins pulsating through the artery and can be detected using a stethoscope. Two measurements are recorded: The systolic pressure 2 is recorded when a pulse is heard, and the diastolic pressure 3 is recorded when the pressure in the cuff is so low that the sound stops.
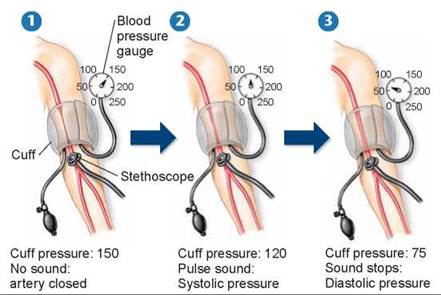
Figure 23.14. Measuring blood pressure.
The blood pressure cuff is tightened to stop the blood flow through the brachial artery 1. As the cuff is loosened, the systolic pressure is recorded as the pressure at which a pulse is heard through a stethoscope 2. The diastolic pressure is recorded as the pressure at which a sound is no longer heard 3.
To understand these measurements it is important to remember what is happening in the heart. During the first part of the heartbeat, the atria are filling. At this time the pressure in the arteries leading from the left side of the heart out to the tissues of the body decreases slightly. This low pressure is referred to as the diastolic pressure. During the contraction of the left ventricle, a pulse of blood is forced into the systemic arterial system, immediately raising the blood pressure within these vessels. The high blood pressure produced in this pushing period, which ends with the closing of the aortic valve, is referred to as the systolic pressure. Normal blood pressure values are 70 to 90 diastolic and 110 to 130 systolic. When the inner walls of the arteries accumulate fats, as they do in the condition known as atherosclerosis, the diameters of the passageways are narrowed. If this occurs, the systolic blood pressure is elevated.
How the Heart Contracts
Throughout the evolutionary history of the vertebrate heart, the sinus venosus has served as a pacemaker, the site where the impulses that produce the heartbeat originate. Although it constitutes a major chamber in the fish heart, it is reduced in size in amphibians and further reduced in reptiles. In mammals and birds, the sinus venosus is no longer a separate chamber, but some of its tissue remains in the wall of the right atrium, near the point where the systemic veins empty into the atrium. This tissue, which is called the sinoatrial (SA) node (indicated in panel 1 of figure 23.15), is still the site where each heartbeat originates.
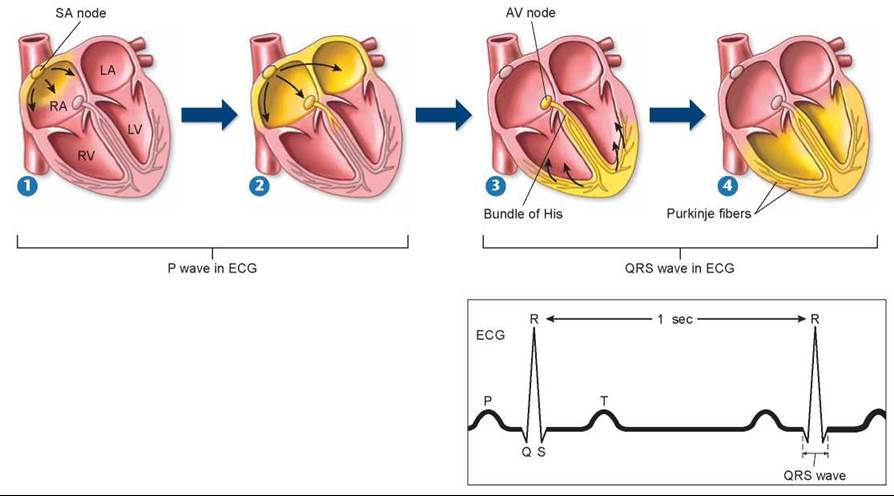
Figure 23.15. How the mammalian heart contracts.
1 Contraction of the mammalian heart is initiated by an electrical signal (yellow highlighting) that begins at the SA node. The electrical activity of the heart can be recorded on an electrocardiogram (ECG or EKG), shown to the right. 2 After passing over the right and left atria and causing their contraction (forming the P wave on the ECG), 3 the signal reaches the AV node, from which it passes to the ventricles by the bundle of His. 4 The signal is then conducted rapidly over the surface of the ventricles by a set of finer fibers called Purkinje fibers, causing the ventricles to contract (forming the QRS wave on the ECG). The T wave on the ECG corresponds to the relaxation of the ventricles. This ECG is showing a heart rate of 60 beats per minute. The time between peaks varies with changes in heart rates.
The contraction of the heart consists of a carefully orchestrated series of muscle contractions. First, the atria contract together, followed by the ventricles. Contraction is initiated by the sinoatrial (SA) node. Its membranes spontaneously depolarize (that is, admit ions that cause it to become more positively charged), creating electrical signals with a regular rhythm that determines the rhythm of the heart’s beating. In this way, the SA node acts as a pacemaker for the heart. Each electrical signal initiated within this pacemaker region passes quickly from one heart muscle cell to another in a wave that envelops the left and the right atria almost simultaneously (indicated by the yellow coloring in figure 23.15, panels 1 and 2).
But the electrical signals do not immediately spread to the ventricles. There is a pause before the lower half of the heart starts to contract. The reason for the delay is that the atria of the heart are separated from the ventricles by connective tissue that does not propagate the electrical signal. The signal would not pass to the ventricles at all except for a slender connection of cardiac muscle cells known as the atrioventricular (AV) node (labeled in panel 3), which connects across the gap to a strand of specialized muscle known as the atrioventricular bundle, or bundle of His. Bundle branches divide into fast-conducting Purkinje fibers, which initiate the almost simultaneous contraction of all the cells of the right and left ventricles about 0.1 seconds after the atria contract. This delay permits the atria to finish emptying their contents into the corresponding ventricles before those ventricles start to contract. The contraction of the ventricles begins at the apex (the bottom of the heart) where depolarization of Purkinje fibers begins the electrical signal. The contraction then spreads up toward the atria (indicated by the yellow coloring in panels 3 and 4). This results in a “wringing out” of the ventricle, forcing the blood up and out of the heart.
Because the vertebrate body basically consists of water, it conducts electrical currents rather well. The electrical signal passing over the surface of the heart generates an electrical current that passes in a wave throughout the body. The magnitude of this electrical pulse is tiny, but it can be detected by sensors placed on the skin. The recording, called an electrocardiogram (ECG or EKG), shows how the cells of the heart respond electrically during the cardiac cycle (figure 23.15). A cardiac cycle consists of one sequence of contraction and relaxation of the heart. The first peak in the recording, P, is produced by the electrical activity of the atria. The second, larger peak, QRS, is produced by ventricular stimulation; during this time, the ventricles contract and eject blood into the arteries. The last peak, T, reflects ventricular relaxation.
Key Learning Outcome 23.7. The mammalian heart is a two-cycle pump. The left side pumps oxygenated blood to the body's tissues, while the right side pumps O2-depleted blood to the lung. The performance of the heart can be monitored in many ways.
Biology and Staving Healthy
Heart Disease Will Kill Many of Us
Heart disease and other diseases of the circulatory system are the leading cause of death in the United States, accounting for nearly 35% of all deaths in 2005. More than 80 million Americans have some form of cardiovascular disease. Heart attacks, the main killers, result from an insufficient supply of blood reaching one or more parts of the heart muscle, which causes myocardial cells in those parts to die. Heart attacks, also called myocardial infarctions, are often caused by a blood clot forming somewhere in the coronary arteries (the arteries that supply the heart muscle with blood); like a rock stuck in a pipe, the clot blocks the passage of blood through the artery to the muscles of the heart. Without blood-borne oxygen, the affected cardiac muscles are damaged and the heart ceases to function properly. If enough cardiac muscle is affected, the heart stops beating altogether and the individual dies.
A heart attack may also result if a coronary artery is blocked by atherosclerosis (discussed later). Recovery from a heart attack is possible if the portion of the heart that was damaged is small. Angina pectoris, which literally means "chest pain,” can occur when the supply of blood to the heart is reduced. The pain may occur in the heart and often also in the left arm and shoulder. Angina pectoris is a warning sign that the blood supply to the heart is inadequate but still sufficient to avoid myocardial cell death.
Strokes are caused by an interference with the blood supply to the brain. They may occur when a blood vessel bursts in the brain or when blood flow in a cerebral artery is blocked by a thrombus (blood clot) or by atherosclerosis. The effects of a stroke depend on how severe the damage is and where in the brain the stroke occurs.
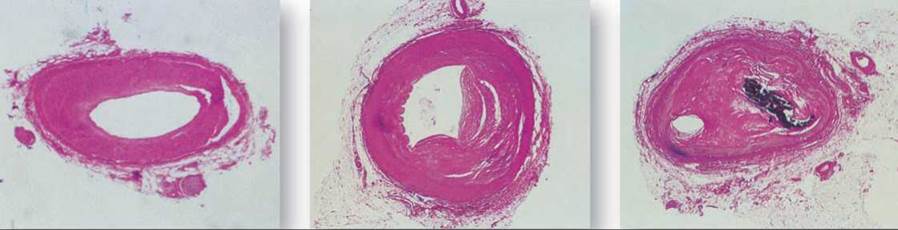
Atherosclerosis is an accumulation within the arteries of fatty materials, abnormal amounts of smooth muscle, deposits of cholesterol or fibrin, or various kinds of cellular debris. These accumulations cause blood flow to be reduced. The lumen (interior) of the artery may be further reduced in size by a clot that forms as a result of the atherosclerosis. Three different coronary arteries are shown below with different degrees of blockage. The coronary artery on the left shows only minor blockage, while the artery you see in the middle exhibits severe atherosclerosis—much of the passage is blocked by buildup on the interior walls of the artery. In the severest cases (as seen on the right), the artery may be blocked completely. Atherosclerosis is promoted by genetic factors, smoking, hypertension (high blood pressure), and high blood cholesterol levels. Diets low in cholesterol and saturated fats (from which cholesterol can be made) can help lower the level of blood cholesterol, and therapy for hypertension can reduce that risk factor. To stop smoking, however, is the single most effective action a smoker can take to reduce the risk of atherosclerosis.
Arteriosclerosis, or hardening of the arteries, occurs when calcium is deposited in arterial walls. It tends to occur when atherosclerosis is severe. Not only do such arteries have restricted blood flow, but they also lack the ability to expand as normal arteries do to accommodate the volume of blood pumped out by the heart. This inflexibility forces the heart to work harder.
Atherosclerosis is treated both with medication and with invasive procedures. Medications include enzymes, which help dissolve clots; anticoagulants, which prevent clots from forming (aspirin works as a weak anticoagulant); and nitroglycerin, which dilates blood vessels. Invasive treatments include reducing the blockage with angioplasty. Angioplasty is a procedure where a small balloon is threaded into a partially blocked coronary artery. Once in the blocked artery, the balloon is inflated, flattening the atherosclerosis deposit against the side of the artery. In some cases, a small metal mesh sleeve called a stent may also be inserted to prop the artery open. More aggressive treatments include coronary bypass surgery, where healthy segments of blood vessels are patched into a coronary artery, which diverts the flow of blood around a blocked section of artery; and heart transplants, where the damaged heart is replaced by a donor heart.
The great tragedy of heart disease is that, like lung cancer, it is largely a lifestyle disease. People who do not smoke have little to fear from lung cancer, and are at much lower risk of developing heart disease. People who exercise regularly and eat a "heart-healthy” low-fat diet tend to have lower blood cholesterol levels and so are far less likely to develop atherosclerosis. Many people with a genetic tendency to overproduce cholesterol can maintain acceptable levels with statin drugs like Lipitor that inhibit the initial enzyme carrying out the body's cholesterol biosynthesis.
Tnquiry & Analysis
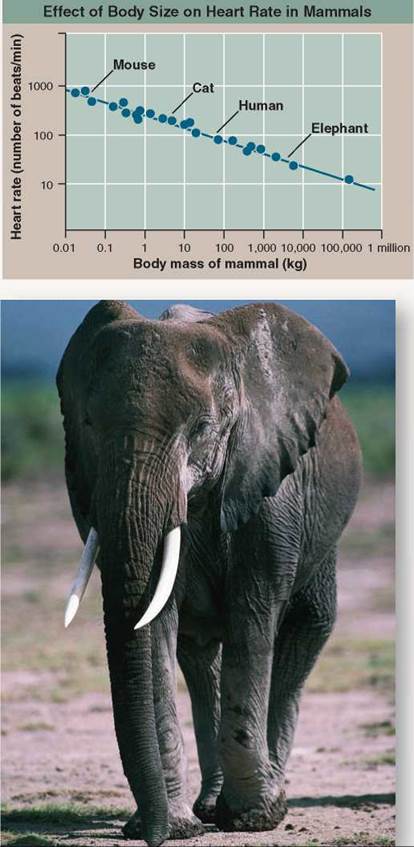
Small animals live at a much faster pace than large animals. They reproduce more quickly and live shorter lives. As a rule, they tend to move about more quickly and so consume more oxygen per unit body weight. Interestingly, small and large mammals have about the same size heart, relative to body size (about 0.6% of body mass). It is interesting to ask whether all mammalian hearts beat at the same rate. The heart of a 7,000-kilogram (a kilogram is 1,000 grams) African bull elephant must push a far greater volume of blood through its body than the heart of a 20-gram mouse, but the elephant is able to do it through much-larger-diameter arteries, which impose far less resistance to the blood's flow. Does the elephant's heart beat faster? Or does the mouse's, in order to deliver more oxygen to its muscles? Or perhaps the mouse's heart beats more slowly because of increased resistance to flow through narrower blood vessels.
The graph to the right displays the pulse rate of a number of mammals of different body sizes (the pulse rate is the number of heartbeats counted per minute, a measure of how rapidly the heart is beating).

1. Applying Concepts
a. Variable. In the graph, what is the dependent variable?
b. Reading a Line Graph. All mammals have the same size hearts relative to their body size. Do their hearts beat at the same rate?
2. Interpreting Data
a. What is the resting pulse rate of a 7,000-kilogram African bull elephant?
b. What is the resting pulse rate of a 20-gram mouse? How many complete heartbeats is that per second?
c. The pulse rate of an adult human at rest is about 70 beats per minute, while the heart of a cat, with a body weight less than a tenth of humans, beats 120 times per minute, almost twice as fast. What general statement can be made regarding the effect of body size on heart rate in mammals?
3. Making Inferences
a. The data in the graph, plotted on logarithmic coordinates (that is, the scale rises in powers of 10), fall nicely upon a straight line. How would you expect them to look, plotted on linear coordinates?
b. As you walk through the graph from left to right, the line slopes down; this is called a negative slope. What does the negative slope of the line signify?
4. Drawing Conclusions If you plotted data for an experiment measuring body mass versus resting oxygen consumption, you would get exactly the same slope of the line as shown in this graph. What does this tell us about why body size affects heart rate in mammals as it does?
5. Further Analysis What would you expect to be the relationship between lung size and body mass in mammals? Explain your reasoning.
1. Which of the following is not a function of the circulatory system?
a. regulation of body temperature
b. protection against injury, foreign toxins, and microbes
c. transportation of materials in the body
d. All of the above are functions of the circulatory system.
2. How do some vertebrates maintain body temperature in cold environments?
a. by mixing cold blood with warm blood in the heart
b. by pumping more warm blood to the extremities
c. by passing warm blood near cold blood in the extremities to warm the blood
d. All of the above are used by vertebrates in cold environments.
3. Exchange of waste material, oxygen, carbon dioxide, and metabolites such as salts and food molecules, takes place in the
a. capillaries.
b. venules.
c. arterioles.
d. arteries.
4. The lymphatic system is like the circulatory system in that they both
a. have nodes that filter out pathogens.
b. are made up of arteries.
c. deliver blood to the heart.
d. carry fluids.
5. The most numerous type of blood cell is the
a. macrophage.
b. leukocyte.
c. platelet.
d. erythrocyte.
6. What advancement in fish led to a more efficient circulatory system?
a. A muscular pump is first seen in fishes.
b. A closed circulatory system is first seen in fishes.
c. A heart with separate chambers is first seen in fishes.
d. A double-loop system is first seen in fishes.
7. Additional septa in the amphibian and reptile heart allow for
a. higher blood pressure to move blood faster.
b. better separation of oxygenated and deoxygenated blood.
c. better body temperature regulation.
d. better transport of food to needy tissues.
8. Which of the following statements is false?
a. Only arteries carry oxygenated blood.
b. Both arteries and veins have a layer of smooth muscle.
c. Capillary beds lie between arteries and veins.
d. Sphincters regulate the flow of blood through capillaries.
9. The four-chambered heart and double-loop vessel system are thought to be important in the evolution of
a. locomotion.
b. ectothermy.
c. exothermy.
d. endothermy.
10. High blood pressure can be detected using
a. a stethoscope.
b. an ECG.
c. a sphygmomanometer.
d. All of the above.